What is the purpose of octreotide
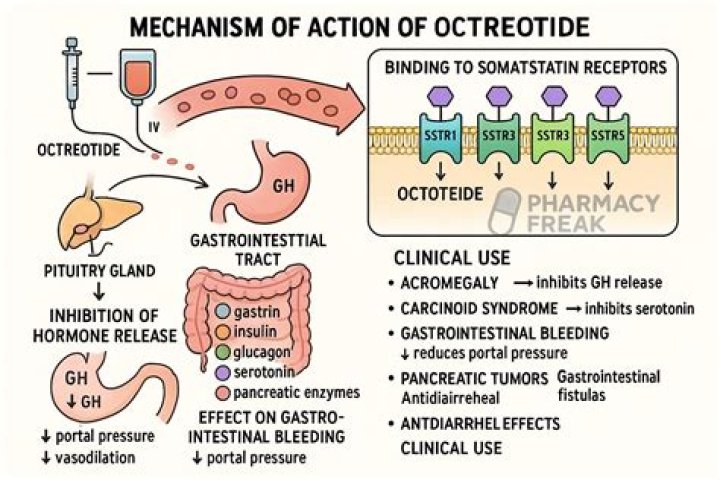
Octreotide immediate-release injection is used to decrease the amount of growth hormone (a natural substance) produced by people with acromegaly (condition in which the body produces too much growth hormone, causing enlargement of the hands, feet, and facial features; joint pain; and other symptoms) who cannot be …
What is octreotide used for liver?
Octreotide is often given as an infusion for management of acute hemorrhage from esophageal varices in liver cirrhosis on the basis that it reduces portal venous pressure, though current evidence suggests that this effect is transient and does not improve survival.
When should I start taking octreotide?
Variceal bleeding occurs as a result of liver cirrhosis, so it is reasonable to start octreotide in patients who are known to or who may have cirrhosis. This would include patients with known or suspected alcoholic liver disease or patients with jaundice, ascites, or hepatic encephalopathy.
What is octreotide used for in palliative care?
A synthetic analogue of somatostatin used in palliative care to relieve symptoms associated with unresectable hormone-secreting tumours (for example carcinoid), intractable diarrhoea related to high output ileostomies or inoperable bowel obstruction in patients with cancer.What is the injection given for vomiting?
Zofran (ondansetron hydrochloridc) Injection is an antiemetic (anti nausea and vomiting) used to prevent nausea and vomiting that may be caused by surgery or by medicine to treat cancer (chemotherapy).
What is hepatorenal failure?
Hepatorenal syndrome (HRS) is a type of progressive kidney failure seen in people with severe liver damage, most often caused by cirrhosis. As the kidneys stop functioning, toxins begin to build up in the body. Eventually, this leads to liver failure.
Is Normix an antibiotic?
A07AA11 – rifaximin ; Belongs to the class of antibiotics. Used in the treatment of intestinal infections.
Does octreotide increase blood pressure?
Octreotide treatment is associated with an increase of 24-h and nighttime blood pressure, and with loss of circadian blood pressure rhythm. Splanchnic vasoconstriction by this drug, shifting blood to peripheral vessels, may explain this phenomenon.How is portal hypertension treated?
Medications such as propranolol and isosorbide may be prescribed to lower the pressure in the portal vein and reduce the risk of recurrent bleeding. The drug lactulose can help treat confusion and other mental changes associated with encephalopathy.
How does octreotide work in bowel obstruction?Among the antisecretory drugs, octreotide has been shown to reduce nausea and vomiting in bowel-obstructed patients owing to a reduction of gastrointestinal secretions, thus allowing in most patients removal of the nasogastric tube and the associated distress.
Article first time published onWhat do you mix octreotide in?
Octreotide is administered as a continuous subcutaneous infusion (CSCI) using sodium chloride 0.9% as the diluent.
How do you give octreotide infusion?
In emergency situations, octreotide may be administered undiluted by intermittent direct IV injection. Give IV slowly over 3 minutes. Dilute in 50 mL to 200 mL of 0.9% Sodium Chloride or 5% Dextrose injection; infuse IV over 15 to 30 minutes. Once diluted, the infusion solution is stable for 24 hours.
What is the function of somatostatin?
Somatostatin is a hormone produced by many tissues in the body, principally in the nervous and digestive systems. It regulates a wide variety of physiological functions and inhibits the secretion of other hormones, the activity of the gastrointestinal tract and the rapid reproduction of normal and tumour cells.
Why is Cabergoline prescribed?
Cabergoline is used to treat hyperprolactinemia (high levels of prolactin, a natural substance that helps breast-feeding women produce milk but can cause symptoms such as infertility, sexual problems, and bone loss in women who are not breast-feeding or men).
