How do you code venous stasis
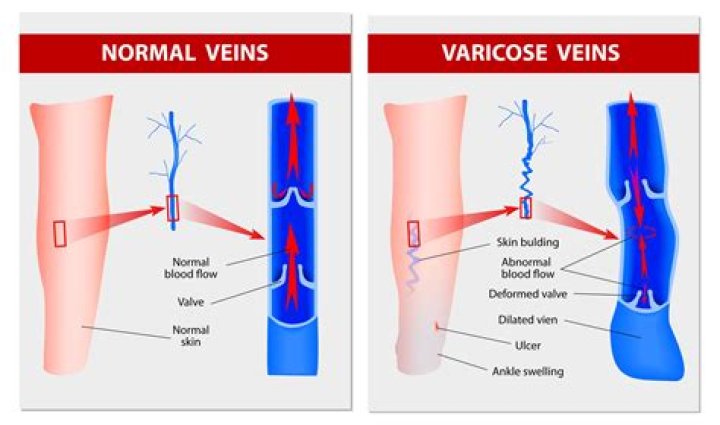
You can confirm the correct code category by looking up the term “Ulcer, stasis (venous)” in the alphabetic index. It directs you to “see Varix, leg, with ulcer,” which has the subterm “without varicose veins,” which specifies code I87.
Is venous and stasis ulcer the same?
Venous ulcer, also known as stasis ulcer, is the most common etiology of lower extremity ulceration, affecting approximately 1 percent of the U.S. population.
Is a venous stasis ulcer a pressure ulcer?
Yes. Venous skin ulcers are caused by poor circulation in the legs caused by damaged valves that prevent blood from flowing the wrong way, allowing blood to pool in the legs. Pressure ulcers, on the other hand, are caused by sustained pressure on an area of the body, which cuts off blood flow.
What is a venous stasis?
Venous stasis involves an inflammation of the skin in the lower legs as a result of chronic venous insufficiency. If the valves or walls of the veins in the legs are not working properly, it is difficult for blood to circulate from the legs back to the heart.What are venous leg ulcers?
Venous ulcers are leg ulcers caused by problems with blood flow (circulation) in your leg veins. Normally, when you get a cut or scrape, your body’s healing process starts working to close the wound. In time, the wound heals.
How is venous ulcer diagnosed?
Arterial pulse examination and measurement of ankle-brachial index are recommended for all patients with suspected venous ulcers. Color duplex ultrasonography is recommended in patients with venous ulcers to assess for venous reflux and obstruction.
What is the ICD 10 code for PVD?
Peripheral vascular disease, unspecified 9 became effective on October 1, 2021. This is the American ICD-10-CM version of I73. 9 – other international versions of ICD-10 I73.
What is the cause of venous stasis ulcer?
What causes venous skin ulcers? Venous skin ulcers are caused by poor blood circulation from the legs, such as from venous insufficiency. Your veins have one-way valves that keep blood flowing toward the heart. In venous insufficiency, the valves are damaged, and blood backs up and pools in the vein.How do you describe a venous stasis ulcer?
A venous stasis ulcer is wound on the skin. It is due to a pooling of blood in the veins. These ulcers happen most often on the legs. If left untreated, the ulcers can lead infection and other serious problems.
What is venous stasis retinopathy?Venous stasis retinopathy is an uncommon sign of carotid artery obstruction. It is found in those patients who have very severe stenosis, or complete occlusion, of the arterial lumen. Affected patients usually have advanced multivessel disease with compromise of both carotid arteries.
Article first time published onWhat is the difference between a venous ulcer and an arterial ulcer?
Arterial ulcers develop as the result of damage to the arteries due to lack of blood flow to tissue. Venous ulcers develop from damage to the veins caused by an insufficient return of blood back to the heart. Unlike other ulcers, these leg wounds can take months to heal, if they heal at all.
What are venous ulcers briefly describe the risk factors for venous leg ulcers?
A venous leg ulcer can develop after a minor injury if there’s a problem with the circulation of blood in your leg veins. If this happens, pressure inside the veins increases. This constant high pressure can gradually damage the tiny blood vessels in your skin and make it fragile.
