What does Pip mean on a ventilator
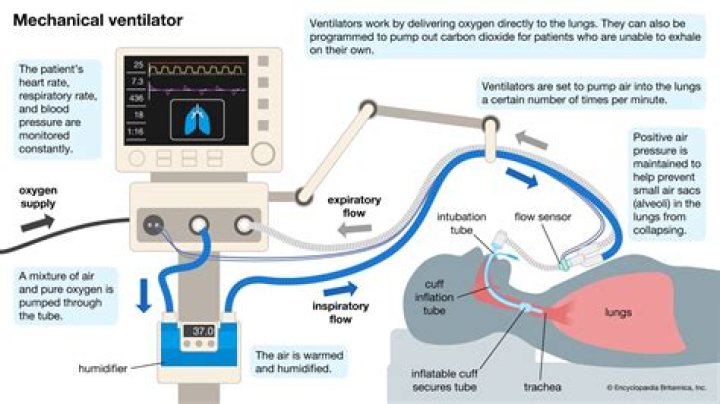
PIP: Total inspiratory work by vent; Reflects resistance & compliance; Normal ~20 cmH20 (@8cc/kg and adult ETT); Resp failure 30-40 (low VT use); Concern if >40. Pplat-PEEP: tidal stress (lung injury & mortality risk). Target < 15 cmH2O.
What is a normal PIP on ventilator?
PIP: Total inspiratory work by vent; Reflects resistance & compliance; Normal ~20 cmH20 (@8cc/kg and adult ETT); Resp failure 30-40 (low VT use); Concern if >40. Pplat-PEEP: tidal stress (lung injury & mortality risk). Target < 15 cmH2O.
What is the normal peak airway pressure?
Peak pressure is graphed as a summation of both initial airway resistance and lung compliance. In general, an acceptable maximum Ppeak is 40 cmH2O.
What is PIP and PEEP?
The difference between PEEP set and the pressure measured during this maneuver is the amount of auto-PEEP. PIP = peak inspiratory pressure. As illustrated here, the measured auto-PEEP can be considerably less than the auto-PEEP in some lung regions if airways collapse during exhalation.What is high PIP?
PIP. Elevated PIP possibly indicates: ○ Hyperventilation – Tidal volume to large, Breath stacking. ○ Poor compliance. Lung issues – Bronchospasm, alveolar collapse, consolidation in.
How do you fix high PIP on a ventilator?
- Increased PIP with normal pPLAT reflects increased airway resistance.
- Reduce airway resistance (suctioning, check ET Tube position, Bronchodilators) Evaluate for Endotracheal Tube obstruction. Consider kinked tubes. Suction for mucous plugs. Consider bronchospasm. …
- Consider increasing the Ventilator pressure limit (caution!)
Is PIP the same as peak?
Paw is airway pressure, PIP is peak airway pressure, Pplat is plateau pressure. Some researchers have suggested that plateau pressures should be monitored as a means to prevent barotrauma in the patient with ARDS.
What causes high PIP?
Peak inspiratory pressure increases with any airway resistance. Things that may increase PIP could be increased secretions, bronchospasm, biting down on ventilation tubing, and decreased lung compliance. PIP should never be chronically higher than 40(cmH2O) unless the patient has acute respiratory distress syndrome.How is PIP measured in ventilator?
2. During volume ventilation, an increase in tidal volume corresponds to an increase in PIP during pressure ventilation. If tidal volume is not measured, initial PIP can be selected based on observation of chest wall movement and magnitude of breath sounds.
What does peep mean in respiratory?Positive end-expiratory pressure (PEEP) is the positive pressure that will remain in the airways at the end of the respiratory cycle (end of exhalation) that is greater than the atmospheric pressure in mechanically ventilated patients.[1]
Article first time published onWhat should you limit your peak inspiratory pressure PIP to?
Generally PIP values should not exceed 30 cm H2O. Values greater than 40 cm H2O may be harmful to the normal horse lung and should not be sustained.
What does high PEEP alarm mean on ventilator?
A high airway pressure alarm is signaling a problem with resistance or compliance. The first thing to do is turn up the upper limit on the alarm parameter to stop the alarm and ensure that the patient receives the set breath from the ventilator.
What are the primary determinants of peak inspiratory pressure PIP for a ventilated patient?
This barotrauma was caused by the high peak inspiratory pressures (PIP) required to oxygenate stiff lungs. The primary determinants of mean airway pressure (and thus oxygenation) on a conventional ventilator are the inspiratory time (IT), PIP, positive end expiratory pressure and gas flow rates.
