How do you use a Passy Muir valve
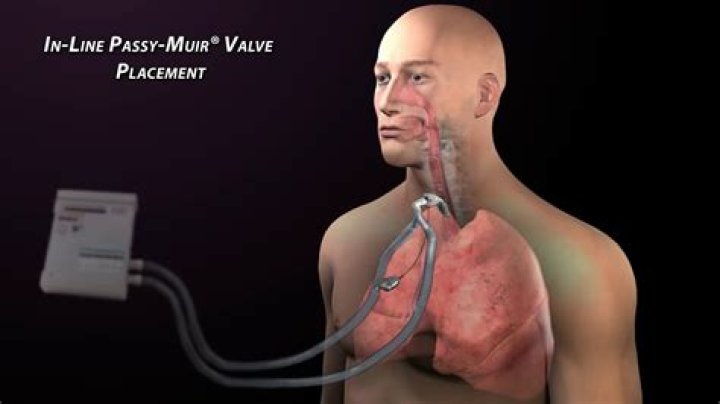
The Passy-Muir speaking valve is commonly used to help patients speak more normally. This one-way valve attaches to the outside opening of the tracheostomy tube and allows air to pass into the tracheostomy, but not out through it. The valve opens when the patient breathes in.
When do you use a Passy Muir valve?
The Passy-Muir speaking valve is commonly used to help patients speak more normally. This one-way valve attaches to the outside opening of the tracheostomy tube and allows air to pass into the tracheostomy, but not out through it. The valve opens when the patient breathes in.
When using a Passy Muir valve What do you need to do with the cuff how about the ventilator?
For in-line Passy Muir® Valve placement, the cuff must be completely deflated to allow airflow through the upper airway upon exhalation.
How does the Passy Muir valve work?
When placed on the hub of a tracheostomy tube or in-line with the ventilator circuit, the Passy Muir Valve redirects airflow through the vocal folds, mouth, and nose, enabling voice and improved communication.What must always be done before applying a Passy Muir valve?
Section A: General guidelines Tracheostomy tube cuffs must be completely deflated prior to placement of Passy Muir Valve (PMV)! Use of a PMV with a foam-filled trach cuff is contraindicated! Use Standard Precautions with all tracheostomy tube patients.
How does a speech valve work?
The speaking valve is a buttonlike piece of equipment that is placed on the outer hub of the tracheostomy tube. The one-way valve opens to let air in through the tracheostomy when the patient inspires. The valve closes during expiration, causing the air to follow the normal route of expiration and permitting speech.
When using a Passy Muir valve on a cuffed tracheostomy tube Why must the cuff be deflated?
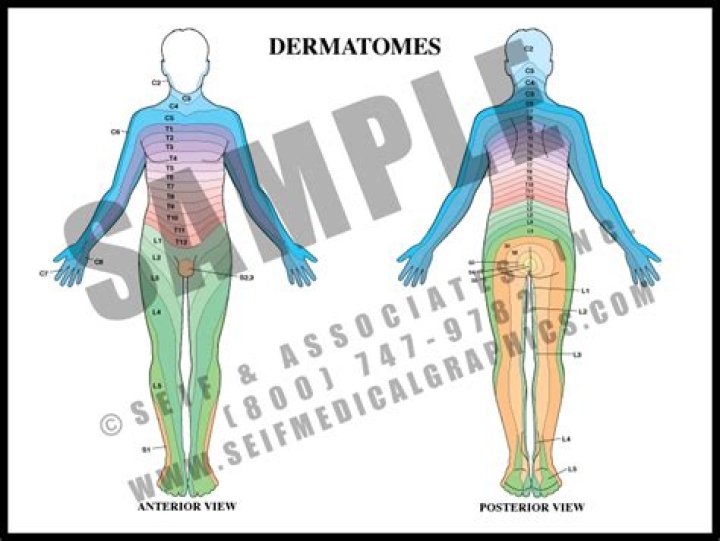
The definition of aspiration is when any food, liquid, or other matter passes below the vocal folds. Therefore, the cuff cannot prevent aspiration as it is located below the vocal folds (see Figure 1). When neither mechanical ventilation or a risk of gross aspiration is present, the cuff should be deflated.
How do you communicate with a tracheostomy patient?
- Mouthing words.
- Electrolarynges.
- Leak speech.
- Tracheal/digital occlusion.
- Talking tracheostomy tubes.
- Speaking Valves.
Does Passy Muir valve humidify?
HMEs retain heat and moisture of the patient’s expired air to warm and humidified the next inspired breath. NOTE: An HME will be ineffective when a speaking valve is in place.
When should a Passy Muir valve be removed?The PMV should last at least two months if you care for it properly. If the PMV becomes sticky, noisy or vibrates during use, it is time to replace it. Need suctioning – Remove the PMV and suction/ cough as needed. The cuff is not deflated completely – Immediately remove the PMV and deflate the cuff completely.
Article first time published onCan you eat with tracheostomy?
Having a tracheostomy usually will not affect the patient’s eating or swallowing patterns. Sometimes there are changes in swallowing dynamics that require adjusting to, but it is rare that this cannot be overcome in a short time.
Can you speak after a tracheostomy is removed?
