How does DIC affect platelets
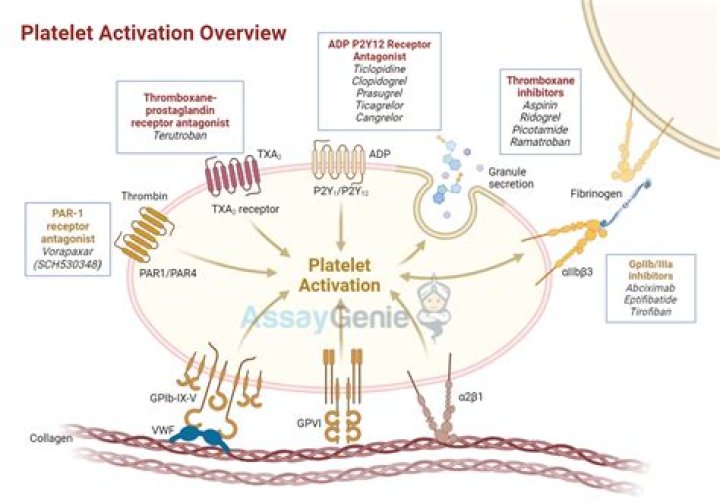
Patients with DIC have a low or rapidly decreasing platelet count, prolonged global coagulation tests, low plasma levels of coagulation factors and inhibitors, and increased markers of fibrin formation and/or degradation, such as D-dimer or fibrin degradation products.
Is there thrombocytosis in DIC?
Patients with DIC can present with a wide range of abnormalities in their laboratory values. Typically, prolonged coagulation times, thrombocytopenia, high levels of fibrin degradation products (FDPs), elevated D-dimer levels, and microangiopathic pathology (schistocytes) on peripheral smears are suggestive findings.
How does DIC cause prolonged PT?
Both PT and aPTT seem prolonged in about 50% of DIC cases which is attributed to the consumption of coagulation factors but can also be prolonged in impaired synthesis of coagulation factors and in massive bleeding.
Can DIC cause splenomegaly?
This case also demonstrated chronic DIC in ad– dition to significant splenomegaly. The vascular symp- toms, inducing bleeding tendency and thrombotic status, were improved by splenectomy.What suppresses fibrinolytic activity in the pathogenesis of disseminated intravascular coagulation DIC )?
However, this profibrinolytic response is almost immediately followed by suppression of fibrinolytic activity due to a sustained increase in plasma levels of PAI-1 ; these effects are mediated by TNF-2 and IL-1.
Do you agree that disseminated intravascular coagulation DIC leads to Hypocoagulation?
DIC is characterized by the systemic activation of coagulation, leading to widespread microvascular thrombosis, which compromises organ perfusion and can contribute to organ failure. The ongoing activation of coagulation may exhaust platelet and coagulation factors, resulting in a hypocoagulable state and bleeding.
Which factors can lead to the development of thrombocytopenia?
Viral: HIV, hepatitis C, Ebstein-Barr virus, parvovirus, mumps, varicella, rubella, Zika viral infections can cause thrombocytopenia. Sepsis causes bone marrow suppression. Helicobacter pylori. Leptospirosis, brucellosis, anaplasmosis, and other tick-borne infections are associated with thrombocytopenia.
What causes splenomegaly?
Infections, such as mononucleosis, are among the most common causes of splenomegaly. Problems with your liver, such as cirrhosisand cystic fibrosis, can also cause an enlarged spleen. Another possible cause of splenomegaly is juvenile rheumatoid arthritis. This condition can cause inflammation of the lymph system.How does leukemia cause splenomegaly?
Splenomegaly can also occur as a result of certain blood cancers, such as leukemias and lymphomas. In these diseases, cancer cells can infiltrate the spleen and lead to enlargement. Additionally, splenomegaly can result from portal hypertension which refers to increased blood pressure in the portal vein.
How does Hypersplenism cause anemia?When your spleen’s overactive, or “hyper,” it removes too many blood cells, including healthy ones. Without enough healthy, mature blood cells, your body has a harder time fighting infections and you may become anemic.
Article first time published onDoes DIC affect INR?
HIT complicated by DIC may cause the following pattern: Platelets may be profoundly reduced (e.g., platelets <20,000/uL) INR prolongation and hypofibrinogenemia may occur.
How does DIC cause ischemia?
DIC leads to fibrin and platelet deposition in small vessels, which can cause tissue ischemia and result in organ dysfunction (Figure 56-1). The consumptive coagulopathy can also lead to clinically significant bleeding.
What is a classic symptom of disseminated intravascular coagulation DIC )?
