How do you assess the severity of a burn
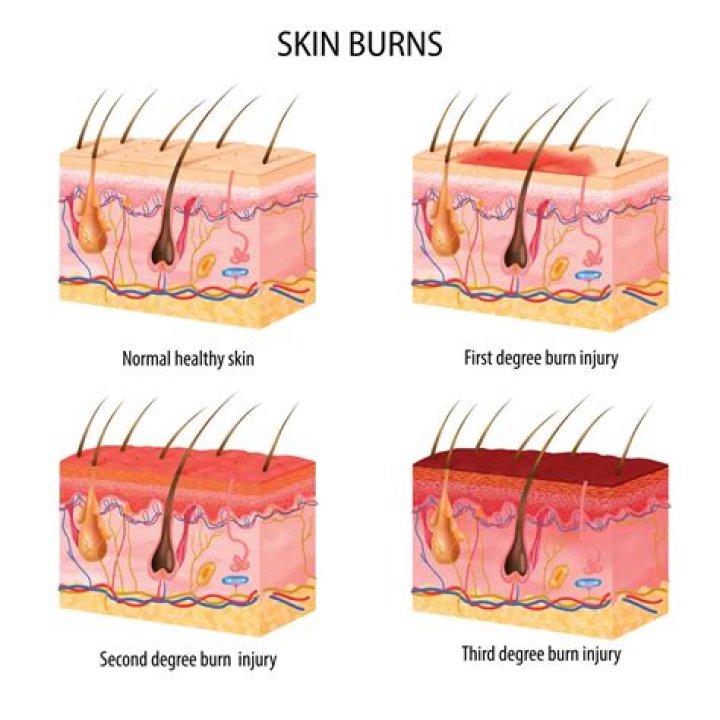
Burn Severity. Severity of burn injury is determined by the depth of injury, extent of body surface injured, location of burn on the body, age of the patient, pre-burn medical history and circumstances or complicating factors (e.g., smoke inhalation, other traumatic injuries).
What are the four ways you assess a burn?
Burn assessment. Assess airway, breathing, circulation, disability, exposure (prevent hypothermia) and the need for fluid resuscitation. Also, assess severity of burns and conscious level [4, 5]. Establish the cause: consider non-accidental injury.
How do you determine burn level?
- First-degree burns affect only the outer layer of the skin. They cause pain, redness, and swelling.
- Second-degree burns affect both the outer and underlying layer of skin. They cause pain, redness, swelling, and blistering. …
- Third-degree burns affect the deep layers of skin.
What are the 3 classifications of the severity of burns?
Burns are classified as first-, second-, or third-degree, depending on how deep and severe they penetrate the skin’s surface.What four 4 things are considered when assessing the severity of burn injuries?
Burn Severity. Severity of burn injury is determined by the depth of injury, extent of body surface injured, location of burn on the body, age of the patient, pre-burn medical history and circumstances or complicating factors (e.g., smoke inhalation, other traumatic injuries).
How are the extent and severity of burns injuries classified?
Burns are classified as first-, second-, third-degree, or fourth-degree depending on how deeply and severely they penetrate the skin’s surface. First-degree (superficial) burns. First-degree burns affect only the outer layer of skin, the epidermis. The burn site is red, painful, dry, and with no blisters.
What defines a severe burn?
Excluding fourth-degree burns, third-degree burns are the most severe. They cause the most damage, extending through every layer of skin.
How do you treat a 3rd degree burn?
- Early cleaning and debriding (removing dead skin and tissue from the burned area). …
- Intravenous (IV) fluids containing electrolytes.
- Intravenous (IV) or oral antibiotics if your child develops an infection.
- Antibiotic ointments or creams.
What are the depths of burns?
Burn depth is classified as first, second, third, or fourth degree, as follows: First-degree burns are usually red, dry, and painful. Burns initially termed first-degree are often actually superficial second-degree burns, with sloughing occurring the next day. Second-degree burns are often red, wet, and very painful.
How do you know if its a third-degree burn?They cause pain, redness, swelling, and blistering. Third-degree burns (full thickness burns) go through the dermis and affect deeper tissues. They result in white or blackened, charred skin that may be numb.
Article first time published onHow are the depth and extent of burns assessed?
The extent of the burn injury is expressed as a percentage of the patient’s total body surface area (TBSA). Superficial (first-degree) burns are not included in percentage TBSA burn assessment. This estimation can be facilitated using a Lund-Browder chart, the Rule of Nines, or the palm method.
What is assessment tool used to assess burns in adults?
It is important to accurately document the location and area of the burn. The recommended tool for assisting in calculating this in adults is the Wallace rule of nines chart, in children the Lund Browder tool is used.
Which assessment is the nurse's highest priority in caring for a patient in the acute phase of burn injury?
