How fast does mucormycosis spread
If not treated in a timely manner, the fungus can spread quite quickly and can prove fatal. “The infection is so aggressive that it spreads faster than cancer. In 15 days, it can spread from your mouth to eyes and within a month to the brain,” Dr Sonal had told TNM.
Does mucormycosis spread quickly?
Mucormycosis is particularly dangerous because it spreads quickly throughout the body. Left untreated, the infection can spread to the lungs or the brain.
How long can you live with mucormycosis?
Mucormycosis has poor prognosis with a mortality rate of 17–51% [10]. Mortality is higher in case of diagnostic delay of more than five days and monocytopenia in patients with active malignant blood diseases. Surgical treatment associated with antifungals improves prognosis [2,10].
How long does it take for a fungal infection to spread?
It can take days or up to 2 weeks before you develop the infection after being in contact with the fungus. The fungi that cause ringworm can live for a long time on objects.How does mucormycosis disease spread?
People get mucormycosis through contact with fungal spores in the environment. For example, the lung or sinus forms of the infection can occur after someone inhales the spores from the air. A skin infection can occur after the fungus enters the skin through a scrape, burn, or other type of skin injury.
Is mucormycosis an emergency situation?
Background: Mucormycosis is a rare presentation for patients in the emergency department (ED), primarily af- fecting immunocompromised patients. Multiple forms of infection are present, and with poor prognosis, ED di- agnosis and treatment of this deadly condition are necessary.
Can mucormycosis be cured on its own?
Successful management of mucormycosis requires early diagnosis, reversal of underlying predisposing risk factors, surgical debridement and prompt administration of active antifungal agents. However, mucormycosis is not always amenable to cure.
What cures ringworm fast?
Over-the-counter antifungals can kill the fungus and promote healing. Effective medications include miconazole (Cruex), clotrimazole (Desenex) and terbinafine (Lamisil). After cleaning the rash, apply a thin layer of antifungal medication to the affected area 2 to 3 times per day or as directed by the package.Do ringworms go away without treatment?
There’s no set time limit for a ringworm infection. Without treatment, it may go away on its own in a matter of months in a healthy person. Or it may not. Ringworm on the body is usually treated with a topical ointment such as terbinafine.
How do you prevent ringworm from spreading?- avoid scratching or touching the ringworm lesion.
- wash the hands thoroughly after touching or treating the ringworm lesion.
- wash clothes, bedding, and towels in hot, soapy water.
Does mucormycosis require surgery?
Surgical debridement is the key to controlling and eliminating mucormycosis, but anti-fungal treatment is also typically used in combination. Studies confirm amphotericin-B liposomal 3.0 mg/kg accompanied by aggressive surgical debridement, up to and including amputation, is reasonably effective.
How do you get rid of mucormycosis?
How is mucormycosis treated? Mucormycosis is a serious infection and needs to be treated with prescription antifungal medicine, usually amphotericin B, posaconazole, or isavuconazole. These medicines are given through a vein (amphotericin B, posaconazole, isavuconazole) or by mouth (posaconazole, isavuconazole).
How common is mucormycosis?
Disease burden The incidence rate of mucormycosis globally varies from 0.005 to 1.7 per million population. In India, prevalence of mucormycosis is estimated as 140 per million population, which is about 80 times higher than the prevalence in developed countries.
Is mucormycosis related to Covid?
Mucormycosis, a fungal infection caused by ubiquitous environmental molds, such as Rhizopus arrhizus, Rhizomucor pusillus, Apophysomyces variabilis and Lichtheimia corymbifera, is surging as a COVID-19-associated infection at unprecedented rates throughout India and raising alarm bells around the world.
Can CT scan detect mucormycosis?
CT and MRI shows a spectrum of findings in rhinocerebral mucormycosis. Imaging plays a major role in assessing the extent of involvement and complications.
What is the symptom of mucormycosis?
Cutaneous (skin) mucormycosis can look like blisters or ulcers, and the infected area may turn black. Other symptoms include pain, warmth, excessive redness, or swelling around a wound. Symptoms of gastrointestinal mucormycosis include: Abdominal pain.
What causes mucormycosis?
Types of fungi that cause mucormycosis The most common types that cause mucormycosis are Rhizopus species and Mucor species. Other examples include Rhizomucor species, Syncephalastrum species, Cunninghamella bertholletiae, Apophysomyces, Lichtheimia (formerly Absidia), Saksenaea, and Rhizomucor.
How do you treat mucormycosis at home?
