How Does Medicare pay for SNF
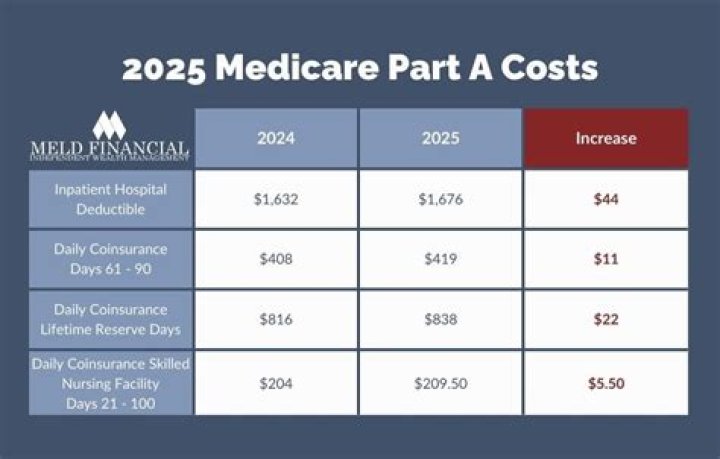
In a nutshell, Medicare will pay for short-term skilled nursing facility stays for specific situations. If you need ongoing or long-term care in a skilled nursing facility, you will have to pay out of pocket or use other programs to fund these services.
Does Medicare pay for skilled nursing facilities?
In a nutshell, Medicare will pay for short-term skilled nursing facility stays for specific situations. If you need ongoing or long-term care in a skilled nursing facility, you will have to pay out of pocket or use other programs to fund these services.
How does Medicare reimburse nursing homes?
Part A services are reimbursed under a prospective payment system that pays facilities a daily rate that covers all patient-related expenses, including nursing services, therapy services—calculated in minutes—and a daily room charge.
How Much Does Medicare pay for SNF?
What do I pay for skilled nursing facility (SNF) care in 2019? In Original Medicare, for each benefit period, you pay: ■ For days 1–20: You pay nothing for covered services. Medicare pays the full cost. For days 21–100: You pay up to $170.50 per day for covered services.How Long Does Medicare pay for nursing home care?
Medicare covers up to 100 days of care in a skilled nursing facility (SNF) each benefit period. If you need more than 100 days of SNF care in a benefit period, you will need to pay out of pocket. If your care is ending because you are running out of days, the facility is not required to provide written notice.
What does Medicare Part B cover in skilled nursing facilities?
These services include, but are not limited to, diagnostic laboratory tests, x rays, hospital outpatient services, ambulance services, rehabilitation services, the purchase and rental of durable medical equipment, orthotic/prosthetic devices, and surgical dressings.
What is not paid by Medicare Part B while the patient is in a SNF?
Screening and preventive services are not included in the SNF PPS amount but may be paid separately under Part B for Part A patients who also have Part B coverage. Screening and preventive services are covered only under Part B.
What is the Medicare 3 day rule?
The 3-day rule requires the patient have a medically necessary 3-day-consecutive inpatient hospital stay. … SNF extended care services are an extension of care a patient needs after a hospital discharge or within 30 days of their hospital stay (unless admitting them within 30 days is medically inappropriate).Does Medicare Part B pay for SNF?
Medicare provides coverage for care required at a skilled nursing facility (SNF). … For Medicare Part B, this comes to 20%. Copayment: This is a fixed dollar amount that an insured person pays when receiving certain treatments.
What does Medicare a cover 2021?Medicare Part A covers inpatient hospital, skilled nursing facility, and some home health care services. About 99 percent of Medicare beneficiaries do not have a Part A premium since they have at least 40 quarters of Medicare-covered employment.
Article first time published onHow are SNF claims billed?
The SNF Prospective Payment System (PPS) pays for all SNF Part A inpatient services. Part A payment is primarily based on the Resource Utilization Group (RUG) assigned to the beneficiary following required Minimum Data Set (MDS) 3.0 assessments.
What reimbursement methodology is used in a Skilled Nursing Facility SNF )?
The Medicare Patient-Driven Payment Model (PDPM) is a major overhaul to the current skilled nursing facility (SNF) prospective payment system (PPS). It is designed to address concerns that a payment system based on the volume of services provided creates inappropriate financial incentives.
What payment methodology reimburse skilled nursing facilities?
A Prospective Payment System (PPS) is a method of reimbursement in which Medicare payment is made based on a predetermined, fixed amount. The payment amount for a particular service is derived based on the classification system of that service (for example, diagnosis-related groups for inpatient hospital services).
