How does diabetes lead to PVD
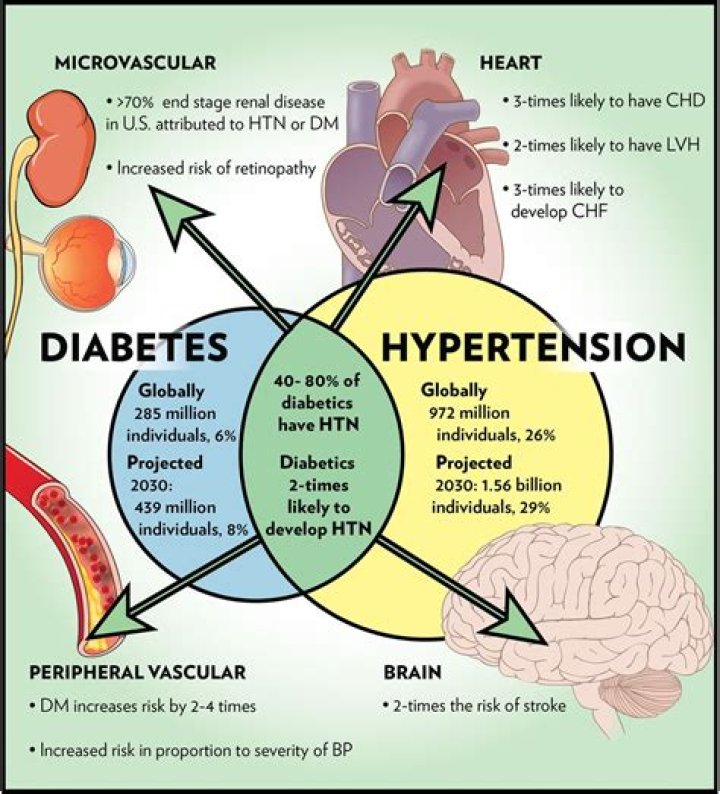
The risk of peripheral vascular disease (PVD) is increased in diabetic patients, occurs earlier and is often more severe and diffuse. Endothelial dysfunction, vascular smooth muscle cell dysfunction, inflammation and hypercoagubility are the key factors in diabetic arteriopathy
How does diabetes cause peripheral vascular?
Diabetes affects the lining around cells in your blood vessels. This means your blood vessels aren’t as flexible as they need to be to help blood flow smoothly. That makes your risk of PAD go up.
Why is diabetes a risk factor for peripheral artery disease?
People with diabetes are at an increased risk for developing PAD, which occurs when the peripheral arteries—those that do not supply blood to the heart and brain—become narrowed by an accumulation of fats, cholesterol, and other substances, a condition known as atherosclerosis.
Can diabetes cause peripheral arterial disease?
Diabetes is a lifelong (chronic) condition. It puts you at high risk for peripheral arterial disease (PAD). This is a disease of arteries in the legs. If you have PAD, arteries in other parts of your body are likely diseased, too.Why do diabetics have vascular problems?
Diabetes causes vascular disease if there is too much glucose in the blood. This excess glucose damages the blood vessels. Doctors do not know why Type 1 diabetes occurs, though they believe there is a hereditary link.
How do you code diabetes with PVD?
“Peripheral arteriosclerosis, peripheral vascular disease and peripheral arterial disease in a diabetic patient should be linked and coded as ‘diabetic peripheral angiopathy. ‘” If diabetes (E11. 9) and peripheral artery disease (PAD) (I73.
Does type 2 diabetes cause peripheral vascular disease?
Peripheral arterial disease (PAD) happens when buildup on the walls of blood vessels causes them to narrow. It commonly affects people with type 2 diabetes, who are also prone to high cholesterol and heart disease.
Why is a patient with diabetes and peripheral vascular disease at risk of infections of toes and other extremities?
If you have diabetes, you are at higher risk of also having peripheral arterial disease (PAD), a form of cardiovascular disease where blood flow to the legs and feet is limited because the arteries have become clogged with cholesterol and other substances.How do you differentiate PVD is a diabetic patient from a non diabetic patient?
The most common symptom of PVD is muscle pain in the lower limbs on exercise. In diabetes, pain perception may be blunted by the presence of peripheral neuropathy. Therefore, a patient with diabetes and PVD is more likely to present with an ischaemic ulcer or gangrene than a patient without diabetes.
What is the relationship between diabetes and poor blood circulation?The link between diabetes and poor circulation Diabetes puts you at high risk for conditions that affect your circulatory system, including: High blood glucose levels cause fatty deposits to form inside blood vessels. Over time, these deposits make your blood vessels narrow and hard, lessening blood flow.
Article first time published onHow does type 2 diabetes affect the arteries?
Over time, high blood sugar can damage blood vessels and the nerves that control your heart. People with diabetes are also more likely to have other conditions that raise the risk for heart disease: High blood pressure increases the force of blood through your arteries and can damage artery walls.
Does diabetes cause narrowing arteries?
People with diabetes have too much sugar in their blood. This may change blood chemistry and cause blood vessels to narrow. Or, it can damage blood vessels — a process known as atherosclerosis. Atherosclerosis is also called hardening of the arteries.
Can diabetes cause posterior vitreous detachment?
