What factors affect contractility
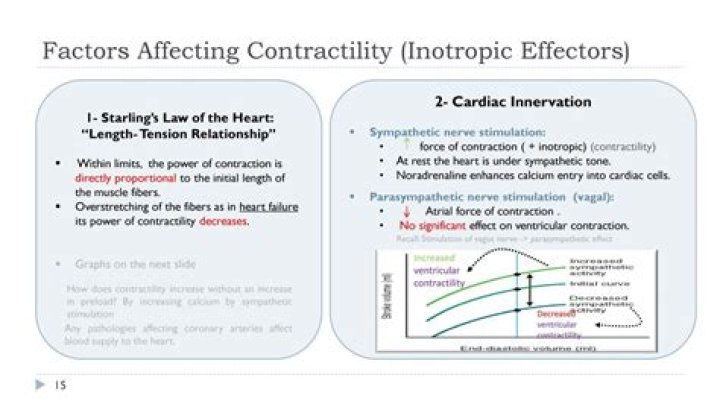
Calcium concentration. Catecholamines and the autonomic nervous system. ATP availability (eg. ischaemia) Extracellular calcium.Temperature.
What causes decreased contractility of the heart?
Reduced myocardial contractility can result from the following: RV infarction. Ischemia. Hypoxia.
What part of the heart regulates contractility?
The endocardium is composed of endothelial cells that provide a smooth, non-adherent surface for blood collection and pumping and may help regulate contractility.
What increases muscle contractility?
Short-term increases in demand on the heart (e.g., exercise) are met by increases in the force and frequency of contraction. These changes are mediated by increases in sympathetic nervous system activity, an increase in the frequency of contraction, and changes in muscle length.How does heart failure affect contractility?
More commonly, heart failure reflects an abnormality of LV contractile function, resulting in systolic dysfunction, and impaired emptying of the left ventricle, with a resultant fall in cardiac output.
How do inotropes increase contractility?
By increasing the concentration of intracellular calcium or increasing the sensitivity of receptor proteins to calcium, positive inotropic agents can increase myocardial contractility.
How does calcium affect contractility?
The calcium that enters the heart cell through the calcium ion channel activates the ryanodine receptor to release enough calcium from the sarcoplasmic reticulum to initiate heart muscle contraction. This is done by binding to another structure, named troponin, inside the heart muscle cell.
How does increased contractility affect cardiac output?
[8] Contractility describes the force of myocyte contraction, also referred to as inotropy. As the force of contraction increases, the heart is able to push more blood out of the heart, and thus increases the stroke volume.What affects preload afterload and contractility?
Contractility is the intrinsic strength of the cardiac muscle independent of preload, but a change in preload will affect the force of contraction. Afterload is the ‘load’ to which the heart must pump against. Afterload goes down when aortic pressure and systemic vascular resistance decreases through vasodilation.
What causes spasm?- Not enough stretching.
- Muscle fatigue.
- Exercising in the heat.
- Dehydration.
- Depletion of electrolytes (salts and minerals like potassium, magnesium and calcium in your body).
- Involuntary nerve discharges.
- Restriction in the blood supply.
- Stress.
What triggers movement of the muscles?
1. A Muscle Contraction Is Triggered When an Action Potential Travels Along the Nerves to the Muscles. Muscle contraction begins when the nervous system generates a signal. The signal, an impulse called an action potential, travels through a type of nerve cell called a motor neuron.
How does force develop during contraction?
Isotonic contractions generate force by changing the length of the muscle and can be concentric contractions or eccentric contractions. A concentric contraction causes muscles to shorten, thereby generating force. Eccentric contractions cause muscles to elongate in response to a greater opposing force.
What makes up the myocardium?
The myocardium is the muscular layer of the heart. It consists of cardiac muscle cells (cardiac myocytes [also known as cardiac rhabdomyocytes] or cardiomyocytes) arranged in overlapping spiral patterns.
What muscle causes contractions of the heart?
Cardiac muscle differs from skeletal muscle in that it exhibits rhythmic contractions and is not under voluntary control. The rhythmic contraction of cardiac muscle is regulated by the sinoatrial node of the heart, which serves as the heart’s pacemaker.
What causes the SA node to fire?
