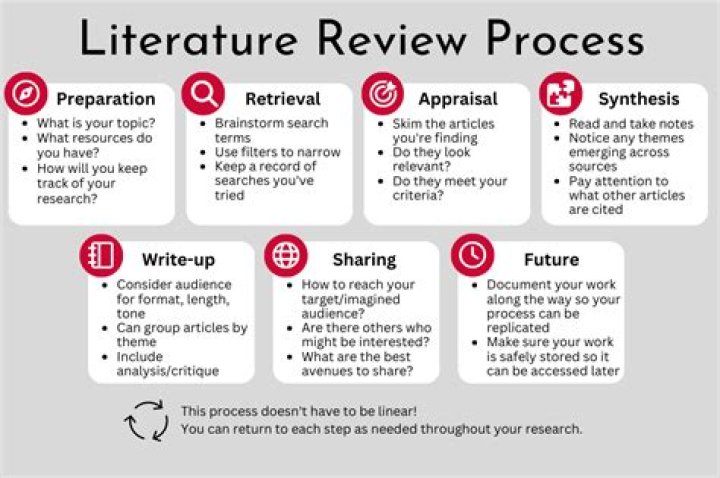
How is cuff pressure measured
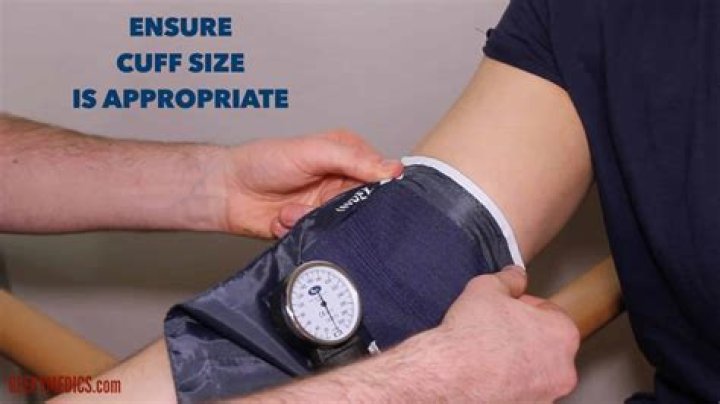
Cuff pressures were measured using aneroid manometer. ETT cuff pressure of 20-30 cm of water was considered as standard. Results: In 69% of the patients, the cuff pressure measurements were above the standard. Age (P = 0.806), weight (P = 0.527), height (P = 0.850), and gender (P = 1.00) were comparable in both groups.
What is normal cuff pressure?
The cuff is inflated to seal the airway to deliver mechanical ventilation. A cuff pressure between 20 and 30 cm H2O is recommended to provide an adequate seal and reduce the risk of complications. Survey results5–7 indicate that cuff pressure is usually monitored and adjusted every 8 to 12 hours.
How often should cuff pressure be measured?
The authors recommended to measure intracuff pressure every 8–24 h because the air inside the cuff may escape from the endotracheal cuff surface or through the pilot balloon valve [56, 57].
How do you measure the cuff pressure on a tracheostomy?
- Attach the cuff pressure manometer to the pilot balloon of the tracheostomy tube.
- Note the pressure reading, which should be 20-25mmHg.
- If it is not, adjust the pressure reading to 20-25mmHg by inflating the cuff with air to increase the pressure, or by removing air from the cuff to decrease the pressure.
What is trach cuff pressure?
Cuff pressure should be maintained between 15-30 cm H2O (up to 22 mm Hg) . A pressure manometer is a hand hand held device used to measure tracheostomy tube cuff pressures.
What is a cuff manometer?
From what I understand, a cuff manometer is used to measure the pressure of the cuff on an endotracheal tube. This can be important when ascending in an unpressurized cabin of a non-standard air evacuation platform.
What is cuff pressure manometer?
Pulmodyne cuffcheck is a low pressure cuff manometer used to safely inflate patient tracheal tubes. This manometer is a reliable and easy way to prevent over or under inflated cuff. Brand: Pulmodyne.
When will the cuff be inflated on a tracheostomy tube?
Inflate cuff 24 hours following initial tracheostomy tube placement (prevents accumulation of subcutaneous air and aspiration of secretions) Manual assisted ventilation/mechanical ventilation. Meals or nasogastric tube feedings for 30 minutes after if problems with aspiration are anticipated.Why is it important to measure cuff pressures?
The importance of ETT cuff pressures is highlighted by the spectrum of complications that can occur outside the ideal pressure range. High cuff pressures can result in complications ranging from sore throat and hoarseness[16,17] to tracheal stenosis, necrosis, and even rupture[18-21].
How do you control cuffs?- Stay hydrated: Drink lots of water to thin mucus.
- Inhale steam: Take a hot shower, or boil water and pour into a bowl, face the bowl (stay at least 1 foot away), place a towel over the back of your head to form a tent and inhale. …
- Use a humidifier to loosen mucus.
How much air do you put in ET cuff?
Sultan et al2 noted that the ET tube cuff should be inflated to the minimum volume at which no air leak is present with positive pressure inspira- tion and should remain less than 25 cm H2O.
