Does supine position increase ICP
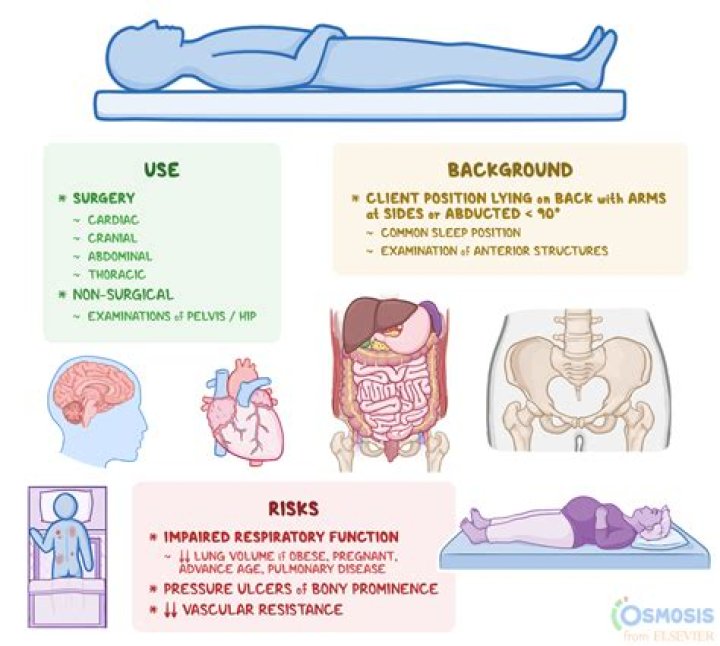
At rest, compared with the reference 30-degree head-up position, the supine position increased ICP by 621 mm Hg (P<. 01) and increased CPP by 3+1 mm Hg (P<. 05). At rest, further head elevation from 30 to 45 degrees did not affect ICP but decreased CPP by 651 mm Hg (P<.
Does ICP increase when lying down?
Pressures in the skull are higher when patients are lying down than when sitting or standing, and there is strong evidence that this difference between pressures when lying and sitting is higher in patients with a working shunt, and lower in patients without a shunt.
What positions should I avoid with ICP?
Head elevation above 30 degrees should be avoided in all cases. In most patients with intracranial hypertension, head and trunk elevation up to 30 degrees is useful in helping to decrease ICP, providing that a safe CPP of at least 70 mmHg or even 80 mmHg is maintained.
What positions increase ICP?
However, ICP is generally significantly higher when the patient is in the horizontal position. This study was undertaken to clarify the issue of optimal head position in the care of head-injured patients.Does prone position increase ICP?
Conclusions: The prone position can be used to improve the oxygenation as well as CPP in patients with traumatic brain injury or SAH. However, this method results in raised ICP, and should be used cautiously in patients with reduced intracranial compliance.
What causes increased ICP?
Increased ICP can result from bleeding in the brain, a tumor, stroke, aneurysm, high blood pressure, or brain infection. Treatment focuses on lowering increased intracranial pressure around the brain. Increased ICP has serious complications, including long-term (permanent) brain damage and death.
What causes pressure in your head when you lay down?
The most common causes of pressure in the head are tension headaches and sinus headaches. Both of these conditions respond well to treatments. In rare cases, pressure in the head is a sign of a more serious condition. If the issue persists, you should see your doctor.
What position is best for head injury?
- Ideally, head up 45 degrees. …
- It seems to position the patient at least 30° head up decreases the ICP but does not decrease the CPP.
- At least in the pediatric population, the angle of the bed is directly related to intracranial pressure.
- Ideally, the C-spine collar should be removed.
How does body position affect ICP?
It has been shown that ICP (i.e., CSF pressure in the ventricles) is reduced when moving from a supine to an upright position, whereas CSF pressure at the lumbar level of the spinal subarachnoid space increases, and it has been hypothesized that there exists a hydrostatic indifference point in the CSF system as well ( …
Which is the best position for a patient to maintain optimum intracranial pressure?If adequate cerebral perfusion pressure is considered more desirable than the absolute level of ICP, the horizontal position is optimal for these patients.
Article first time published onHow do you control increased intracranial pressure?
Medical options for treating elevated ICP include head of bed elevation, IV mannitol, hypertonic saline, transient hyperventilation, barbiturates, and, if ICP remains refractory, sedation, endotracheal intubation, mechanical ventilation, and neuromuscular paralysis.
How can I increase my cerebral perfusion?
Maintaining an adequate cerebral perfusion pressure is achieved by lowering the intracranial pressure and supporting the mean arterial blood pressure through fluid resuscitation and direct-acting vasoconstrictors.
What measure helps lower intracranial pressure?
Hyperventilation to moderate levels (PaCO2 = 25-35) is generally considered a short-term temporizing measure to decrease ICP.
