How much pleural fluid is drained
Removal of 400-500 mL of pleural fluid is often sufficient to alleviate shortness of breath. The recommended limit is 1000-1500 mL in a single thoracentesis procedure.
How much can you drain pleural effusion?
Pleural fluid drainage should to be started immediately and up to 1500 mL of fluid can be removed. After removing the pleural fluid, a chest radiograph or postprocedural CT scan should be obtained to confirm the appropriate position of the pigtail catheter and evaluate possible complications including pneumothorax.
How much chest tube drainage is normal?
Compared to a daily volume drainage of 150 ml, removal of chest tube when there is 200 ml/day is safe and will even result in a shorter hospital stay.
How much fluid is typically drained from the lung?
A thoracentesis is a procedure used to drain excess fluid from the space outside of the lungs but inside the chest cavity. Normally, this area contains about 20 milliliters of clear or yellow fluid. If there’s excess fluid in this area, it can cause symptoms such as shortness of breath and coughing.How many liters is pleural effusion?
Mild symptoms suggestive of re-expansion oedema are common after large volume thoracentesis in pleural effusion with patients experiencing discomfort and cough. It is recommended that no more than approximately 1.5 litres should be drained at any one time or drainage should be slowed to<500 ml h−1.
Does pleural effusion mean Stage 4?
Metastatic pleural effusion from lung cancer has a particularly poor prognosis, and in NSCLC it is actually reclassified as stage IV disease.
How much pleural fluid is produced per day?
Pleural fluid production (approximately 15-20 mL/day) [4] is dependent on the same Starling forces that govern the movement of fluid between vascular and interstitial spaces throughout the body.
When should pleural drain be removed?
Chest tubes are commonly used to drain fluid following surgery involving the pleural space. Removal can be considered when there is no empyema or air leak, and fluid drainage has decreased to an acceptable level.How much should a chest tube drain per hour?
7.1 Place container upright on floor. 7.2 Mark and date drainage, at eye level, on collection chamber. 7.3 Record. Pediatric: 3 mL/Kg/hour in a 3 hour period or 5 to 10 mL/Kg in any 1 hour period.
Do you empty chest tube drainage?If fluid is draining from your chest, it will flow through your chest tube and into your Pneumostat’s collection chamber. The collection chamber can hold up to 30 milliliters (mL) of fluid. Empty it before it fills up to the 30 mL mark, so it doesn’t overflow (see Figure 5).
Article first time published onHow much fluid is usually removed during a thoracentesis?
Traditional guidelines recommend that the volume of fluid removed during a thoracentesis should be limited to <1.5 liters, to avoid re-expansion pulmonary edema.
Where does fluid in pleural space come from?
Transudative pleural effusion is caused by fluid leaking into the pleural space. This is from increased pressure in the blood vessels or a low blood protein count. Heart failure is the most common cause.
Where does pleural effusion drain?
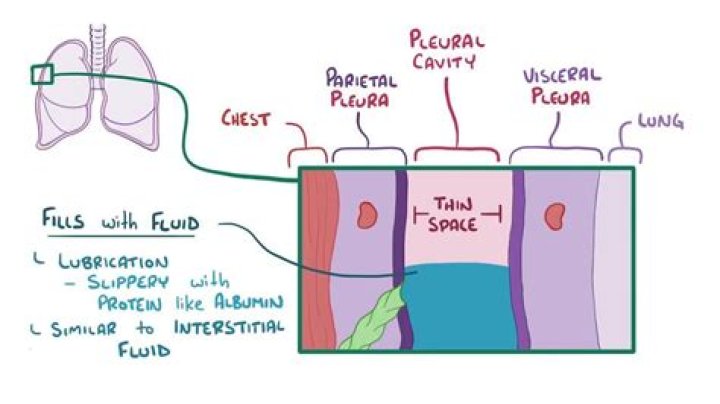
Thoracentesis is a procedure to remove fluid or air from around the lungs. A needle is put through the chest wall into the pleural space. The pleural space is the thin gap between the pleura of the lung and of the inner chest wall.
Where does fluid in pleural effusion come from?
Pleural effusion occurs when fluid builds up in the space between the lung and the chest wall. This can happen for many different reasons, including pneumonia or complications from heart, liver, or kidney disease. Another reason could be as a side effect from cancer.