How is ET tube size measured?
The ETT is measured from the distal end of the tube and is typically marked in 2 cm increments. After successfully intubating the patient the depth of the endotracheal tube ending at the teeth or lips should be noted.
What is the maximum recommended range for tracheal tube cuff pressures?
Cuff pressures greater than 30 cmH2O impede mucosal capillary blood flow. Multiple prior studies have recommended 30 cmH2O as the maximum safe cuff inflation pressure.
Why do tracheostomy have cuffs?
Cuffed tubes allow positive pressure ventilation and prevent aspiration. If the cuff is not necessary for those reasons, it should not be used because it irritates the trachea and provokes and trap secretions, even when deflated.
How does a cuffed tracheostomy work?
A cuff is a balloon attached around the outside of the tube. The cuff is inflated by filling the pilot balloon with air, which fills the cuff. When inflated, the cuff seals against the inside walls of the airway. A cuff is necessary when a patient is on a mechanical ventilator.
What is an airway cuff?
The cuff of the endotracheal tube (ETT) is designed to provide a seal within the airway, allowing airflow through the ETT but preventing passage of air or fluids around the ETT.
How do you use a Posey Cufflator?
Connect the extension tube to the cuff inflation line and to the Posey Cufflator. Use the hook on the back of the Posey Cufflator to hang it on the headboard of the bed. The Posey Cufflator will now monitor the intra-cuff pressure continuously and can be inflated or deflated as required.
When do you inflate and deflate a cuff?
When neither mechanical ventilation or a risk of gross aspiration is present, the cuff should be deflated. Another consideration is to change the patient to a cuffless tracheostomy tube. The definition of aspiration is when any food, liquid, or other matter passes below the vocal folds.
How do you measure a cuff leak?
Introduction. The cuff-leak test has been proposed as a simple method to predict the occurrence of post-extubation stridor. The test is performed by cuff deflation and measuring the expired tidal volume a few breaths later (VT). The leak is calculated as the difference between VT with and without a deflated cuff.
What device measures cuff pressure?
Cuff pressures were measured using aneroid manometer. ETT cuff pressure of 20–30 cm of water was considered as standard.
What is the difference between cuffed and uncuffed Trach?
Tracheostomy tubes can be cuffed or uncuffed. Uncuffed tubes allow airway clearance but provide no protection from aspiration. Cuffed tracheostomy tubes allow secretion clearance and offer some protection from aspiration, and positive-pressure ventilation can be more effectively applied when the cuff is inflated.
Can you suction a trach with cuff down?
This removes air from the cuff of the tracheostomy tube. Perform tracheal suctioning while deflating the cuff to attempt to remove secretions that have passed into the lower airways, preventing them from falling into the lungs. The cuff can be fully deflated or partially deflated for leak speech.
What is a low volume high pressure cuff?
[1] Low volume high pressure cuff was used in early ETs but replaced by high volume low pressure (HVLP) cuff because the former causes mucosal injury along the lateral tracheal wall. HVLP cuffs appeared ideal because they are capable of producing a seal with low pressure.
How many CCS is a ETT cuff?
The CIV range of 6-7 cc resulted in the highest likelihood of achieving the desired cuff pressure range, while cuffs inflated with 8-10 cc resulted in dangerously high CPs in all instances.
What size ET tube is typically used for oral intubation of a male patient?
Generally, in patients intubated only for the purposes of a general anesthetic, a smaller ETT may be used than on the patient who will remain intubated in the medium to long term as a result of respiratory failure; typically a 7-mm ETT is used for women and a 7.5- or 8-mm ETT is used for men.
Are cuffed ETT the same size as uncuffed?
Put another way, a 3.0 cuffed ETT has roughly the same outer diameter of a 3.5 uncuffed ETT. Under spontaneous ventilation, this difference matters as the work of breathing through a larger tube is less than that of a smaller tube.
How do you measure an endotracheal tube for a child?
- Uncuffed endotracheal tube size (mm ID) = (age in years/4) + 4.
- Cuffed endotracheal tube size (mm ID) = (age in years/4) + 3.
How do you check placement of endotracheal tube?
Clinical signs of correct ETT placement include a prompt increase in heart rate, adequate chest wall movements, confirmation of position by direct laryngoscopy, observation of ETT passage through the vocal cords, presence of breath sounds in the axilla and absence of breath sounds in the epigastrium, and condensation …
What are the 3 conditions that require airway management?
Indications for the use of airway management are: (1) failure to oxygenate; (2) failure to ventilate; (3) failure to maintain a patent airway.
Which is a potential complication of a low pressure in the endotracheal tube cuff?
Which of the following is a potential complication of a low pressure in the ET cuff? Low pressure in the cuff can increase the risk for aspiration pneumonia. High cuff pressure can cause tracheal bleeding, ischemia, and pressure necrosis.
Can you talk with a cuffed trach?
Cuffed tubes usually are used in acute care and for mechanically ventilated patients. When the cuff is inflated, air must pass through the tracheostomy tube to enter and exit the lungs. Because air no longer passes over the vocal cords, speech isn’t possible.