Is prone position safe?
Prone positioning is not a benign procedure, and there are potential risks (complications) that can occur to both the patient and the health care worker. Notable complications that can arise include: unplanned extubation, lines pulled, tubes kinked, and back and other injuries to personnel.
What happens if ICP is too high?
A sudden increase in the pressure inside a person’s skull is a medical emergency. Left untreated, an increase in the intracranial pressure (ICP) may lead to brain injury, seizure, coma, stroke, or death. With prompt treatment, it is possible for people with increased ICP to make a full recovery.
Does stress increase ICP?
Because anxiety can make increased ICP worse by raising your blood pressure, you may receive a sedative as well. Less common treatments for increased ICP include: removing part of the skull.
What are the late signs of raised ICP?
The Answer Seizure. Late signs of intracranial pressure that comprise Cushing triad include hypertension with a widening pulse pressure, bradycardia, and abnormal respiration. The presence of those signs indicates very late signs of brain stem dysfunction and that cerebral blood flow has been significantly inhibited.
How can I increase my CSF flow?
These techniques include massage and manipulation of the spine. Walking, stretching, cycling, heat, and yoga may all help SFF.
What are the four stages of increased intracranial pressure?
Intracranial hypertension is classified in four forms based on the etiopathogenesis: parenchymatous intracranial hypertension with an intrinsic cerebral cause, vascular intracranial hypertension, which has its etiology in disorders of the cerebral blood circulation, meningeal intracranial hypertension and idiopathic …
What is Fowler's and supine?
Fowler’s position is commonly used for shoulder arthroscopy procedures. Surgical tables may be articulated to place patients in a seated position or shoulder chair (beach chair) accessories may be used as an alternative. The patient is placed supine on the operating table and general endotracheal anesthesia is induced.
Which body position should be used for the patient with the symptoms of perfusion?
Conclusions: The best SPP values were obtained in Position III, which is the ideal position for peripheral arterial circulation in patients with severe PAD.
Is CSF pressure same as intracranial pressure?
Intracranial pressureTypesIncreased, normal, decreased
Do you elevate head of bed with head injury?
Besinger: The head of the bed should be elevated, ideally to 30 to 45 degrees. There are a couple of good reasons for doing that. First and most important, it decreases intracranial pressure. That’s extremely important for the patient with a severe head injury.
What is the normal value of ICP?
For the purpose of this article, normal adult ICP is defined as 5 to 15 mm Hg (7.5–20 cm H2O). ICP values of 20 to 30 mm Hg represent mild intracranial hypertension; however, when a temporal mass lesion is present, herniation can occur with ICP values less than 20 mm Hg [5].
How do you manage head injury emergencies?
Serious or traumatic brain injuries, often requires emergency care, such as surgery to remove blood clots and relieve the pressure of the brain. Minor head injuries will be treated and observed by its symptoms that may include pain medication of headache and medications for nausea and vomiting.
How does mannitol work for ICP?
Mannitol lowers ICP through two distinct effects in the brain. The first, rheological effect, reduces blood viscosity, and promotes plasma expansion and cerebral oxygen delivery. In response, cerebral vasoconstriction occurs due to autoregulation, and cerebral blood volume is decreased.
Does hyperventilation cause vasoconstriction?
Hyperventilation promotes hypocapnia, which causes vasoconstriction in the cerebral arterioles and thus reduces cerebral blood flow and, to a lesser extent, cerebral blood volume effectively, decreasing temporarily intracranial pressure.
What is Decerebrate posturing?
Decerebrate posture is an abnormal body posture that involves the arms and legs being held straight out, the toes being pointed downward, and the head and neck being arched backward. The muscles are tightened and held rigidly. This type of posturing usually means there has been severe damage to the brain.
How does propofol decrease ICP?
We increase propofol if EEG derived parameters do not indicate a deep suppression of metabolism. The metabolism reduction induces a fall of cerebral blood flow (metabolic coupling) and therefore an ICP reduction. In many patients, this optimization of sedation is sufficient for controlling ICP.
When a patient's ICP increases what must the map do in order to maintain adequate CPP?
To achieve adequate CPP, clinicians must balance treating the underlying cause of elevated ICP and appropriately supporting the patient’s blood pressure. Even if the CPP is within acceptable range, elevations in ICP above 20-25 mmHg and/or hypotension should be promptly treated (Smith and Amin-Hanjani, 2019).
How does sedation affect increased ICP?
The effect of sedatives on ICP is due mainly to reduction in CMRO2 that leads to a decrease in cerebral blood flow. This effect can be seen as a decrease in cerebral blood volume that leads to a decrease in ICP. As well, sedation reduces pain and agitation and improves the tolerance to the endotracheal tube.



