How is DRG pricing calculated
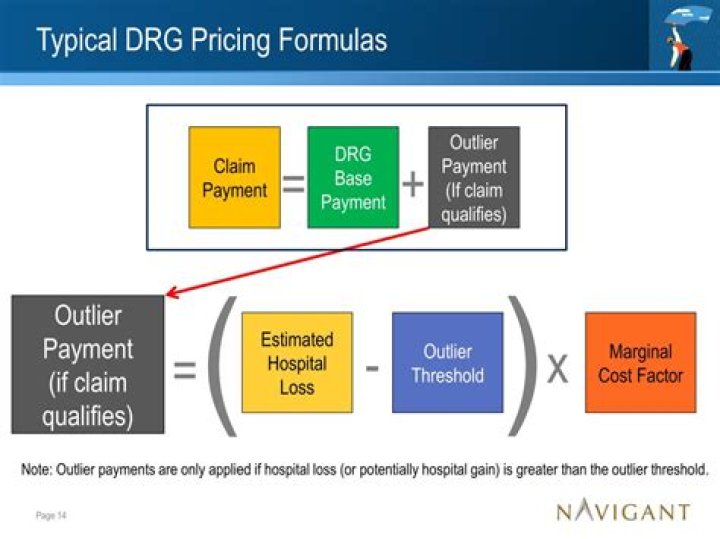
To figure out how much money your hospital got paid for your hospitalization, you must multiply your DRG’s relative weight by your hospital’s base payment rate. Here’s an example with a hospital that has a base payment rate of $6,000 when your DRG’s relative weight is 1.3: $6,000 X 1.3 = $7,800.
How does DRG pricing work?
Instead of paying for each day you’re in the hospital and each Band-Aid you use, Medicare pays a single amount for your hospitalization according to your DRG, which is based on your age, gender, diagnosis, and the medical procedures involved in your care.
How CMS calculate DRG weights?
The DRG weight is multiplied by the hospital’s payment rate per case. All hospitals are reimbursed on the basis of one of two Federal rates–“large urban” or “other.”34 These rates are adjusted to reflect differences in prevailing wage rates.
How are APR DRGs calculated?
Just as with MS-DRGs, an APR-DRG payment is calculated by using an assigned numerical weight that is multiplied by a fixed dollar amount specific to each provider. Each base APR-DRG, however, considers severity of illness and risk of mortality instead of being based on a single complication or comorbidity.How is DRG relative weight calculated?
The DRG relative weights are estimates of the relative resource intensity of each DRG. These weights are computed by estimating the average resource intensity per case for each DRG, measured in dollars, and dividing each of those values by the average resource intensity per case for all DRG’s, also measured in dollars.
How are DRGs or MS DRGs developed and calculated?
The formula used to calculate payment for a specific case multiplies an individual hospital’s payment rate per case by the weight of the DRG to which the case is assigned. … In a small number of MS-DRGs, classification is also based on the age, sex, and discharge status of the patient.
How does Medicare determine reimbursement rates?
The Centers for Medicare and Medicaid Services (CMS) determines the final relative value unit (RVU) for each code, which is then multiplied by the annual conversion factor (a dollar amount) to yield the national average fee. Rates are adjusted according to geographic indices based on provider locality.
What is 3M APR DRG?
Developed by 3M, APR DRGs stands for All Patient Refined Diagnosis Related Groups, a classification system designed to accurately identify how sick a patient population is compared to peer organizations. … The 3M APR DRGs include four severity-of-illness levels and four risk-of mortality levels within each DRG.Does Medicare use DRGs to reduce costs?
The use of DRGs does not appear to be related to the amount of costs that Medicaid does not pay and that hospitals, therefore, must seek from other payers. There is no relationship between the use of DRGs and the extent to which the Medicaid program covers the full cost of care for Medicaid patients.
What is used to define a newborn APR DRG?Here are some important definitions that impact the MS-DRG assignment: … Neonate – an infant less than four weeks old. Prematurity – the birth weight of 1,000-2,499 grams, or gestational age of 27-36 completed weeks of gestation.
Article first time published onWhat is the difference between DRG and APR DRG?
AP-DRGs are similar to DRGs, but also include a more detailed DRG breakdown for non-Medicare patients, particularly newborns and children. The APR-DRG structure is similar to the AP-DRG, but also measures severity of illness and risk of mortality in addition to resource utilization.
How do you calculate case mix index for MS-DRG?
Case mix index is calculated by adding up the relative Medicare Severity Diagnosis Related Group (MS-DRG) weight for each discharge, and dividing that by the total number of Medicare and Medicaid discharges in a given month and year.
