Does PE count for CHADS2 VASc
Specifically, the ARISTOTLE trial defined sys- temic embolism as requiring “a clinical history consistent with an acute loss of blood flow to a peripheral artery (or arteries) supported by the evidence of embolism from surgical specimens, autopsy, angiography, vascular imaging, or other objective testing.”4 By these …
What is the Chadsvasc scale?
CHADSVASC is a long acronym that refers to the various factors influencing your risk of stroke as an AFib patient. Specifically, your CHADSVASC score runs on a sliding scale from 0-10, and is made up of the following factors: Congestive Heart Failure (one point) High blood pressure (one point)
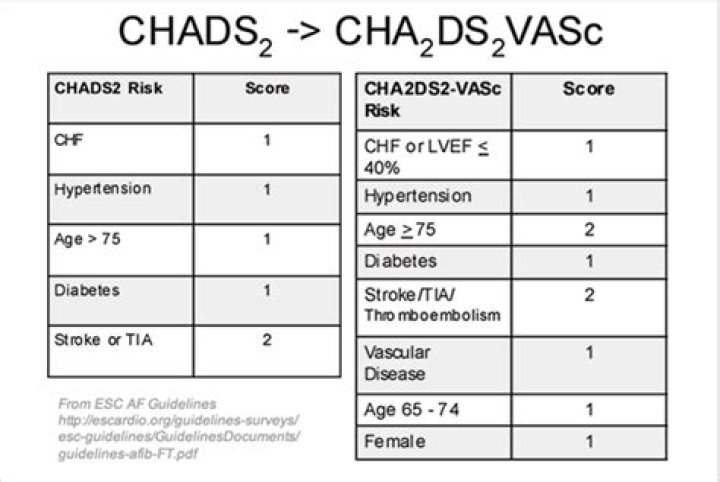
What is the difference between CHADS2 and CHA2DS2-VASc?
Conclusions: The C-statistic suggests a similar clinical utility of the CHADS2 and CHA2DS2-VASc scores in predicting stroke and thromboembolism, but CHA2DS2- VASc has the important advantage of identifying extremely low-risk patients with atrial fibrillation, as well as classifying a lower proportion of patients as …
Is AFib considered CAD?
Coronary artery disease (CAD) is the most common cardiovascular disease while atrial fibrillation (AF) is the most common cardiac arrhythmia. Both diseases share associated risk factors – hypertension, diabetes mellitus, sleep apnea, obesity and smoking. Moreover, inflammation plays a causative role in both diseases.Is BLED score high risk?
The HAS-BLED scores range from 0 to 9, with scores of ≥3 indicating high risk of bleeding, for which caution and regular review of the patient are recommended.
What is valvular AFib?
AFib is considered valvular when it’s seen in people who have a heart valve disorder or a prosthetic heart valve. Nonvalvular AFib generally refers to AFib caused by other things, such as high blood pressure or stress. There’s still some debate over how exactly to define valvular AFib.
Does AFib cause VTE?
Conclusions. The occurrence of AF was associated with increased risk of incident VTE, and occurrence of VTE was associated with greater risk of incident AF. Associations were particularly strong among blacks, and during the first 6 months after the initial diagnosis, though they remained elevated even after 6 months.
Can CAD cause atrial flutter?
Atrial flutter is often caused by another heart condition, such as coronary artery disease or another heart rhythm problem. It may happen after heart surgery.When do you Anticoagulate AFib?
Based on these observations, it is generally recommended that anticoagulation be instituted for three weeks before cardioversion is attempted in patients with AF of more than two days’ duration. To minimize thromboembolic complications, anticoagulants should be continued for four weeks after cardioversion.
Does CAD cause arrhythmia?Over time, CAD can weaken the heart muscle and lead to heart failure and arrhythmias.
Article first time published onIs AFib considered heart disease Yes or no?
Atrial fibrillation (AF) is a common heart rhythm condition that can cause stroke and heart failure. Read about AF symptoms, causes, risk factors and common triggers. You can also learn about treatment and find ways to manage your condition.
What Chadsvasc score is high risk?
As for level of risk, a CHADS2 score of 0 is considered low risk; a 1 or 2, moderate risk; and higher than 2 was indicative of high risk.
What is a CHADS2 score in cardiology?
The CHADS 2 score is a system used to predict the risk of thromboembolic stroke in patients with atrial fibrillation helping to guide to use of anticoagulation to prevent stroke.
What does a CHADS2 score of 2 mean?