DIC may develop quickly over hours or days, or more slowly. Signs and symptoms may include bleeding, bruising, low blood pressure, shortness of breath, or confusion. Complications can be life-threatening and include bleeding or multiple organ failure.
What is the most common cause of DIC in pregnancy?
Acute obstetrical hemorrhage is one of the leading causes for DIC in pregnancy and is one of the most avoidable etiologies of maternal death.
How does heparin treat DIC?
Heparin, as an anticoagulant, which, not only inhibits the activation of the coagulation system, but is also an anti-inflammatory and immunomodulatory agent, has been widely used during DIC treatment and in the prevention and treatment of thrombotic diseases.
What are the complications of DIC?
- Acute kidney injury.
- Change in mental status.
- Respiratory dysfunction.
- Hepatic dysfunction.
- Life-threatening thrombosis and hemorrhage (in patients with moderately severe–to–severe DIC)
- Cardiac tamponade.
- Hemothorax.
- Intracerebral hematoma.
Which respiratory manifestations would be associated with DIC?
In DIC, blood clots form throughout the body’s small blood vessels. These blood clots can reduce or block blood flow through the blood vessels. This can cause the following signs and symptoms: Chest pain and shortness of breath if blood clots form in the blood vessels in your lungs and heart.
Which conditions are commonly associated with DIC quizlet?
- Sepsis and severe infection (including COVID-19 )
- Trauma (neurotrauma)
- Organ destruction (eg, pancreatitis)
- Malignancy (solid and lymphoproliferative/myeloproliferative malignancies)
- Severe transfusion reactions.
What are the different types of thrombocytopenia?
- idiopathic (or immune) thrombocytopenic purpura (ITP)
- thrombotic thrombocytopenic purpura (TTP)
- haemolytic uraemic syndrome (HUS).
Why does DIC increase PT and PTT?
Schistocytes are seen in approximately 50% of cases of DIC. Patients with DIC will present with both the PT and PTT prolonged due to decreased levels of coagulation factors in both the intrinsic and extrinsic pathways in a Protime and Partial Thromboplastin Time study.
What do labs look like in DIC?
Laboratory findings suggestive of DIC include a low platelet count, elevated D-dimer concentration, decreased fibrinogen concentration, and prolongation of clotting times such as prothrombin time (PT).
Which is the most important goal for the patient with disseminated intravascular coagulation DIC?
The goals of pharmacotherapy in cases of disseminated intravascular coagulation (DIC) are to reduce morbidity and to prevent complications. Therapy should be based on etiology and aimed at eliminating the underlying disease.
Why does splenomegaly cause leukopenia?
Anemia – The anemia observed in splenomegaly results from sequestration and hemodilution. Leukopenia – Increased destruction or sequestration of leukocytes causes the leukopenia observed in splenomegaly.
What organisms cause splenomegaly?
Viral infections, such as mononucleosis. Bacterial infections, such as syphilis or an infection of your heart’s inner lining (endocarditis) Parasitic infections, such as malaria. Cirrhosis and other diseases affecting the liver.
Does anemia cause splenomegaly?
Splenomegaly may occur with severe, persistent, untreated iron deficiency anemia. This is uncommon in the United States and Europe.
What causes enlarged liver and spleen?
Enlarged liver and spleen has a variety of causes including infections, blood disorders, liver disease, and cancers.
Can thyroid affect spleen?
Histological and immunohistochemical results showed that the spleen and diaphragm metastases derived from thyroid follicular carcinoma. Radioiodine uptake by the pulmonary metastases confirmed the thyroid source.
What is palpable spleen?
Clinically, if a spleen is palpable (felt via external examination), it means it is enlarged as it has to undergo at least twofold enlargement to become palpable. However, the tip of the spleen may be palpable in a newborn baby up to three months of age.
Can Hypersplenism cause thrombocytopenia?
Thrombocytopenia associated with hypersplenism is usually mild (50,000 to 100,000 platelets per microliter) and requires no specific treatment. Severe thrombocytopenia or thrombocytopenia that interferes with a required therapy may require intervention, although this is rare.
Does thrombocytosis cause splenomegaly?
Spleen enlargement, present in 10-20% of Essential Thrombocythemia (ET) patients at diagnosis, is a feature clinically easy to assess, confirmable by echography with a very low chance of misinterpretation. Nonetheless, the clinical and prognostic role of splenomegaly has been seldom evaluated.
Does cirrhosis cause thrombocytopenia?
Thrombocytopenia is a common complication in liver disease and can adversely affect the treatment of liver cirrhosis, limiting the ability to administer therapy and delaying planned surgical/diagnostic procedures because of an increased risk of bleeding.