What does dead space mean in medical terms
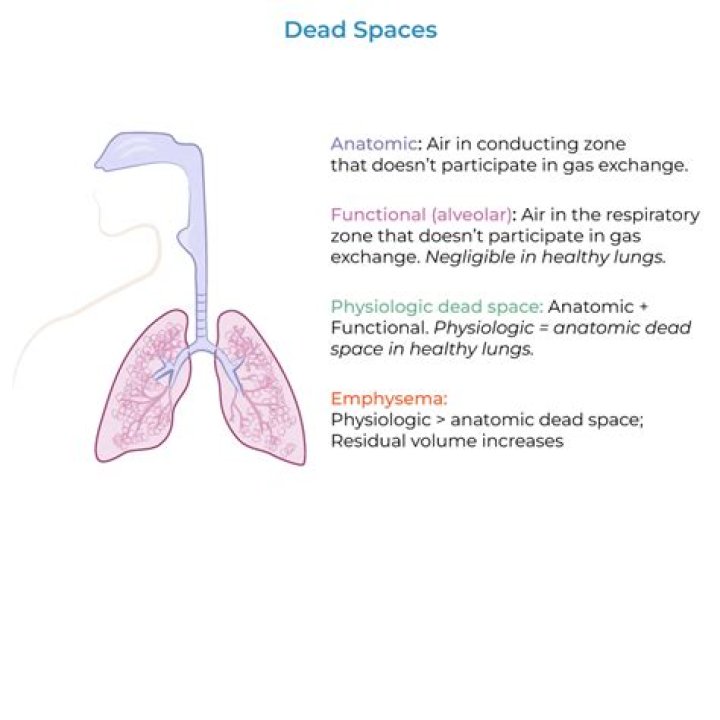
1 : space in the respiratory system in which air does not undergo significant gaseous exchange — see anatomical dead space, physiological dead space. 2 : a space (as that in the chest following excision of a lung) left in the body as the result of a surgical procedure.
What is the meaning of dead space?
Dead space is the volume of air that is inhaled that does not take part in the gas exchange, because it either remains in the conducting airways or reaches alveoli that are not perfused or poorly perfused. It means that not all the air in each breath is available for the exchange of oxygen and carbon dioxide.
What causes dead space in lungs?
The alveolar deadspace is caused by ventilation/perfusion inequalities at the alveolar level. The commonest causes of increased alveolar deadspace are airways disease–smoking, bronchitis, emphysema, and asthma. Other causes include pulmonary embolism, pulmonary hypotension, and ARDS.
What does dead space mean in surgery?
“Dead space” refers to the soft tissue and bony defect left behind after debridement. Appropriate management of this space is necessary to reduce the risk of persistent infection from poor vascularization of the area and to maintain the integrity of the skeletal part.What is an anatomical dead space?
Anatomic dead space specifically refers to the volume of air located in the respiratory tract segments that are responsible for conducting air to the alveoli and respiratory bronchioles but do not take part in the process of gas exchange itself.
How do you measure dead space?
The “anatomical” dead space is commonly measured by sampling an inert gas (N2) and volume in the exhalation following a large breath of oxygen (VD(F)). It may also be measured from an inert gas washout (VD(O)) that describes both volume and the delivery of VD(O) throughout the expiration.
What does the marker do in dead space?
Purposes. The ultimate purpose of the Markers is to create a Necromorph Moon (also known as Brethren Moons), by spreading an alien contagion that reanimates dead cells and kills all life in the area.
Can Dead Space cause hypoxemia?
If underlying pathophysiology causes a problem with ventilation and/or perfusion in the form of a shunt or dead space, the resultant VQ mismatch will cause hypoxemia.How do you calculate dead space in your lungs?
The equation states VD is equal to VT multiplied by the partial pressure of arterial carbon dioxide (PaCO2) minus partial pressure of expired carbon dioxide (PeCO2) divided by PaCO2. Breaking down this equation, there is the tidal volume which is the normal amount of inspired and expired gas equivalent to 500 mL.
What portions of the respiratory system are referred to as anatomical dead space and why?What portions of the respiratory system are referred to as anatomical dead space? And why? All but the respiratory zone structures (Respiratory bronchioles, alveolar ducts and sacs, and alveoli). Because no gas exchange occurs except in the respiratory zone, particularly in the alveoli.
Article first time published onWhat happens when dead space is increased?
At a fundamental level, increasing the dead space functionally indistinguishable from hypoventilation: Dead space is a fraction of the total tidal volume. Of the tidal volume, only the non-dead fraction participates in gas exchange. Ergo, increasing dead space has the same effect as reducing the tidal volume.
What are the two types of dead space?
The two types of dead space are anatomical dead space and physiologic dead space. Anatomical dead space is represented by the volume of air that fills the conducting zone of respiration made up by the nose, trachea, and bronchi.
What happens to dead space during exercise?
