What is Ranson scoring system
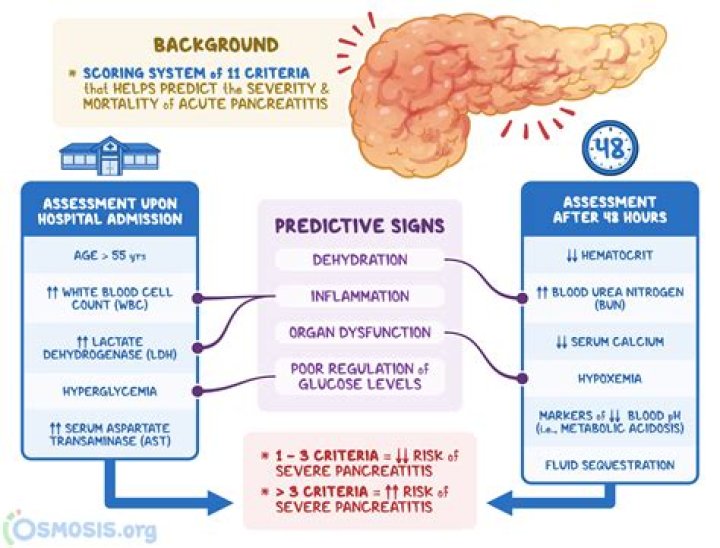
Ranson’s criteria is a scoring system that helps healthcare professionals predict the severity and mortality of acute pancreatitis, an inflammatory condition of the pancreas that occurs primarily as a result of alcohol or gallstones.
What does a Ranson score of 3 to 4 indicate in a patient with pancreatitis?
Acute Pancreatitis A Ranson score > 3 or an APACHE II score > 8 indicates severe pancreatitis. Limitations of Ranson’s criteria include a 48‐hour time requirement for score determination, and a lack of ability to reassess severity at later points during the hospitalization.
How do you calculate fluid sequestration in acute pancreatitis?
Level of fluid sequestration in the first 48 hours after hospital admission was calculated by subtracting the total amount of fluid administered and lost in the first 48 hours of hospitalization.
How do you know the severity of pancreatitis?
The revised clinical criteria for the diagnosis of AP are (1) acute pain and tenderness in the upper abdomen; (2) elevated pancreatic enzyme levels in in blood and/or urine; and (3) ultrasound (US), CT or magnetic resonance imaging (MRI) abnormalities of the pancreas characteristic of AP[1].What is fluid sequestration?
Fluid sequestration (FS) is one of the components of Ranson score [6] and is considered as another simple prognostic parameter. FS was defined as the difference between the amount of fluids administered and the losses from urine and nasogastric tube [7].
How does pancreatitis cause third spacing?
This is caused by release of cytokines and other pro inflammatory mediators. These further cause vasodilatation, intravascular volume depletion, and end organ hypoperfusion. Patients of acute pancreatitis have significant fluid loss in third space. This is evident by increased hematocrit.
Why is LDH elevated in pancreatitis?
In patients with biliary pancreatitis (BP), however, liver enzymes are generally elevated early in the course of the disease because of acute inflammatory liver cell injury caused by ampullary stones impacted during their transpapillary passage.
When caring for a patient with acute pancreatitis which laboratory finding is the best indicator of the disorder?
Serum amylase and lipase levels are typically elevated in persons with acute pancreatitis. However, these elevations may only indicate pancreastasis. In research studies, amylase or lipase levels at least 3 times above the reference range are generally considered diagnostic of acute pancreatitis.What are Pseudocysts?
Pancreatic pseudocysts are collections of leaked pancreatic fluids. They may form next to the pancreas during pancreatitis. Having gallstones and drinking a lot of alcohol are the two most common causes of pancreatitis. Most people with pseudocysts will have stomach pain, vomiting, and other symptoms of pancreatitis.
What is Ranson Criteria for pancreatitis?The modified Ranson criteria are used to assess gallstone pancreatitis. The five parameters on admission are age older than 70 years, WBC greater than 18,000 cells/cmm, blood glucose greater than 220 mg/dL (greater than 12.2 mmol/L), serum AST greater than 250 IU/L, and serum LDH greater than 400 IU/L.
Article first time published onWhat tests confirm pancreatitis?
- Blood tests. …
- Stool tests. …
- Ultrasound. …
- Computed tomography (CT) scan. …
- Magnetic resonance cholangiopancreatography (MRCP). …
- Endoscopic ultrasound (EUS link). …
- Pancreatic Function Test (PFT).
What are the markers for pancreatitis?
Serum amylase remains the most commonly used biochemical marker for the diagnosis of acute pancreatitis, but its sensitivity can be reduced by late presentation, hypertriglyceridaemia, and chronic alcoholism.