2 points. Stroke/Transient Ischemic Attack/Thromboembolic event. 1 point. Vascular disease (prior heart attack, peripheral artery disease, or aortic plaque)
HAS-BLED scored aspirin?
The HAS-BLED score also makes clinicians think about the potentially reversible risk factors for bleeding, e.g. uncontrolled blood pressure (the H in HAS-BLED), labile INRs if on warfarin (the L in HAS-BLED) and concomitant use of aspirin/NSAIDs (the D in HAS-BLED).
What can cause increased INR?
- Too much anticoagulant medicine, a type of blood thinner that helps prevent clots.
- Other medicines, such as aspirin, NSAIDs, and some antibiotics, when you also are using anticoagulants.
- Health conditions, such as liver failure or bleeding disorders.
Is HAS-BLED only for warfarin?
HAS-BLED bleeding risk score – UpToDate. The HAS-BLED bleeding risk score has only been validated in patients with atrial fibrillation receiving warfarin.
What is the main difference between atrial fibrillation and atrial flutter?
In atrial fibrillation, the atria beat irregularly. In atrial flutter, the atria beat regularly, but faster than usual and more often than the ventricles, so you may have four atrial beats to every one ventricular beat.
Does AFIB increase risk of PE?
Epidemiological studies indicate that AF can be seen as a presenting sign, during the early phase, or later in the course of recovery from PE. Patients with AF are also at increased risk of developing PE, a risk that correlates with the CHA2DS2-VASc score.
What is an appendage of the heart?
The left atrial appendage (LAA) is a small, ear-shaped sac in the muscle wall of the left atrium (top left chamber of the heart).
What is considered valvular disease?
Valvular heart disease is when any valve in the heart has damage or is diseased. There are several causes of valve disease. The normal heart has four chambers (right and left atria, and right and left ventricles) and four valves (Figure 1).
What is a flutter in the heart?
Atrial flutter is a type of abnormal heart rhythm, or arrhythmia. It occurs when a short circuit in the heart causes the upper chambers (atria) to pump very rapidly.
Do leaky heart valves cause AFib?
Left untreated, leaky heart valves can cause serious complications, including heart failure, atrial fibrillation (irregular heartbeat) or pulmonary hypertension (high blood pressure in the lung’s vessels).
Do you Anticoagulate for atrial flutter?
Most patients with atrial flutter should be considered for chronic anticoagulation in a manner similar to those with atrial fibrillation (AF). This recommendation is based not only on the fact atrial flutter carries a risk for systemic embolization but also that these patients usually have episodes of AF.
Do you Anticoagulate for paroxysmal AFib?
American College of Chest Physicians recommended that anticoagulation be consid- ered for all patients with atrial fibrillation, whether it be chronic or paroxysmal.
Which anticoagulant is best for atrial fibrillation?
Non-vitamin K oral anticoagulants (NOACs), are now recommended as the preferred alternative to warfarin for reducing the risk of stroke associated with atrial fibrillation (AFib), according to the 2019 AHA/ACC/HRS Focused Update of the 2014 AHA/ACC/HRS Guideline for the Management of Patients with Atrial Fibrillation …
Does ablation weaken the heart?
“Because ablations irritate and inflame the heart a little, many patients experience short runs of arrhythmia in the weeks afterward,” Dr. Arkles says. In other words, the weeks after an ablation shouldn’t be used to determine whether the procedure was a success – though more often than not, it is.
Can anxiety cause AFIB symptoms?
Tackle stress, anxiety and depression to benefit your heart. Stress can contribute to heart rhythm disorders (arrhythmias) such as atrial fibrillation. Some studies suggest that stress and mental health issues may cause your atrial fibrillation symptoms to worsen.
How do you know if your heart is fluttering?
What does a heart flutter or palpitation feel like? These sensations usually aren’t painful, but they sure do feel strange. You may feel like your heartbeat is fluttering or like your heart skipped a beat. You may also experience a pounding sensation from a racing heartbeat or a slow heartbeat.
Does CAD cause tachycardia?
Arrhythmias that can develop in people with CAD include, but are not limited to, the following: bradycardia, a slow heart rate. tachycardia, a fast heart rate. atrial fibrillation, a chaotic, irregular rhythm in the top chambers of the heart (atria)
Can CAD cause SVT?
Coronary artery disease, other heart problems and previous heart surgery. Narrowed heart arteries, a heart attack, abnormal heart valves, prior heart surgery, heart failure, cardiomyopathy and other heart damage increase your risk of developing SVT .