Can pleural effusion causes death?
The presence of a pleural effusion indicates a high risk of death, with 15% of patients dying within 30 days and 32% dead within one-year of hospital admission.
How long can I live with pleural effusion?
Malignant pleural effusion (MPE) is a common but serious condition that is related with poor quality of life, morbidity and mortality. Its incidence and associated healthcare costs are rising and its management remains palliative, with median survival ranging from 3 to 12 months.
Is draining fluid from lungs painful?
A needle is inserted between your ribs into the pleural space. You may feel some discomfort or pressure when the needle is inserted. As your doctor draws out excess fluid from around your lungs, you may feel like coughing or have chest pain.
When are chest tubes removed for pleural effusion?
If placement was for any pleural fluid drainage, once the drainage volume is less than 200 ml in a 24-hour period,3,5 the fluid is serous, the lung has re-expanded on the chest film, and the patient’s clinical status has improved, the chest tube may be removed.
How long does a chest drain last?
Your doctors will discuss with you how long the drain needs to stay in. This may be from between one day to one to two weeks, depending on how well you are responding to treatment. You may need to have several chest X-rays during this time to see how much fluid or air remains.
How deep should a chest tube go?
For most patients, 10 cm is an adequate and safe depth of insertion. Very large people may require 12-14 cm. Insertion beyond these depths risks injury to the lung, cardiac, and mediastinal structures, especially if you were unsuccessful at guiding the tube toward the apex (see #4).
How long can a chest tube be left in?
Following lung cancer surgery, the tube will be left in place until only minimal drainage remains, often a period of three to four days.
How long can a PleurX catheter stay in?
Notify your doctor if you continue to feel short of breath after draining 1000mL of fluid. How long will the catheter be in my chest or abdomen? Chest: The catheter will be in your chest until fluid stops draining. The amount of time will vary from patient to patient, anywhere from a few weeks to several months.
How do you remove a pleural drain?
- Remove the dressing and anchor tape using clinically clean gloves.
- Prepare sterile field.
- Prepare occlusive dressing.
- Discuss the procedure with assistant to ensure a coordinated approach.
- Perform hand hygiene.
- Don full PPE (gown, mask, gloves, goggles).
How painful is chest tube removal?
The presence of chest drains is synonymous of postoperative pain and its withdrawal is a discomfort to the patient. The pain during the removal is characterized as one of the most distressing for patients and some have reported as the worst memory during hospitalization.
Can a nurse insert a chest tube?
Advanced practice registered nurses and physician assistants perform chest tube insertions as well as trauma surgeons do.
What does the color of pleural effusion mean?
Pale yellow fluid may be associated with exudates; bloody fluid with malignancy, trauma, and pulmonary infarction; black with an Aspergillus infection; and dark green with bilothorax. The WBC and differential are also used to help determine the cause of a pleural effusion.
Can fluid around the lungs be cured?
You can have treatment to stop fluid from building up and help relieve symptoms. This treatment is called pleurodesis. It seals the space between the tissues covering the lung by using sterile talc to make them inflamed so they stick together.
How serious is fluid on the lungs in elderly?
Fluid in Lungs: Elderly Prognosis It’s fairly common for seniors to suffer from fluid in the lungs, but getting a good prognosis depends on understanding the underlying cause. Most cases are the result of heart problems, which is why acute pulmonary edema has a one-year mortality rate of about 40% for elderly patients.
What purpose does pleural fluid serve?
Structure and Function of Pleural Fluid Pleural fluid functions by lubricating the space between the pleura, allowing the pleura to glide smoothly during inhalation and exhalation. In this way, it cushions delicate lung tissues against friction from the ribs and the chest wall itself.
What is a permanent lung drain?
IPCs are designed to be a permanent solution to the problem of fluid in the pleural space (though they can be removed if they are no longer needed). There is a soft cuff around the tube, which is positioned under the skin. The skin heals and attaches to this cuff, making the drain more secure.
What happens if you don't drain a pleural effusion?
The most common cancers of this type include lung and breast cancers and lymphoma. An infection, such as pneumonia, can lead to inflammation of the lung. This, too, can be a contributing factor to pleural effusion. Without treatment, pleural effusion can be very serious and even life-threatening.