What are interstitial opacities
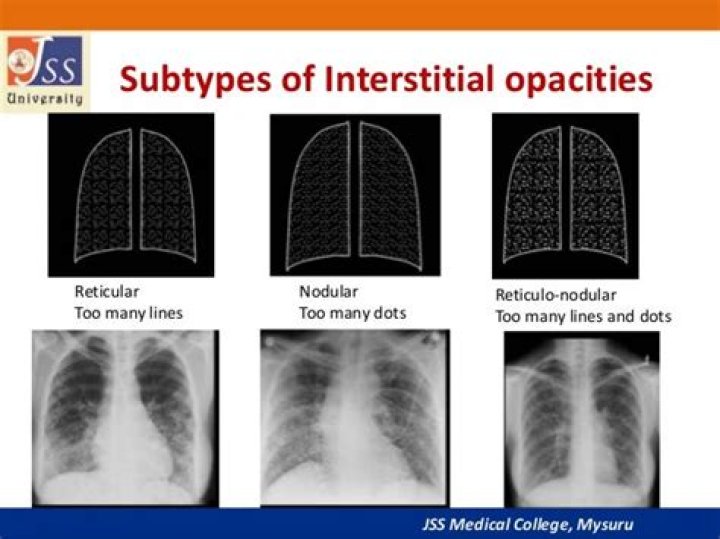
Interstitial (in-tur-STISH-ul) lung disease describes a large group of disorders, most of which cause progressive scarring of lung tissue. The scarring associated with interstitial lung disease eventually affects your ability to breathe and get enough oxygen into your bloodstream.
What is interstitial opacities in the lungs?
Interstitial (in-tur-STISH-ul) lung disease describes a large group of disorders, most of which cause progressive scarring of lung tissue. The scarring associated with interstitial lung disease eventually affects your ability to breathe and get enough oxygen into your bloodstream.
Is interstitial lung disease cancer?
The evidence supports an increased risk of lung cancer due to specific fibrotic and inflammatory lung diseases (termed interstitial lung diseases), including idiopathic pulmonary fibrosis, systemic sclerosis, and certain pneumoconioses.
How do you treat opacities in the lungs?
The current main treatment methods for pulmonary multifocal GGO are forming a troika including the following: surgery, stereotactic body radiation therapy (SBRT), and thermal tumor ablation (including radiofrequency ablation, microwave ablation, and cryoablation).Does Covid cause interstitial lung disease?
Residual pulmonary disease is sometimes referred to as “post-COVID interstitial lung disease” (ILD). In this issue of Radiology, Han and Fan et al (1) report on a prospective cohort of 114 patients with severe COVID-19 pneumonia undergoing CT during hospital admission and 6 months later.
What does the medical term interstitial mean?
Medical Definition of interstitial 1 : situated within but not restricted to or characteristic of a particular organ or tissue —used especially of fibrous tissue. 2 : affecting the interstitial tissues of an organ or part interstitial hepatitis.
What is the difference between COPD and interstitial lung disease?
In IPF, your lungs become scarred, stiff, and thick, and the progressive damage is not reversible. In COPD, the airways, which are branching tubes that carry air within the lungs, become narrow and damaged. This makes people feel out of breath and tired.
How long does ground-glass opacity last after Covid?
Conclusion. The majority of patients have altered PFT at three months, even in patients with mild initial disease, with significantly lower function in patients with residual CT lesions. Steroids do not seem to modify functional and radiological recovery. Long-term follow-up is needed.How long does Covid pneumonia last?
For the 15% of infected individuals who develop moderate to severe COVID-19 and are admitted to the hospital for a few days and require oxygen, the average recovery time ranges between three to six weeks.
Can ground-glass in lungs go away?Most clinicians have probably observed that a percentage of GGNs disappear spontaneously (a transient GGN). My research group found that 37% of pure GGNs (pGGNs) and 48% of mixed GGNs (mGGNs) regressed or disappeared within 3 months, which suggested their inflammatory nature (1).
Article first time published onHow long can you live with interstitial lung?
The average survival for people with this type is currently 3 to 5 years . It can be longer with certain medications and depending on its course. People with other types of interstitial lung disease, like sarcoidosis, can live much longer.
What is the best test to confirm interstitial lung disease?
Computerized tomography (CT) scan. This imaging test is key to, and sometimes the first step in, the diagnosis of interstitial lung disease. CT scanners use a computer to combine X-ray images taken from many different angles to produce cross-sectional images of internal structures.
What is the most common cause of interstitial lung disease?
A bacteria called Mycoplasma pneumoniae is the most common cause. Idiopathic pulmonary fibrosis. This makes scar tissue grow in the interstitium.