What are subcutaneous injections?
A subcutaneous injection is a way to give certain medications using a needle. The subcutaneous tissue, also known as the hypodermis, is the innermost (deepest) layer of skin. It is made up of fat and connective tissue and helps the body control temperature.
What is the best medicine to stop vomiting?
Over-the-counter (OTC) medications to stop vomiting (antiemetics) such as Pepto-Bismol and Kaopectate contain bismuth subsalicylate. They may help protect the stomach lining and reduce vomiting caused by food poisoning.
What relieves nausea fast?
- Drink clear or ice-cold drinks.
- Eat light, bland foods (such as saltine crackers or plain bread).
- Avoid fried, greasy, or sweet foods.
- Eat slowly and eat smaller, more frequent meals.
- Do not mix hot and cold foods.
- Drink beverages slowly.
What is the best medicine for nausea and vomiting?
- Bismuth subsalicylate, the active ingredient in OTC medications like Kaopectate® and Pepto-Bismol™, protects your stomach lining. Bismuth subsalicylate is also used to treat ulcers, upset stomach and diarrhea.
- Other medicines include cyclizine, dimenhydrinate, diphenhydramine, and meclizine.
When should I take Normix?
To treat irritable bowel syndrome with diarrhea, take this medication by mouth with or without food as directed by your doctor, usually 3 times a day for 14 days. To prevent hepatic encephalopathy, take this medication by mouth with or without food as directed by your doctor, usually 2 times a day (every 12 hours).
What is nexium used for?
Esomeprazole is used to treat certain stomach and esophagus problems (such as acid reflux, ulcers). It works by decreasing the amount of acid your stomach makes. It relieves symptoms such as heartburn, difficulty swallowing, and persistent cough.
Does rifaximin treat UTI?
Rifaximin is different from other antibiotics one might take for a urinary tract infection or a sinus infection, Pimentel said. He said it less likely to create antibiotic resistance because 99 percent of it passes out of the body in the feces, rather than being absorbed into other areas of the body outside the gut.
Can you survive hepatorenal syndrome?
Hepatorenal syndrome is classified into 2 types: type-1 HRS shows a rapid and progressive decline in renal function with a very poor prognosis (median survival of about 2 weeks); type-2 HRS has a more stable kidney failure, with a median survival of 6 months; its main clinical manifestation is refractory ascites.
What are the symptoms of hepatorenal syndrome?
- Abdominal swelling due to fluid (called ascites, a symptom of liver disease)
- Mental confusion.
- Muscle jerks.
- Dark-colored urine (a symptom of liver disease)
- Decreased urine output.
- Nausea and vomiting.
- Weight gain.
- Yellow skin (jaundice, a symptom of liver disease)
What are the signs of dying from cirrhosis of the liver?
- Loss of appetite.
- Weakness.
- Fatigue.
- Nausea/Vomiting.
- Abdominal pain/bloating.
- Itching.
Is portal hypertension serious?
Portal hypertension is a dangerous condition with severe, life-threatening complications. Call your healthcare provider right away if you notice any of these symptoms: Yellowing of the skin. Abnormally swollen belly.
What stage of liver disease is portal hypertension?
Portal hypertension is defined as the pathological increase of portal venous pressure, mainly due to chronic end-stage liver disease, leading to augmented hepatic vascular resistance and congestion of the blood in the portal venous system.
What happens if portal vein is blocked?
Portal vein thrombosis is blockage or narrowing of the portal vein (the blood vessel that brings blood to the liver from the intestines) by a blood clot. Most people have no symptoms, but in some people, fluid accumulates in the abdomen, the spleen enlarges, and/or severe bleeding occurs in the esophagus.
Does somatostatin increase blood pressure?
During somatostatin infusion, the mean blood pressure (MBP) remained unaffected in all patients with EH and the normotensive subjects, while the PRA decreased slightly in the EH group.
Why is octreotide used in GI bleed?
Octreotide reduces portal and variceal pressures as well as splanchnic and portal-systemic collateral blood flows [2]. It also prevents postprandial splanchnic hyperemia in patients with portal hypertension [3] and lowers gastric mucosal blood flow in normal and portal hypertensive stomachs [4].
When do you use octreotide in GI bleed?
Octreotide is not recommended for routine use in patients with acute nonvariceal upper GI bleeding, but it can be used as adjunctive therapy in some cases. Its role is generally limited to settings in which endoscopy is unavailable or as a means to help stabilize patients before definitive therapy can be performed.
What is malignant bowel obstruction?
Malignant bowel obstruction (MBO) is a frequent complication in patients with advanced cancer, especially of digestive or gynecological origin. Bowel obstruction is any mechanical or functional obstruction of the intestine that prevents physiological transit and digestion.



