How much oxygen is in a face mask
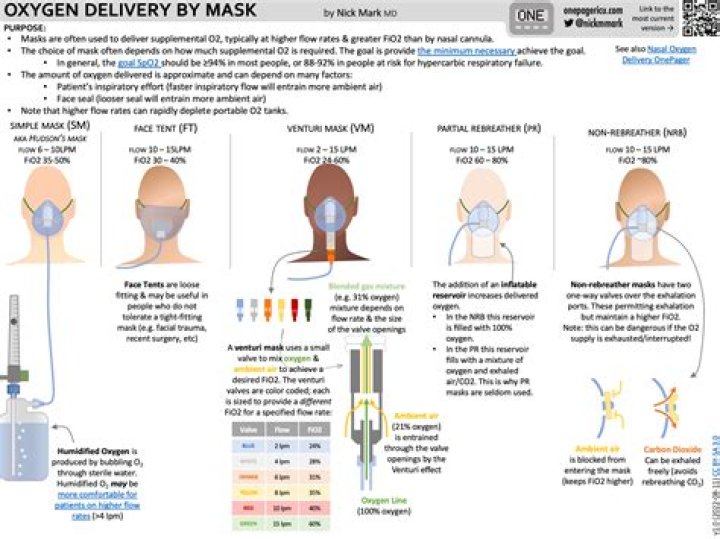
Cloth masks and surgical masks do not provide an airtight fit across the face. The CO2 escapes into the air through the mask when you breathe out or talk. CO2 molecules are small enough to easily pass through mask material. In contrast, the respiratory droplets that carry the virus that causes COVID-19 are much larger than CO2, so they cannot pass as easily through a properly designed and properly worn mask.
Does wearing a mask increase your CO2 intake?
Cloth masks and surgical masks do not provide an airtight fit across the face. The CO2 escapes into the air through the mask when you breathe out or talk. CO2 molecules are small enough to easily pass through mask material. In contrast, the respiratory droplets that carry the virus that causes COVID-19 are much larger than CO2, so they cannot pass as easily through a properly designed and properly worn mask.
Does wearing a face mask cause dizziness and headaches?
Wearing a cloth mask will not cause dizziness, lightheadedness, and headaches (also known as hypercapnia or carbon dioxide toxicity). Carbon dioxide passes through the mask, it does not build up inside the mask.
Does wearing a mask harm your health?
No, wearing a mask will not harm your health even if you are sick with a cold or allergies. If your mask gets too moist just make sure you are changing it regularly.What SpO2 oxygen level is normal for COVID-19 patients?
An SpO2 of 100% has effectively zero clinical difference to a 96% reading. As a good rule of thumb, a person with COVID-19 monitoring his or her clinical status at home will want to ensure that the SpO2 reading stays consistently at or above 90 to 92%.
Should people with COPD wear a mask during the COVID-19 pandemic?
Wearing a mask with COPD can be difficult. Yet the Centers for Disease Control and Prevention (CDC) recommends that people wear masks to help slow the spread of the coronavirus.
What are the risks of wearing an extra mask during the COVID-19 pandemic?
Adding an extra layer or mask could block vision. Reduced vision could lead to trips, falls, or other injuries.
What happens if I don’t wear a mask in an indoor area or a public transportation during the COVID-19 pandemic?
On conveyances with no outdoor spaces, operators of public transportation conveyances must refuse to board anyone not wearing a mask that completely covers the mouth and nose. On conveyances with outdoor areas, operators must refuse to allow entry to indoor areas to anyone not wearing a mask.Why do my ears hurt after wearing a face mask during the COVID-19 pandemic?
A mask’s ear loops can make your ears sore. Elastic straps pull on your ears and put pressure on your skin, which can become irritated.
Is dizziness a neurological symptom of COVID-19?An earlier published study from China found dizziness to be the most common neurological manifestation of COVID-19. Dizziness was proposed to occur ensuing the neuroinvasive potential of severe acute respiratory syndrome coronavirus 2 or SARS-CoV-2 virus which causes COVID-19.
Article first time published onCould headache be a symptom of COVID-19?
Most people infected with SARS-CoV-2 virus will have no or mild to moderate symptoms associated with the brain or nervous system. However, most hospitalized patients do have symptoms related to the brain or nervous system, most commonly including muscle aches, headaches, dizziness, and altered taste and smell.
How can I measure the oxygen level of my blood during the COVID-19 pandemic?
You can measure your blood oxygen level with a pulse oximeter. That’s a small device that clips onto your fingertip. It shines a light into the tiny blood vessels in your finger and measures the oxygen from the light that’s reflected back.