Is interstitial lung disease a terminal illness?
Interstitial lung disease (ILD), especially idiopathic pulmonary fibrosis (IPF), is a fatal disease with a poor prognosis, and the therapeutic options are limited.
Is interstitial lung disease painful?
Conclusion. In conclusion, pain is common in the patients with ILD and the pain intensity is associated with exposure history, 6MWD, and mMRC score. The patients with ILD and pain have more possibility to suffer depression, anxiety and impaired HRQoL.
How does interstitial lung progress?
Scarring Progresses When this happens, the body’s organs, like the heart and the brain, do not receive the oxygen they need to function properly. As chronic ILD with progressive fibrosis worsens, sheets of dense scar tissue replace normal lung tissue and shrink the size of the lung.
How is interstitial lung disease diagnosed?
- Spirometry. A spirometer is a device used to check lung function. …
- Peak flow monitoring. This device is used to measure how fast you can blow air out of the lungs. …
- Chest X-rays. …
- Blood tests. …
- CT scan. …
- Bronchoscopy. …
- Bronchoalveolar lavage. …
- Lung biopsy.
Is ILD an autoimmune disease?
Interstitial lung disease (ILD) refers to a broad category of conditions that produce inflammation and scarring in the lungs. Autoimmune ILD is caused specifically by autoimmune disorders, which involve the body’s own immune system attacking the lungs.
What is another name for interstitial?
Interstitial synonyms In this page you can discover 6 synonyms, antonyms, idiomatic expressions, and related words for interstitial, like: interspatial, substitutional, invagination, subendothelial, eosinophilic and perivascular.
What are interstitial spaces in the body?
The interstitial compartment (also called “tissue space”) surrounds tissue cells. It is filled with interstitial fluid, including lymph. Interstitial fluid provides the immediate microenvironment that allows for movement of ions, proteins and nutrients across the cell barrier.
What are symptoms after recovering from Covid?
In some people, lasting health effects may include long-term breathing problems, heart complications, chronic kidney impairment, stroke and Guillain-Barre syndrome — a condition that causes temporary paralysis. Some adults and children experience multisystem inflammatory syndrome after they have had COVID-19 .
How long can a person stay on a ventilator?
How long does someone typically stay on a ventilator? Some people may need to be on a ventilator for a few hours, while others may require one, two, or three weeks. If a person needs to be on a ventilator for a longer period of time, a tracheostomy may be required.
What does Covid do to your lungs?
In critical COVID-19 — about 5% of total cases — the infection can damage the walls and linings of the air sacs in your lungs. As your body tries to fight it, your lungs become more inflamed and fill with fluid. This can make it harder for them to swap oxygen and carbon dioxide.
How do you get rid of ground-glass opacities in the lungs?
In case of bacterial or viral infections, treating with intravenous antibiotics and other supportive medicine relieves the symptoms, and the haziness resolves spontaneously without any further management. In severe cases of ground-glass opacities, lobectomy surgery is used to remove the affected part of the lung.
What causes multifocal pneumonia?
Multifocal pneumonia can also be caused by a bacteria like streptococcus pneumoniae or legionella pneumophila, or a fungus like pneumocystis pneumonia, coccidioidomycosis, or cryptococcus, Dr. Casciari says. “Having multifocal pneumonia doesn’t automatically signify what’s causing the pneumonia,” he says.
How serious is a ground-glass lung nodule?
Women with pure ground-glass nodules “had a significantly higher relative risk of lung cancer than men with the same type of nodules, and a similar trend was observed for part-solid nodules,” according to RSNA. By contrast, the relative risk of lung cancer for solid nodules was comparable for both sexes.
How fast do ground glass opacities grow?
The doubling time for most malignant nodules is between 30 and 400 days. The absence of growth of solid nodule over at least a 2-year period is generally considered to be a reliable indicator of benignity.
What percentage of ground glass opacities are cancerous?
Pulmonary ground glass opacity (GGO) is becoming an important clinical dilemma in oncology as its diagnosis in clinical practice is increasing due to the introduction of low dose computed tomography (CT) scan and screening. The incidence of cancer in GGO has been reported as high as 63%.
Do inhalers help interstitial lung disease?
Patients may be prescribed quick-relief and long-acting controller inhalers, as well as undergo oxygen therapy to improve lung function.
How do people live with interstitial lung disease?
- Get vaccinated. …
- Take part in pulmonary rehabilitation (when prescribed). …
- Use oxygen therapy.
Can interstitial lung disease be misdiagnosed?
With vague symptoms, interstitial lung disease (ILD) is often overlooked or misdiagnosed. If that happens, the consequences can be grave.