Respiratory and fluid status remains highest priority. Assess peripheral pulses frequently for first few days after the burn for restricted blood flow. Closely observe hourly fluid intake and urinary output, as well as blood pressure and cardiac rhythm; changes should be reported to the burn surgeon promptly.
Which of the following factors has the most significant impact on determining the severity of a burn?
One of the most important factors that determines burn severity is how deeply it penetrates beneath the surface of the skin. This is what people are talking about when they describe first-, second- or third-degree burns.
How do you know when a burn is bad?
In general, if the burn covers more skin than the size of the palm of your hand it needs medical attention. Signs of infection. If the pain increases, there is redness or swelling, or liquid or a foul odor is coming from the wound then the burn is likely infected. Worsening over time.
What is the immediate threat from severe burns?
But when faced with large or deep burns, it can overreact, often making the injury more severe and harming the heart, lungs, blood vessels, kidneys, and other organ systems. During this inflammatory response, there is fluid loss that can cause a sharp and potentially deadly drop in blood pressure known as shock.
How is burn extent approximated?
Palm method – Small or patchy burns can be approximated by using the surface area of the patient’s palm. The palm of the patient’s hand, excluding the fingers, is approximately 0.5 percent of total body surface area, and the entire palmar surface including fingers is 1 percent in children and adults [11-13].
How do you measure or estimate the size and extent of the burn area?
The “rule of palm” is another way to estimate the size of a burn. The palm of the person who is burned (not fingers or wrist area) is about 1% of the body. Use the person’s palm to measure the body surface area burned.
How do I know if I have a second-degree burn?
Common symptoms of a 2nd degree burn include a wet, glossy wound, a dark red appearance, blisters, painful and sensitive skin, and a white, discolored appearance to the site of the burn. 2nd degree burns can become more serious if they affect large portions of the body.
What is considered a 2nd degree burn?
What is a second-degree burn? Second-degree burns (also known as partial thickness burns) involve the epidermis and part of the dermis layer of skin. The burn site appears red, blistered, and may be swollen and painful.
Should you keep 3rd degree burns covered?
Treat small burns with over-the-counter topical antibiotic ointment, like Polysporin or Neosporin, until healed. Keep the wound covered with a bandage. Burns heal better in a moist, covered environment.
Why is a third-degree burn traumatic?
Third-degree burns involve damage or complete destruction of the skin to its full depth and damage to underlying tissues. People who experience such burns often require skin grafting. The swelling and blistering characteristic of burns are caused by the loss of fluid from damaged blood vessels.
What are fifth degree burns?
Fifth-degree burn injuries occur when all the skin and subcutaneous tissues are destroyed, exposing muscle. These burns can be fatal due to damage to major arteries and veins. Fifth-degree burn injuries also may require amputation due to damage to muscles.
Is second-degree burn worse than third?
Second-degree burns are more serious burns that affect the outer layer of skin and the next layer, the dermis. They take longer to heal. Third-degree burns are the most serious types of burn. They affect both layers of skin and may also affect other tissue, such as sweat glands.
What percentage of burns is severe?
A severe (major) burn is any burn injury that is complicated by major trauma or inhalation injury, chemical burn, high-voltage electrical burn, and, in general for adults, any burn encompassing over 20 percent of the total body surface area, excluding superficial burns such as sunburn. (See ‘Severe burn injury’ above.)
How is the circulatory system affected by severe burns?
Cardiac stress, mediated by increased catecholamines, is the hallmark of severe burn injury typified by marked tachycardia, increased myocardial oxygen consumption, and increased cardiac output. It remains one of the main determinants of survival in large burns.
How do nurses treat burns?
- Cool the burn. Hold the burned area under cool (not cold) running water or apply a cool, wet compress until the pain eases. …
- Remove rings or other tight items. …
- Don’t break blisters. …
- Apply lotion. …
- Bandage the burn. …
- Take a pain reliever. …
- Consider a tetanus shot.
What nursing measures should be taken to prevent infection of burns?
The followings are the key general measures for preventing the spread infection within burned patients; the implementation of contact precautions (single use masks, gowns, and gloves are worn while in contact with the patient and the hands are washed after finishing contact with the patient), cohort nursing (grouping …
What is Wound Care Management for a burn patient?
Wash the area gently and thoroughly with mild soap and water. Use a small amount of antibiotic ointment and a nonstick dressing and allow the wound to heal. If the surrounding area becomes red and warm, you might have an infection. Contact your health care provider for further evaluation.
Which is a major initial concern for a person that has experienced a severe skin burn?
Infection is also a major concern. Burns damage the skin’s protective barrier, meaning bacteria and other foreign invaders can sneak in. Burns also weaken the immune system, so the body is less able to fight off threats.