Can the coronavirus disease cause breathing problems?
COVID-19 is a respiratory disease, one that especially reaches into your respiratory tract, which includes your lungs. COVID-19 can cause a range of breathing problems, from mild to critical.
Does wearing a cloth mask over a medical one reduce exposure to COVID-19 more than wearing just one mask?
Based on experiments that measured the filtration efficiencies of various cloth masks and a medical procedure mask (6), it was estimated that the better fit achieved by combining these two mask types, specifically a cloth mask over a medical procedure mask, could reduce a wearer’s exposure by >90%.
Are people with chronic lung diseases at a higher risk of getting severely ill from COVID-19?
Chronic lung diseases can make you more likely to get severely ill from COVID-19.
Does having multiple medical conditions increase the risk of a severe illness from COVID-19?
Certain underlying medical conditions increased risk for severe COVID-19 illness in adults. Having multiple conditions also increased risk. Obesity, diabetes with complications, and anxiety and fear-related disorders had the strongest association with death. The risk associated with a condition increased with age.
Can I still have sex during the coronavirus pandemic?
If both of you are healthy and feeling well, are practicing social distancing and have had no known exposure to anyone with COVID-19, touching, hugging, kissing, and sex are more likely to be safe.
What are some of the common symptoms of the COVID-19 disease?
Symptoms may include: fever or chills; cough; shortness of breath; fatigue; muscle and body aches; headache; new loss of taste or smell; sore throat; congestion or runny nose; nausea or vomiting; diarrhea.
How do you breathe in COVID-19 face masks?
Masks must be worn over your mouth and nose. Yes, breathing through a mask can take some getting used to, but don’t lower your mask to breathe through your nose. When you don’t have the mask over your nose, you are breathing or sneezing potentially infectious particles into the air around you.
Are passengers required to wear masks on public conveyance during the COVID-19 pandemic?
CDC issued an Order, effective February 2, 2021 requiring the wearing of masks by travelers (both passengers and crew) on public conveyances to prevent the spread of COVID-19. Conveyance operators must require all persons onboard to wear masks when boarding, disembarking, and for the duration of travel.
Could COVID-19 cause neurological problems?
While primarily a respiratory disease, COVID-19 can also lead to neurological problems. The first of these symptoms might be the loss of smell and taste, while some people also may later battle headaches, debilitating fatigue, and trouble thinking clearly, sometimes referred to as “brain fog.”
What are some of the neurologic complications from COVID-19?
It is clear that COVID can cause brain damage by direct infection (encephalitis), by strokes, and by lack of oxygen. It is also clear that when patients experience severe illness requiring an ICU stay, brain damage is highly likely to occur, and its effects are typically obvious.
Does COVID-19 affect the brain?
The most comprehensive molecular study to date of brain tissue from people who died of COVID-19 provides clear evidence that SARS-CoV-2 causes profound molecular changes in the brain, despite no molecular trace of the virus in brain tissue.
When can COVID-19 symptoms begin to appear?
Symptoms may appear 2-14 days after someone is exposed to the virus and can include fever, chills, and cough.
When do you start developing symptoms of the coronavirus disease?
Signs and symptoms of coronavirus disease 2019 (COVID-19) may appear two to 14 days after exposure. This time after exposure and before having symptoms is called the incubation period.
What do I do if I have mild symptoms of COVID-19?
If you have milder symptoms like a fever, shortness of breath, or coughing: Stay home unless you need medical care. If you do need to go in, call your doctor or hospital first for guidance. Tell your doctor about your illness.
How long does the post-COVID condition last?
Although most people with COVID-19 get better within weeks of illness, some people experience post-COVID conditions. Post-COVID conditions are a wide range of new, returning, or ongoing health problems people can experience more than four weeks after first being infected with the virus that causes COVID-19.
How long can a patient still feel the effects of COVID-19 after recovery?
Older people and people with many serious medical conditions are the most likely to experience lingering COVID-19 symptoms, but even young, otherwise healthy people can feel unwell for weeks to months after infection.
What SpO2 oxygen level is normal for COVID-19 patients?
An SpO2 of 100% has effectively zero clinical difference to a 96% reading. As a good rule of thumb, a person with COVID-19 monitoring his or her clinical status at home will want to ensure that the SpO2 reading stays consistently at or above 90 to 92%.
How does COVID-19 affect the blood?
Some people with COVID-19 develop abnormal blood clots, including in the smallest blood vessels. The clots may also form in multiple places in the body, including in the lungs. This unusual clotting may cause different complications, including organ damage, heart attack and stroke.