What is the difference between a skilled nursing facility and a nursing home?
Nursing homes are where people usually go when they require high levels of assistance with non-medical, everyday living tasks. On the other hand, skilled nursing is what people may receive when they require medical care in cases such as recovering from a stroke.
What happens when you run out of Medicare days?
Medicare will stop paying for your inpatient-related hospital costs (such as room and board) if you run out of days during your benefit period. To be eligible for a new benefit period, and additional days of inpatient coverage, you must remain out of the hospital or SNF for 60 days in a row.
What is considered a skilled nursing facility?
A skilled nursing facility is an in-patient treatment and rehabilitation center featuring licensed nurses and other medical professionals. These services can be very expensive but most skilled nursing facilities are covered, at least in part, by private health insurance or else Medicare or Medicaid.
How does SNF billing work?
An SNF is responsible for the charges incurred by the technical aspect of a service, while the provider bills Medicare directly for the professional aspect. The provider then bills the SNF for the technical expense out of its per diem rate received from Medicare Part A.
What is SNF consolidated billing?
The consolidated billing requirement confers on the SNF the billing responsibility for the entire package of care that residents receive during a covered Part A SNF stay and physical, occupational, and speech therapy services received during a non-covered stay.
Is SNF Part A or Part B?
For SNF patients covered under Medicare Part A, the majority of services, including DME, are required to be provided by the SNF and payment is included in the SNF PPS rate. … Thus, Part B reimbursement for DME is not possible.
Which part of Medicare pays for rehab?
Medicare Part A covers medically necessary inpatient rehab (rehabilitation) care, which can help when you’re recovering from serious injuries, surgery or an illness.
What qualifies a patient for skilled nursing care?
1.) A skilled nursing facility level of care is appropriate for the provision of skilled rehabilitative therapies when ALL of the following criteria are met: a) the patient requires skilled rehabilitative therapy(ies) at a frequency and intensity of at least 5 days per week for at least 60 minutes per day.
What documentation is included in a skilled nursing care record?
Documentation should include: the resident’s vital signs. the reason why the resident is receiving skilled services. a detailed description of the resident’s condition at that time.
How many days of rehab does Medicare cover?
Medicare will pay for inpatient rehab for up to 100 days in each benefit period, as long as you have been in a hospital for at least three days prior. A benefit period starts when you go into the hospital and ends when you have not received any hospital care or skilled nursing care for 60 days.
What is a skilled nursing assessment?
An assessment includes collecting information about: Your current physical and mental condition. Your medical history. Medications you’re taking. How well you can do activities of daily living (like bathing, dressing, eating, getting in and out of bed or a chair, moving around, and using the bathroom)
How Long Does Medicare pay for rehab after stroke?
How long does Medicare pay for rehab after a stroke? Medicare covers up to 90 days of inpatient rehab. You’ll need to meet your Part A deductible and cover coinsurance costs. After your 90 days, you’ll start using your lifetime reserve days.
How long can you stay in ICU on Medicare?
Medicare covers a hospital stay of up to 90 days, though a person may still need to pay coinsurance during this time. While Medicare does help fund longer stays, it may take the extra time from an individual’s reserve days. Medicare provides 60 lifetime reserve days.
Does Medicare have a lifetime limit?
In general, there’s no upper dollar limit on Medicare benefits. As long as you’re using medical services that Medicare covers—and provided that they’re medically necessary—you can continue to use as many as you need, regardless of how much they cost, in any given year or over the rest of your lifetime.
What is the Medicare 2 day rule?
In general, the original Two-Midnight rule stated that: Inpatient admissions would generally be payable under Part A if the admitting practitioner expected the patient to require a hospital stay that crossed two midnights and the medical record supported that reasonable expectation.
What is the Irmaa for 2021?
IRMAA Table2021More than $111,000 but less than or equal to $138,000$297.00More than $138,000 but less than or equal to $165,000$386.10More than $165,000 but less than $500,000$475.20More than $500,000$504.90
Are Medicare Part B premiums going up in 2021?
In November 2021, CMS announced the monthly Medicare Part B premium would rise from $148.50 in 2021 to $170.10 in 2022, a 14.5% ($21.60) increase.
How much does Medicare take from Social Security?
In 2021, based on the average social security benefit of $1,514, a beneficiary paid around 9.8 percent of their income for the Part B premium. Next year, that figure will increase to 10.6 percent.