What are normal ventilator settings?
Ventilator settings Sensitivity adjusts the level of negative pressure required to trigger the ventilator. A typical setting is –2 cm H2O. Too high a setting (eg, more negative than –2 cm H2O) causes weak patients to be unable to trigger a breath.
What is inspiratory time on ventilator?
In short, the inspiratory rise time determines the rate at which the ventilator achieves a target pressure (in pressure control and pressure support modes) or flow rate (in volume control modes). It is set in percent of the breath cycle (from 0% to 20% of the breath cycle time) or in seconds (0-0.4 seconds).
What causes low peak pressure on ventilator?
Some causes for low pressure alarms are: Inadequate inflation of the tracheostomy tube cuff. Poorly fitting noninvasive masks or nasal pillows/prongs. Loose circuit and tubing connections. The patient demands higher levels of air than the ventilator is putting out.
How is pip calculated?
The value of a pip can be calculated by dividing 1/10,000 or 0.0001 by the exchange rate. For example, a trader who wants to buy the USD/CAD pair would be purchasing US dollars and simultaneously selling Canadian dollars.
What is inspiratory hold?
The inspiratory hold manoeuvre abolishes the pressure contribution from the airway resistance and reveals the pressure in the alveoli.
What does high pressure mean on a ventilator?
High pressure alarm: This will sound when the pressure in the circuit has increased. It helps protect the lungs from high pressures delivered from the ventilator. Secretions, water in the tubing, or kinks in the tubing can cause high pressure.
What is the highest PEEP level?
Under controlled conditions, higher levels of PEEP are well tolerated. PEEP of 29 appears to be the highest tolerated PEEP in our patient. We noted an initial rise in blood flow across all cardiac valves followed by a gradual decline.
How do you do inspiratory hold on a ventilator?
- Ensure the Paw waveform is displayed.
- Open the Hold window.
- Wait until the Paw waveform plot restarts from the left side.
- Wait for the next inspiration.
- Then select INSP hold.
- When the flow reaches zero, deactivate the hold maneuver by selecting Insp hold again.
How long can a person stay on a ventilator?
How long does someone typically stay on a ventilator? Some people may need to be on a ventilator for a few hours, while others may require one, two, or three weeks. If a person needs to be on a ventilator for a longer period of time, a tracheostomy may be required.
What does a PEEP of 5 mean?
A higher level of applied PEEP (>5 cmH2O) is sometimes used to improve hypoxemia or reduce ventilator-associated lung injury in patients with acute lung injury, acute respiratory distress syndrome, or other types of hypoxemic respiratory failure.
Is a PEEP of 15 bad?
To determine optimum PEEP, Gaussian mixture model was applied to the adjusted means of cardiac output and oxygen delivery. Increasing PEEP to 10 and higher resulted in significant declines in cardiac output. A PEEP of 15 and higher resulted in significant declines in oxygen delivery.
What does MV low mean on a ventilator?
Answer. Low exhaled volume alarms are triggered by air leaks. These are most frequently secondary to ventilatory tubing disconnect from the patient’s tracheal tube but will also occur in the event of balloon deflation or tracheal tube dislodgement.
What is f total in ventilator?
Exhaled Minute Volume – amount of air exhaled in one minute. Peak Inspiratory Pressure – maximum amount of pressure reached during inspiration. RR/F – Total respiratory rate includes set rate and patient initiated breaths.
What is the lowest setting on a ventilator?
When using the ventilator a PS of 5 – 7 cmH2O and 1-5 cmH20 PEEP (so called ‘minimal ventilator settings’) will overcome increased work of breathing through the circuit (i.e. ETT) If still on the ventilator the patient should have ‘minimal ventilator settings” Initial trial should last 30 – 120 minutes.
How do you read ventilator numbers?
- The respiratory rate set by the user. …
- The tidal volume per breath. …
- Flow- How fast is the breath delivered by the ventilator.
- Waveform- This is a square waveform which means that the air is delivered at a constant pressure throughout inspiration.
What are the most appropriate initial settings to choose on the ventilator?
Initial settings for ventilation may be summarized as follows: Assist-control mode. Tidal volume set depending on lung status – Normal = 12 mL/kg ideal body weight; COPD = 10 mL/kg ideal body weight; ARDS = 6-8 mL/kg ideal body weight. Rate of 10-12 breaths per minute.