How does rtPA work for stroke
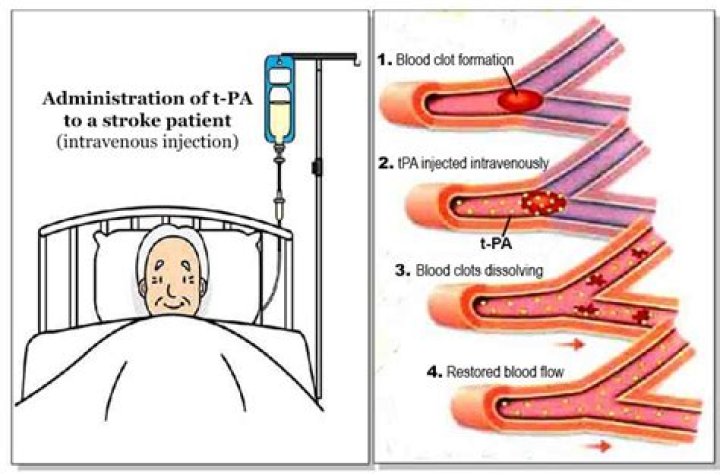
TPA works by dissolving blood clots. That helps to restore blood flow to the brain after a stroke, potentially preventing additional brain cells from dying.
What is rtPA test?
In the early 1990s, 3 large randomized trials were started to test the hypothesis that thrombolysis with intravenous recombinant tissue plasminogen activator (rtPA) in acute ischemic stroke could restore blood flow and improve patient outcome.
Is rtPA the same as tPA?
tPA can be manufactured using recombinant biotechnology techniques; tPA produced by such means are referred to as recombinant tissue plasminogen activator (rtPA). Specific rtPAs include alteplase, reteplase, and tenecteplase. They are used in clinical medicine to treat embolic or thrombotic stroke.
When do you give rtPA?
Alteplase (IV r-tPA) within 4.5 hours of stroke onset remains the standard of care for most ischemic stroke patients.What is rtPA medication?
The use of recombinant tissue plasminogen activator (rtPA) has been the standard of care for treatment of acute ischemic stroke for several years.
How do you give RTPA?
- Administer within 30 minutes of hospital arrival.
- Adults greater than or equal to 67 kg get 100 mg total dosage administered as a 15 mg IV bolus, followed by 50 mg IV infused over 30 minutes, and then 35 mg IV infused over the next 60 minutes.
How long do clot busters take to work?
However, tPA has to be given within a certain time frame to work. Long-time guidelines stated that the drug should be infused within three hours of the first stroke symptoms — or, for certain patients, within 4.5 hours.
How long does it take tPA to dissolve a clot?
It may take up to 72 hours for the clot to dissolve (although most clots dissolve within 24 hours).Why is streptokinase only given once?
As streptokinase is a bacterial product, the body has the ability to build up an immunity to it. Therefore, it is recommended that this medication should not be used again after four days from the first administration, as it may not be as effective and can also cause an allergic reaction.
What is the best medication for stroke?An IV injection of recombinant tissue plasminogen activator (tPA) — also called alteplase (Activase) — is the gold standard treatment for ischemic stroke. An injection of tPA is usually given through a vein in the arm with the first three hours. Sometimes, tPA can be given up to 4.5 hours after stroke symptoms started.
Article first time published onWhat happens in the first 3 days after a stroke?
During the first few days after your stroke, you might be very tired and need to recover from the initial event. Meanwhile, your team will identify the type of stroke, where it occurred, the type and amount of damage, and the effects. They may perform more tests and blood work.
What is the difference between an ischemic stroke and a hemorrhagic stroke?
An ischemic stroke is when blood vessels to the brain become clogged. A hemorrhagic stroke is when bleeding interferes with the brain’s ability to function.
Who Cannot receive tPA?
Other Contraindications for tPA Significant head trauma or prior stroke in the previous 3 months. Symptoms suggest subarachnoid hemorrhage. Arterial puncture at a noncompressible site in previous 7 days. History of previous intracranial hemorrhage.
Why is tPA not given after 4.5 hours?
tPA administered at 4.5 hours after carotid thrombosis resulted in a decrease in thrombus area and survival rate, whereas no benefit on cerebral blood flow.