What is third space loss?
Third-space losses refer to fluid losses into spaces that are not visible, such as the bowel lumen (in bowel obstruction) or the retroperitoneum (as in pancreatitis).
How do fluids help pancreatitis?
Patients with acute pancreatitis lose a large amount of fluids to third spacing into the retroperitoneum and intra-abdominal areas. Accordingly, they require prompt intravenous (IV) hydration within the first 24 hours. Especially in the early phase of the illness, aggressive fluid resuscitation is critically important.
How do IV fluids help pancreatitis?
Early fluid resuscitation could thus help to restore local pancreatic perfusion, counteract systemic hypotension and thus prevent secondary organ failure due to fluid sequestration.
Is edema considered third spacing?
Third-spacing occurs when too much fluid moves from the intravascular space (blood vessels) into the interstitial or “third” space-the nonfunctional area between cells. This can cause potentially serious problems such as edema, reduced cardiac output, and hypotension.
What is volume depletion?
Volume depletion denotes reduction of effective circulating volume in the intravascular space, whereas dehydration denotes loss of free water in greater proportion than the loss of sodium.
How do we replace this lost fluid?
- 1 Drink frequently (2-4 times an hour, 200-250ml each time)
- 2 Keep your drink slightly cool (5-15℃)
- 3Sodium concentration (40-80 mg / 100 ml) Salt concentration 0.1-0.2%
- 4Sugar concentration (around 4-8%) Should contain glucose + fructose (or sugar)
Does LDH blood test require fasting?
You don’t need any special preparations for an LDH blood test.
How is biliary pancreatitis diagnosed?
Gallstone pancreatitis is diagnosed by using a combination of tools. The most common are blood tests and different types of body scans. Blood tests can identify inflammation in the pancreas. CT scan, MRI, or ultrasound can give a clearer picture of the severity of your pancreatitis.
Does pancreatitis affect liver enzymes?
Elevated liver enzymes in the setting of acute pancreatitis point toward choledocholithiasis as the cause, with an alanine aminotransferase greater than three times the upper limit of normal having a positive predictive value of 95% for gallstone pancreatitis in the nonalcoholic patient.
Why does pancreatitis cause sirs?
Additionally, pancreatic proteases released into the bloodstream can activate NPM and macro- phages distant from the pancreas, releasing further inflammatory mediators causing the sys- temic inflammatory response syndrome (SIRS) and organ damage.
What levels are elevated with pancreatitis?
Amylase levelsLipase levelsNormal23-85 U/L (some lab results go up to 140 U/L)0-160 U/LPancreatitis suspected> 200 U/L> 200 U/L
What is the relationship between the liver and the pancreas?
The pancreas and bile duct (biliary) systems together form an important part of the digestive system. The pancreas and liver produce juices (pancreatic juice and bile) which help in the process of digestion (i.e. the breakdown of foods into parts which can be absorbed easily and used by the body).
How do you drain a pancreas?
A radiologist will drain it by inserting a needle guided by computed tomography. A gastroenterologist may drain the pseudocyst through the stomach by creating a small opening between the pseudocyst and the stomach, or by placing a stent into the pancreas during endoscopy.
What does Hypodensity in pancreas mean?
Hypodense infiltrating mass of the head of the pancreas with posterior celiac infiltration. Chronic pancreatitis macrocalcifications of the head are absent within tumour infiltration. Pancreatic adenocarcinoma is a tumour with a hypoxic, hypovascular fibrous component, as is the fibrosis of chronic pancreatitis.
What does my pancreas do?
The pancreas produces digestive juices and insulin, as well as other hormones to do with digestion. The part which produces the digestive juices is called the exocrine pancreas. The part which produces hormones, including insulin, is called the endocrine pancreas.
What laboratory finding is primary diagnostic indicator for pancreatitis?
Serum amylase and lipase levels are still used to confirm the diagnosis of acute pancreatitis. Although not routinely available, the serum trypsin level is the most accurate laboratory indicator for pancreatitis.
Which laboratory test would the nurse anticipate to diagnose pancreatitis?
The key laboratory results for diagnosis of pancreatitis are elevated amylase and lipase levels.
What laboratory finding is the primary diagnostic indicator for acute pancreatitis quizlet?
Although serum amylase was the primary diagnostic marker, serum lipase is now the preferred test.
How do you assess the pancreas?
A procedure called endoscopic retrograde cholangiopancreatography (ERCP) uses a long tube with a camera on the end to examine your pancreas and bile ducts. The tube is passed down your throat, and the camera sends pictures of your digestive system to a monitor.