What is the decubitus ulcer?
Listen to pronunciation. (deh-KYOO-bih-tus UL-ser) Damage to an area of the skin caused by constant pressure on the area for a long time. This pressure can lessen blood flow to the affected area, which may lead to tissue damage and tissue death.
Where are venous stasis ulcers located?
Commonly located on the ankle or calf, venous stasis ulcers are painful and red in color but may be covered with a yellow, fibrous tissue and an irregular border. Drainage and discharge are possible with venous stasis ulcers. This type of ulcer is common in patients with a history of leg swelling or varicose veins.
What are the different types of leg ulcers?
- Venous stasis ulcers.
- Neurotrophic (diabetic)
- Arterial (ischemic ulcers)
How do you treat venous stasis ulcers?
- Wear compression stockings or bandages every day as instructed. …
- Put your feet above your heart as often as possible. …
- Take a walk or exercise every day. …
- Take medicines as directed to help with healing.
What is the ICD 10 code for CVA?
Acute cerebrovascular insufficiency The 2022 edition of ICD-10-CM I67. 81 became effective on October 1, 2021. This is the American ICD-10-CM version of I67.
Is PAD and PVD the same?
Peripheral artery disease (PAD) is often used interchangeably with the term “peripheral vascular disease (PVD).” The term “PAD” is recommended to describe this condition because it includes venous in addition to arterial disorders.
Is atherosclerosis the same as PVD?
The term can include any disorder that affects any blood vessels. It is, though, often used as a synonym for peripheral artery disease. PVD is the most common disease of the arteries. The build-up of fatty material inside the vessels, a condition called atherosclerosis or hardening of the arteries, is what causes it.
What should be included in the documentation of a venous stasis ulcer?
Document wound size, appearance, location, condition of surrounding skin, presence and characteristics of exudate, and signs and symptoms of infection.
What is the ICD 10 code for stasis dermatitis?
I87. 332 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM I87. 332 became effective on October 1, 2021.
What is retinal vascular occlusion?
Retinal vein occlusion happens when a blood clot blocks the vein. Sometimes it happens because the veins of the eye are too narrow. It is more likely to occur in people with diabetes, and possibly high blood pressure, high cholesterol levels, or other health problems that affect blood flow.
Is retinopathy a disease?
Retinopathy means disease of the retina. There are several types of retinopathy but all involve disease of the small retinal blood vessels. Signs of retinopathy (see photograph) can be seen when the retina is viewed through the pupil with an ophthalmoscope.
What is the main difference between arterial and venous blood?
Arteries are blood vessels responsible for carrying oxygen-rich blood away from the heart to the body. Veins are blood vessels that carry blood low in oxygen from the body back to the heart for reoxygenation.
What is the difference between venous and arterial?
Arterial blood always flows away from the heart while venous blood flows towards the heart.
How can you tell the difference between arterial and venous insufficiency?
Although arterial and venous insufficiency share many of the same characteristics and symptoms, the two conditions are actually quite different. Venous insufficiency refers to a breakdown in the flow of blood in our veins, while arterial insufficiency stems from poor circulation in the arteries.
What is the appearance of a venous ulcer?
A venous ulcer is typically shallow with irregular sloping edges whereas an arterial ulcer can be deep and has a ‘punched out’ appearance. Venous ulcers are typically ‘wet’ with a moderate to heavy exudate, whereas arterial ulcers are typically ‘dry’ and scabbed.
How is decubitus ulcer diagnosed?
Diagnosis of a Decubitus Ulcer Medical personnel may take samples of the pressure ulcer tissue and fluid to look for bacteria or cancer. They may also do blood cultures, bone scans or other tests depending on the seriousness of the ulcer.
What is the ICD 10 code for sacral decubitus ulcer?
Pressure ulcer of sacral region, unstageable L89. 150 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
What is sacral decubitus ulcer?
Decubitus ulcers are open wounds on the skin, usually found around bony areas of the body, including the sacral region. The sacral region is near the lower back at the bottom of the spine. Ulcers often form in people who are bedridden and are not able to move their bodies.