What is a DRG What is difference between a DRG and a MS-DRG?
In 1987, the DRG system split to become the All-Patient DRG (AP-DRG) system which incorporates billing for non-Medicare patients, and the (MS-DRG) system which sets billing for Medicare patients. The MS-DRG is the most-widely used system today because of the growing numbers of Medicare patients.
What is a grouper code?
The Grouper allows users to enter one or more ICD-10-CM diagnosis codes and any applicable ICD-10-PCS procedure codes along with some other required inputs, click a button, and quickly get the resulting DRG and other important information (including the Relative Weight, Length of Stay, Procedure Type, Post Acute …
What is the 72 hour rule?
The 72-Hour Rule is a courtesy that may be extended to a camp as an option for. the director to get his or her hands on missing documentation.
How are hospitals paid by Medicare?
Inpatient hospitals (acute care): Medicare pays hospitals per beneficiary discharge, using the Inpatient Prospective Payment System. The base rate for each discharge corresponds to one of over 700 different categories of diagnoses—called Diagnosis Related Groups (DRGs)—that are further adjusted for patient severity.
Does length of stay affect MS DRG reimbursement?
GMLOS: Geometric Mean Length of Stay—used to compute reimbursement. It is statistically adjusted value for all cases for a given DRG.
What are the 3 DRG options?
There are currently three major versions of the DRG in use: basic DRGs, All Patient DRGs, and All Patient Refined DRGs. The basic DRGs are used by the Centers for Medicare and Medicaid Services (CMS) for hospital payment for Medicare beneficiaries.
How is Medicare allowable calculated?
The GPCIs are applied in the calculation of a fee schedule payment amount by multiplying the RVU for each component times the GPCI for that component. The Medicare limiting charge is set by law at 115 percent of the payment amount for the service furnished by the nonparticipating physician.
How do you calculate insurance reimbursement?
Take a look at your contract with insurance company. This contract will include the rates you’ll be reimbursed. (Usually, this is at the bottom of your contract, but each will vary.) You may decide to record them someplace easy and accessible.
What are the three components of the RVU?
Medicare Reimbursement in Calculated To understand this more fully, the calculations can be broken into three components – RVUs, the geographical adjustment and the conversion factor.
What are the pros and cons of DRG?
The advantages of the DRG payment system are reflected in the increased efficiency and transparency and reduced average length of stay. The disadvantage of DRG is creating financial incentives toward earlier hospital discharges. Occasionally, such polices are not in full accordance with the clinical benefit priorities.
Why is geriatric care in high demand?
Geriatric care is in high demand because people are living longer. As a result of wellness awareness, health care facilities have developed wellness centers to help people make healthy decisions. Methods of cost containment include outpatient services, preventive care, and energy conservation.
How are DRGs impacted with quality of care?
Studies have found no deterioration in the quality of care rendered to Medicare beneficiaries. … The success of the PPS/DRG system in controlling costs and promoting quality in this country suggests its application in other countries, either as a method of reimbursement or as a product line management tool.
Who owns APR DRG?
3M™ All Patient Refined Diagnosis Related Groups (APR DRGs) | 3M.
How many APR DRG codes are there?
There are 315 base APR-DRGs (version 27.0). Each APR-DRG is subdivided into four severity of illness subclasses and four risk of mortality subclasses. In addition there are two error APR-DRGs (955,956) that are not subdivided into subclasses.
What is the current version of APR DRG?
APR DRG version 38.0 will be accompanied by updates of the Methodology Overview, the Definitions Manual, the Summary of Changes document, and the Weights and Trims with Code Descriptions spreadsheet.
What is APR DRG reimbursement?
All Patients Refined Diagnosis Related Groups (APR DRG) is a classification system that classifies patients according to their reason of admission, severity of illness and risk of mortality.
What does DRG 794 mean?
DRG. 794. DRG 794 NEONATE WITH OTHER SIGNIFICANT PROBLEMS. Principal or secondary diagnosis of newborn or neonate,with other significant problems, not assigned to DRG 789 through 793 or 795. PRINCIPAL OR SECONDARY DIAGNOSIS.
How is severity calculated?
To determine the severity of illness score for an individual case, a rater scores each of the seven dimensions into one of four levels of increasing severity by examining data in the patient’s medical record following discharge.
Is DRG a bundled payment?
Medicare’s diagnosis-related groups (DRGs), which were introduced in 1983, are essentially bundled payments for hospital services, categorized by diagnosis and severity.