The vitreous in diabetic patients undergoes abnormal collagen crosslinking and nonenzymatic glycation, which lead to precocious liquefaction and posterior vitreous detachment (PVD). Diabetic patients have been shown to exhibit vitreous degeneration[153–155] in a manner similar to that normally seen in older adults.
Is Diabetic peripheral angiopathy the same as PVD?
“Peripheral vascular disease” is synonymous with peripheral angiopathy. In accordance with the “Diabetes > with” coding convention noted above, even when the medical record does not link PVD to diabetes as the cause, the linkage is presumed unless the physician specifically indicates they are not related.
Is peripheral angiopathy same as PVD?
In addition to peripheral artery disease and PAD, you may have heard the condition referred to as peripheral vascular disease or PVD. This often leads the two to be used interchangeably, and while the term PVD does encompass all cases of PAD, the term PAD cannot be used to refer to all types of PVD.
What is Diabetic peripheral angiopathy with gangrene?
Diabetic peripheral angiopathy (DPA) is a blood vessel disease caused by high blood sugar levels (glucose). It is one of the most common complications of diabetes. It affects blood vessels that carry oxygen-rich blood away from the heart.
What are the microvascular complications of diabetes?
Microvascular complications of diabetes are those long-term complications that affect small blood vessels. These typically include retinopathy, nephropathy, and neuropathy. Retinopathy is divided into two main categories: Nonproliferative retinopathy and proliferative retinopathy.
What causes PVD?
What causes peripheral vascular disease? The most common cause of PVD is atherosclerosis, the buildup of plaque inside the artery wall. Plaque reduces the amount of blood flow to the limbs. It also decreases the oxygen and nutrients available to the tissue.
How is PVD diagnosed?
- Angiography. Angiography involves injecting dye into the arteries to identify a clogged or blocked artery.
- Ankle-brachial index (ABI). …
- Blood tests. …
- Computerized tomography angiography (CTA). …
- Magnetic resonance angiography (MRA). …
- Ultrasound.
Does diabetes cause high blood pressure?
Diabetes damages arteries and makes them targets for hardening, called atherosclerosis. That can cause high blood pressure, which if not treated, can lead to trouble including blood vessel damage, heart attack, and kidney failure.
How do diabetics increase circulation in their feet?
- Put your feet up when you are sitting.
- Wiggle your toes for a few minutes throughout the day. Move your ankles up and down and in and out to help blood flow in your feet and legs.
- Do not wear tight socks or elastic stockings. …
- Be more physically active. …
- Stop smoking.
How does insulin help diabetes?
Sometimes, people with type 2 diabetes or gestational diabetes need insulin therapy if other treatments haven’t been able to keep blood glucose levels within the desired range. Insulin therapy helps prevent diabetes complications by keeping your blood sugar within your target range.
How is type 2 diabetes related to CHF?
Over time, high blood sugar levels from diabetes can damage the blood vessels in your heart, making them more likely to develop fatty deposits. The longer you have diabetes, the higher the chances are that you will develop heart disease. Around 30 per cent of people with Type 2 diabetes also have CVD1.
How does blood pressure and sugar control cholesterol?
- Eat healthy fats. To reduce cholesterol levels, many people cut out sources of fat from their diets. …
- Reduce your intake of added. sugars. …
- Consume more vegetables. Increasing your intake of both. …
- Eat mostly whole, nutritious. foods.
What are Jemima's risk factors for type 2 diabetes?
- Weight. Being overweight or obese is a main risk.
- Fat distribution. Storing fat mainly in your abdomen — rather than your hips and thighs — indicates a greater risk. …
- Inactivity. …
- Family history. …
- Race and ethnicity. …
- Blood lipid levels. …
- Age. …
- Prediabetes.
What are two reasons why diabetes increases the incidence atherosclerosis?
Although multiple metabolic abnormalities that characterize diabetes are involved in the progression of atherosclerosis in patients with DM, it may be said that prolonged exposure to hyperglycemia and insulin resistance clustering with other risk factors such as obesity, arterial hypertension, and dyslipidemia play …
Why does diabetes cause retinopathy?
Diabetic retinopathy is caused by prolonged high blood glucose levels Over time, high sugar glucose levels can weaken and damage the small blood vessels within the retina. This may cause haemorrhages, exudates and even swelling of the retina. This then starves the retina of oxygen, and abnormal vessels may grow.
What type of diabetes is atherosclerosis a risk factor for?
Type 2 diabetes mellitus is associated with a marked increase in the risk of atherosclerotic diseases, including coronary heart disease, peripheral arterial disease, and cerebrovascular disease. Insulin resistance is a key factor in the pathogenesis of type 2 diabetes mellitus.
Does diabetes increase risk of retinal detachment?
Retinal detachment. The abnormal blood vessels associated with diabetic retinopathy stimulate the growth of scar tissue, which can pull the retina away from the back of the eye. This can cause spots floating in your vision, flashes of light or severe vision loss.
Can diabetes cause vitreous floaters?
Diabetic retinopathy is blood vessel damage in the retina that happens as a result of diabetes. Diabetic retinopathy can cause a range of symptoms, including blurred vision, difficulty seeing colors, and eye floaters.
Can diabetes cause holes in retina?
Diabetic retinopathy is damage to the eye’s retina that occurs from complications of long term diabetes resulting in damage to the blood vessels of the retina, the light-sensitive tissue at the back of the eye. People with both type 1 diabetes and type 2 diabetes are at risk for this condition.