What are the major side effects of tPA?
- Pulmonary embolism.
- Cholesterol embolism.
- Abnormal heartbeats.
- Allergic reactions.
- Re-embolization of deep DVT venous thrombi during treatment of acute massive pulmonary embolism.
- Angioedema.
How long does it take alteplase to work?
Alteplase in acute myocardial infarction (AMI) patients is rapidly cleared from the plasma with an initial half-life of less than 5 minutes. There is no difference in the dominant initial plasma half-life between the 3-hour and accelerated regimens for AMI.
Can heparin break up clots?
This medicine is sometimes called a blood thinner, although it does not actually thin the blood. Heparin will not dissolve blood clots that have already formed, but it may prevent the clots from becoming larger and causing more serious problems.
What is the most common complication of fibrinolytic therapy?
The most feared complication of fibrinolysis is intracranial hemorrhage (ICH), but serious hemorrhagic complications can occur from bleeding at any site in the body. Risk factors for hemorrhagic complications include the following: Increasing age. Lower body weight.
Are clot busters safe?
Clot-busting drugs may be safe for certain stroke patients with brain aneurysms that haven’t ruptured, researchers say. An aneurysm is a bulge in the wall of a blood vessel. In the new study, patients had suffered an ischemic stroke, which is caused by blocked blood flow in the brain.
What are the odds of surviving a pulmonary embolism?
A pulmonary embolism (PE) is a blood clot in the lungs, which can be serious and potentially lead to death. When left untreated, the mortality rate is up to 30% but when treated early, the mortality rate is 8%.
Can a blood clot go away on its own?
Blood clots do go away on their own, as the body naturally breaks down and absorbs the clot over weeks to months. Depending on the location of the blood clot, it can be dangerous and you may need treatment.
Why does tPA cause intracranial hemorrhage?
The risk of hemorrhage is increased because tPA triggers plasmin activation, which degrades cross-linked fibrin into fibrin split products and reversal agents. Reperfusion injury and breakdown of the blood-brain barrier may also contribute to the risk of symptomatic intracranial hemorrhage.
Is Ischemic stroke?
Ischemic stroke is one of three types of stroke. It’s also referred to as brain ischemia and cerebral ischemia. This type of stroke is caused by a blockage in an artery that supplies blood to the brain. The blockage reduces the blood flow and oxygen to the brain, leading to damage or death of brain cells.
Why can tPA only be given within 3 hours?
Most of them are ineligible because they come to the hospital after the three-hour time window.” The timing of treatment is important, because giving a strong blood thinner like tPA during a stroke can cause bleeding inside the brain.
What is the most important complication of streptokinase therapy?
The hemorrhagic stroke as the most serious ADR of streptokinase was documented in three patients.
Why is streptokinase not used in strokes?
Studies of streptokinase in acute stroke were stopped due to an increase in mortality compared to placebo due to increased haemorrhage rates.
How much does streptokinase cost?
The Red Book average wholesale price of 1.5 million units of streptokinase was $320; the price of 100 mg of t-PA was $2,750.
What happens after tPA is given?
If bleeding into the brain happens after TPA is given, it may cause your stroke symptoms to be worse and may result in death. However, the death rate is the same with or without TPA and there is still a greater chance of recovery with TPA treatment. TPA may also cause bleeding in other areas of the body.
Is tPA a blood thinner?
It has also been used in treatment for pulmonary embolism and myocardial infarction. TPA is a blood thinner, and therefore it is not used for hemorrhagic strokes or head trauma.
Can the brain heal itself after a stroke?
Fortunately, damaged brain cells are not beyond repair. They can regenerate — this process of creating new cells is called neurogenesis. The most rapid recovery usually occurs during the first three to four months after a stroke. However, recovery can continue well into the first and second year.
What are the 5 warning signs of a stroke?
- Sudden numbness or weakness in the face, arm or leg (especially on one side of the body).
- Sudden confusion or trouble speaking or understanding speech.
- Sudden vision problems in one or both eyes.
- Sudden difficulty walking or dizziness, loss of balance or problems with coordination.