It’s usually difficult to speak if you have a tracheostomy. Speech is generated when air passes over the vocal cords at the back of the throat. But after a tracheostomy most of the air you breathe out will pass through your tracheostomy tube rather than over your vocal cords.
What is the purpose for inflating the balloon of a tracheostomy?
Inflating the cuff during mechanical ventilation makes sure that air is entering the lungs and not escaping through the nose and mouth. The cuff also prevents aspiration of saliva in patients who have trouble swallowing.
Which conditions make it difficult for a patient to tolerate a Passy Muir valve?
- Thick secretions may require more aggressive pulmonary hygiene.
- Changes in your airway that make it difficult to breathe easily may stimulate a dry cough.
How does an electronic voice box work?
This small, battery-operated device is placed directly on the neck, under the chin, when you want to speak. When you push a button on the device, the electrolarynx produces a vibration that is transferred through the skin to the throat. You shape this sound into words with the mouth, tongue, lips, and teeth.
When would you never use a speaking valve?
This means adequate room for gas to flow past the tube in the trachea and out via the upper airways. An uncuffed or cuff-deflated tracheostomy tube is therefore required. Speaking valves should NEVER be used with the cuff inflated as this can lead to asphyxiation, respiratory arrest and death.
Can you use a speaking valve on a ventilator?
A speaking valve such as the Passy-Muir Valve may be used in-line with mechanical ventilation to allow for verbalization, among other benefits. Ventilator changes may be beneficial to the success of using a speaking valve during mechanical ventilation.
What happen if tracheostomy cuff over inflated?
Overinflation of the cuff may damage the cuff or increase pressure against the tracheal wall causing ischemia, softening of tracheal cartilage, or mucosal erosion. The tracheostomy cuff should be deflated as ordered by physician.
Do you deflate trach cuff when eating?
If your tracheostomy tube has a cuff, the speech therapist or provider will ensure the cuff is deflated during meal times. This will make it easier to swallow. If you have a speaking valve, you may use it while you eat. It will make it easier to swallow.
How long before you can talk after a tracheostomy?
But it may take at least 2 weeks to adjust to living with your trach (say “trayk”). At first, it may be hard to make sounds or to speak. Your doctor, nurses, respiratory therapists, and speech therapists can help you learn to talk with your trach tube or with other speaking devices.
Can you breathe on your own with a tracheostomy?
a tracheostomy. Usually air enters through the mouth and nose, goes through the windpipe and into the lungs. In cases with an injury or a blockage to the windpipe, a tracheostomy tube can bypass the damaged part of the windpipe and allow a person to continue to breathe on their own.
WHEN A tracheostomy is performed what is done to the windpipe?
Breathing is done through the tracheostomy tube rather than through the nose and mouth. The term “tracheotomy” refers to the incision into the trachea (windpipe) that forms a temporary or permanent opening, which is called a “tracheostomy,” however; the terms are sometimes used interchangeably.
Is Passy Muir a one-way valve?
The Passy Muir Valve (PMV) is a bias-closed, one-way valve, which allows the trach patient to inspire via the trach tube and exhale through the upper airway and vocal cords.
Can a laryngectomy patient use a Passy Muir valve to speak?
Laryngectomy patients cannot use a Passy-Muir® Valve! Due to the anatomical changes associated with total laryngectomy, the Passy-Muir® Valve can not be used on this population.
Why is a cuffed tracheostomy tube used?
Cuffed tubes allow positive pressure ventilation and prevent aspiration. If the cuff is not necessary for those reasons, it should not be used because it irritates the trachea and provokes and trap secretions, even when deflated.
Do you remove the inner cannula PMV?
disposable inner cannula with grasp ring, the inner cannula may need to be removed prior to PMV placement if the grasp ring extends beyond the 15mm hub of the tracheostomy tube. Failure to remove the inner cannula prior to use may obstruct opening movement of the PMV 005 (white) diaphragm.
What is the quality of life after a tracheostomy?
The median survival after tracheostomy was 21 months (range, 0-155 months). The survival rate was 65% by 1 year and 45% by 2 years after tracheostomy. Survival was significantly shorter in patients older than 60 years at tracheostomy, with a hazard ratio of dying of 2.1 (95% confidence interval, 1.1-3.9).
Can you vomit with a tracheostomy?
If you need to vomit, turn your head away from the tracheostomy stoma so that the vomit will not go down the opening. Using the bulb syringe or suction catheter is recommended.
Can you smell with a tracheostomy?
After surgery, your ability to smell will change because air no longer passes through your nose. For a few weeks after surgery, your nose may be sore and runny as its tissues adjust to the lack of air flow. This is normal and will improve over time. A method called “polite yawning” may help improve smell.
How long can you stay on a tracheostomy?
A tracheostomy can be used for days or, with proper care, for years. Most tracheostomies are temporary in intent. Research indicates that patients can be discharged from the intensive care unit with a tracheotomy cannula without adding morbidity or mortality.
Is a tracheostomy painful?
A planned tracheostomy is usually carried out under general anaesthetic, which means you’ll be unconscious during the procedure and will not feel any pain. A doctor or surgeon will make a hole in your throat using a needle or scalpel before inserting a tube into the opening.