- Eat Yoghurt and Probiotics. Yoghurt and other probiotics have an ample amount of good bacteria that help stave off many fungal infections. …
- Wash with Soap and Water. …
- Use Apple Cider Vinegar. …
- Use Tea Tree Oil. …
- Use Coconut Oil. …
- Use Turmeric. …
- Use Aloe Vera. …
- Garlic.
What is mucormycosis and what area of the body is most commonly infected?
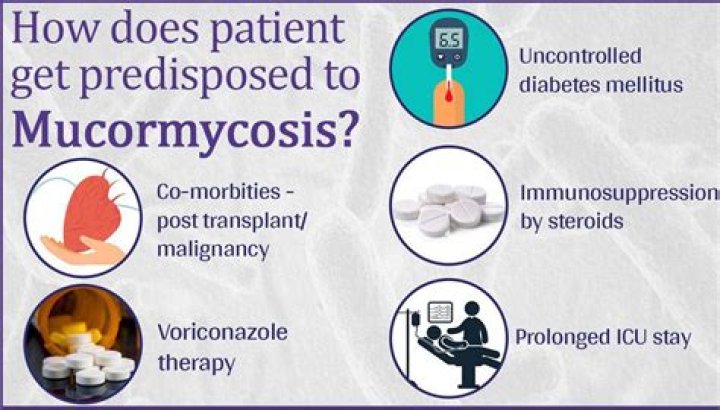
Mucormycosis mainly affects people who have health problems or take medicines that lower the body’s ability to fight germs and sickness. It most commonly affects the sinuses or the lungs after inhaling fungal spores from the air. It can also occur on the skin after a cut, burn, or other type of skin injury.
What can be mistaken for ringworm?
There are a variety of ringworm imposters that could be causing you or your child’s rash. The two most common conditions are nummular eczema and granuloma annulare. Nummular eczema causes circular patches of dry skin that can burn or become dry and scaly.
Are ringworms itchy?
Ringworm is a common skin infection that is caused by a fungus. It’s called “ringworm” because it can cause a circular rash (shaped like a ring) that is usually red and itchy.
Is ringworm always itchy?
Ringworm might appear as roundish, flat patches of itchy skin. Ringworm of the body (tinea corporis) is a rash caused by a fungal infection. It’s usually an itchy, circular rash with clearer skin in the middle.
What does ringworm initially look like?
Ringworm infection can affect both humans and animals. The infection initially appears as red patches on affected areas of the skin and later may spread to other parts of the body. It may affect the scalp, feet, nails, groin, beard, or other areas.
How quickly does ringworm show up?
How soon do symptoms appear? The incubation period is unknown for most of these agents, however ringworm of the scalp is usually seen 10 to 14 days after contact and ringworm of the body is seen 4 to 10 days after initial contact.
Does ringworm get worse in the heat?
Ringworm of the skin can start as a small patch of itchy, red, or scaling skin. The rash can spread and cover a large area. Clothing that rubs the skin can irritate the rash. Sweat, heat, or moisture in the air (humidity) can make the itching and infection worse.
Is ringworm a big deal?
The fungal infection ringworm can be a nuisance, but good treatment options are available. Despite its name, ringworm isn’t caused by a worm — but rather by a fungus. “The rash happens to come as a ring,” says Amy Kassouf, MD, a dermatologist with the Cleveland Clinic in Ohio.
How do I clean my house after ringworm?
To kill ringworm spores, clean and disinfect solid surfaces. Launder bedding and other fabric, small area rugs and soft articles. Vacuum upholstered furniture and drapes, and discard the vacuum cleaner bag. Press duct tape to furniture to remove any hair the vacuum missed.
Do you have to touch ringworm to get it?
Ringworm spreads easily from person to person, especially in communal areas like locker rooms and neighborhood pools. Ringworm is so contagious, in fact, that you don’t even have to touch someone to get infected. The fungus can linger in places like locker room floors, as well as on hats, combs, and brushes.
How do you test for mucormycosis?
Medical professionals diagnose mucormycosis with a medical history and physical exam. They may also take fluid or tissue samples send them to a lab. Other tests may include CT scan or MRI. There are no specific blood tests to detect mucormycosis.
Is mucormycosis contagious?
It is a non-contagious disease. It belongs to a fungal family of Mucorales.
Can mucormycosis recur after surgery?
“The recurrence is a rule rather than an exception in mucormycosis. Currently, the incidence of recovered patients requiring a revision operation is around 20%,” said ENT surgeon Samir Joshi, who is the head of the department and professor of ENT at Sassoon General Hospital.