Figure 6. Dead space ventilation at differing levels of work. During exercise, dead space ventilation falls with increasing work, owing to increasing Vts. In the high–dead space group, dead space ventilation is significantly higher throughout exercise, and this difference is exaggerated with increasing work.
Why is it called the anatomical dead space?
The volume of air contained in this conducting zone is known as anatomic dead space. ‘Dead’ sounds kind of ominous but it basically reflects the fact that this air is as good as dead to the body, because you can’t extract oxygen from it.
Why does dead space increase with age?
Dead space increases with age because the larger airways increase in diameter. However, expiratory flow changes very little. After the age of 40, the diameter of the small airways decreases, but again, there is no change in airway resistance.
What are the aliens in Dead Space?
The Alien Necromorph is a Necromorph created from members of the nameless alien species native to Tau Volantis.
What are the monsters in Dead Space?
Several common varieties of Necromorph. Necromorphs are mutated corpses, reshaped into horrific new forms by a recombinant extraterrestrial infection derived from a genetic code etched into the skin of the Markers. The resulting creatures are extremely aggressive and will attack any uninfected organism on sight.
How does the Dead Space series end?
The ending to Dead Space happens after Isaac defeats the Hive Mind. He then boards the ship used to transport the marker, and quickly takes off from the planet, so as not to be killed by the falling rock.
How does tracheostomy reduce dead space?
Proponents of early tracheostomy argue that decreases in anatomic dead space lower airway resistance, allow lower peak inspiratory pressures and may even change dynamic compliance, resulting in reduction of the work of breathing, thus allowing patients to wean off the ventilator expeditiously and decrease ventilator …
Does spirometry measure dead space?
Lung function testing Anatomic dead space is defined as the volume of the conducting airways, where no gas exchange takes place (Fig. 50.7). … The subject then exhales to residual volume into the spirometer, during which continuous recordings of nitrogen concentration and volume are made.
Which situation will happen when you have emphysema?
In emphysema, the inner walls of the lungs’ air sacs (alveoli) are damaged, causing them to eventually rupture. This creates one larger air space instead of many small ones and reduces the surface area available for gas exchange. Emphysema is a lung condition that causes shortness of breath.
What is the difference between dead space and shunt?
The main difference between the shunt and dead space is that shunt is the pathological condition in which the alveoli are perfused but not ventilated, whereas dead space is the physiological condition in which the alveoli are ventilated but not perfused.
Does peep increased dead space?
Positive end-expiratory pressure (PEEP) increases arterial carbon dioxide tension and alveolar dead space by reducing alveolar capillary perfusion. … Both dead space/tidal volume ratio and arterial carbon dioxide tension remained significantly elevated with PEEP even with normal cardiac output.
Does dead space cause hypercapnia?
Nonetheless, energy is required to ventilate the physiological dead space, although neither oxygen gain nor carbon dioxide removal occurs. … Beyond that point, inadequate ventilation caused by extensive physiological dead space can lead to acute respiratory failure of the hypercapnic variety.
Does dead space improve with oxygen?
Dead spaces can severely impact breathing, because they reduce the surface area available for gas diffusion. As a result, the amount of oxygen in the blood decreases, whereas the carbon dioxide level increases.
Is pneumonia shunt or dead space?
A pulmonary shunt often occurs when the alveoli fill with fluid, causing parts of the lung to be unventilated although they are still perfused. Intrapulmonary shunting is the main cause of hypoxemia (inadequate blood oxygen) in pulmonary edema and conditions such as pneumonia in which the lungs become consolidated.
How does dead space affect minute ventilation?
Firstly, with low tidal volumes, the VD/VT increases as tidal volume decreases if VD remains constant. The weight of dead space increases in proportion of tidal volume decrease. … Consequently, for a steady minute ventilation, when the respiratory rate or the dead space are increased, alveolar ventilation is reduced.
How do you reduce ventilation in dead space?
Dead-space ventilation may be reduced by expiratory flushing of airways (1) or tracheal gas insufflation (2-4). By increasing alveolar ventilation, these methods may increase CO2 clearance.
Why is increased dead space bad?
Increasing the proportion of dead space to alveolar ventilation will lead to retention of carbon dioxide by the patient. If mechanical dead space volume equals or exceeds alveolar ventilation volume the patient will not be able to clear carbon dioxide at all.
What's the difference between anatomical and physiological dead space?
Anatomical dead space is the air-filled in conducting airways and does not participate in gas exchange. Meanwhile, physiological dead space is the sum of all parts of the tidal volume that does not participate in gas exchange.
Which term refers to relaxed quiet breathing?
Quiet breathing, also known as eupnea, is a mode of breathing that occurs at rest and does not require the cognitive thought of the individual. During quiet breathing, the diaphragm and external intercostals must contract. A deep breath, called diaphragmatic breathing, requires the diaphragm to contract.