The autonomic nervous system, the same part of the nervous system as controls the blood pressure, controls the firing of the SA node to trigger the start of the cardiac cycle.
What impaired contractility?
Systolic dysfunction, often termed ventricular failure, refers to an impairment in ventricular contractility which results in a reduced stroke volume and hence inadequate cardiac output.
How does contractility affect ventricular function?
Changes in myocardial contractility alter the position of both the filling pressure-stroke volume relationship and the aortic systolic pressure-stroke volume relationship with an increase in contractility shifting these relations up to a new relationship with a greater stroke volume at any given pressure.
Does increased contractility cause CHF?
Enhanced contractility associated with SERCA2 overexpression was also reported to benefit heart failure and secondary remodeling and/or hypertrophy. For example, overexpression of SERCA2 by transgenesis was protective against diabetic cardiomyopathy as well as cardiac dysfunction induced by chronic pressure overload.
How does cAMP increase contractility?
These catecholamines bind primarily to beta1-adrenoceptors in the heart that are coupled to Gs-proteins. … Increased cAMP, through its coupling with other intracellular messengers, increases contractility (inotropy), heart rate (chronotropy) and conduction velocity (dromotropy).
How does acidosis decrease heart contractility?
The reduction of contractility associated with an acidosis is determined by the fall of pH in the intracellular fluid. The function of many organelles within the cardiac cell is affected by hydrogen ions. The tension generated by isolated myofibrils at a fixed calcium concentration is reduced at low pH.
What drugs increase cardiac contractility?
Inotropic agents such as milrinone, digoxin, dopamine, and dobutamine are used to increase the force of cardiac contractions.
What affects preload of the heart?
Factors affecting preload Preload is affected by venous blood pressure and the rate of venous return. These are affected by venous tone and volume of circulating blood. Preload is related to the ventricular end-diastolic volume; a higher end-diastolic volume implies a higher preload.
Do beta blockers decrease contractility?
By reducing heart rate, contractility, and arterial pressure, beta-blockers reduce the work of the heart and the oxygen demand of the heart.
Does contractility depend on afterload?
Contractility represents the ability of the myocardial muscle to shorten or thicken against a load. Although ejection fraction (EF) is the most common clinical assessment of contractility in practice, it is highly dependent on ventricular afterload.
What factors affect afterload?
Factors which affect afterload: valve resistance, vascular resistance, vascular impedance, blood viscosity, intrathoracic pressure, and the relationship of ventricular radius and volume. Determinants which are specific to the right and left ventricles.
What affects end-systolic volume?
End-systolic volume depends on two factors: contractility and afterload. Contractility describes the forcefulness of the heart’s contraction. Increasing contractility reduces end-systolic volume, which results in a greater stroke volume and thus greater cardiac output.
What factors affect cardiac output quizlet?
- lower blood volume.
- Sympathetic nerves regulate peripheral venous tone.
- Venous muscle pump.
- Increased cardiac output reduces filling pressure.
- Respiration’s effect on extramural cardiac pressure.
- Increased extramural pressure impairs filling.
Does contractility affect blood pressure?
Conclusions. In the present study, we demonstrated by means of a mathematical model of the cardiovascular system that a physiological increase in cardiac contractility leads to a steeper forward pressure wave pumped by the LV, which, subsequently, drastically alters central and peripheral pressure and flow waves.
Does Arteriole constriction increase or decrease afterload?
In heart failure, particularly when cardiac output is significantly reduced, arterial vasoconstriction helps to maintain arterial pressure. The increased systemic vascular resistance, however, contributes to an increase in afterload on the heart, which can further depress systolic function.
What causes muscle spasms in the chest?
High blood pressure and high cholesterol are the most common causes of these spasms. Approximately 2 percent of people with angina, or chest pain and pressure, experience coronary artery spasms. Coronary artery spasms can also occur in people who have atherosclerosis.
Can anxiety cause muscle spasms?
Anxiety can also cause muscle spasms. The most common reasons for spasms include: Muscle Tension Anxiety causes a considerable amount of muscle tension, and muscle tension can lead to both cramping and spasms. Muscle tension is a lot like exercise – it tires out the muscles and causes them to spasm as a result.