What is Undersensing and Oversensing of a pacemaker
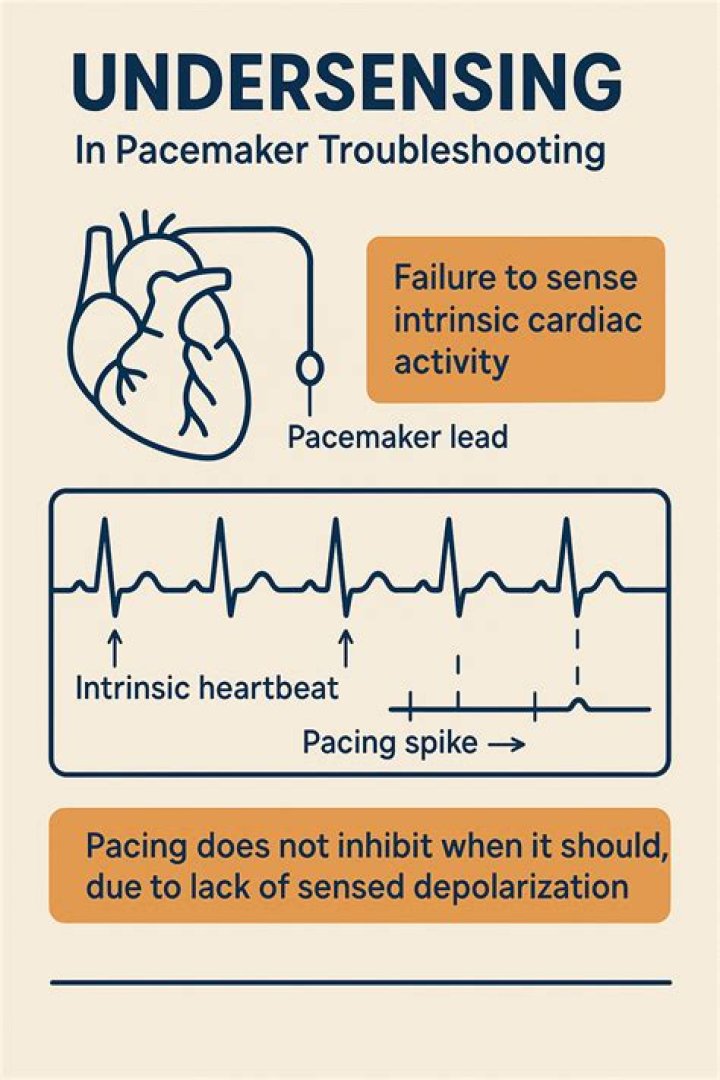
Oversensing, which means that the pacemaker senses signals that are not true P-waves or R-waves. Sensing of such signals normally inhibits the pacemaker. Oversensing may lead to underpacing. Failure to sense (undersensing), which means that it fails to sense true P-waves or R-waves. Undersensing may lead to overpacing.
What is pacemaker Oversensing?
Oversensing. Oversensing occurs when the pacemaker senses electrical signals that it should not normally encounter, which results in inappropriate inhibition of the pacing stimulus.
How do you fix a pacemaker Oversensing?
Oversensing is one condition that is diagnosable and treatable with magnet application. As mentioned before, magnet application will convert the pacemaker to asynchronous mode, and it will then operate at the preset rate.
What does Undersensing mean?
Undersensing occurs when the pacemaker does not sense intrinsic cardiac activity that is present and delivers a pace pulse when it shouldn’t. … Oversensing is inappropriate inhibition of a demand pacemaker due to detection of signals other than R-waves, such as muscle artifact or T-waves.How do you know if your pacemaker is Undersensing?
Problems with Sensing Results in asynchronous pacing. Causes include increased stimulation threshold at electrode site (exit block), poor lead contact, new bundle branch block or programming problems. ECG findings may be minimal, although presence of pacing spikes within QRS complexes is suggestive of undersensing.
What is T wave Oversensing?
T-wave oversensing is associated with a typical aspect of alternating high-frequency (R-wave) and low-frequency (T-wave) signals on the near-field electrogram. The device counts the T-wave as an additional ventricular event doubling the measured ventricular rate.
What is functional Undersensing?
Functional undersensing occurs when the pacemaker does not sense intrinsic activity during the period when sensing is disabled. This is an appropriate form of undersensing, and was discussed previously (refer to PVARP). Undersensing can lead to overpacing, because the pacemaker does not sense ongoing activity.
What causes 3rd degree heart block?
Third-degree heart block may be caused by: Damage to the heart from surgery. Damage to the heart muscle from a heart attack. Other types of heart disease that result in heart muscle damage.What is VVI mode pacemaker?
A pacemaker in VVI mode denotes that it paces and senses the ventricle and is inhibited by a sensed ventricular event. The DDD mode denotes that both chambers are capable of being sensed and paced.
What causes pacemaker lead dislodgement?First described in 1968, refers to permanent malfunction of a pacemaker due to the patient’s manipulation of the pulse generator. The patient, inadvertently or deliberately, turns and rotates the generator on its long axis and, because of traction, causes the lead displacement.
Article first time published onWhat are the most common problems with a pacemaker?
- Infection near the site in the heart where the device is implanted.
- Swelling, bruising or bleeding at the pacemaker site, especially if you take blood thinners.
- Blood clots (thromboembolism) near the pacemaker site.
- Damage to blood vessels or nerves near the pacemaker.
- Collapsed lung (pneumothorax)
What is the normal pacemaker of the heart what happens when this pacemaker fails?
The sinoatrial node is called the heart’s pacemaker. When something goes wrong with the sinoatrial node, you may develop a consistently slow heartbeat (sinus bradycardia) or the normal pacemaker activity may stop entirely (sinus arrest).
What causes pacemaker to malfunction?
Causes of pacemaker failure include lead related failure, unit malfunction, problems at the insertion site, failures related to exposure to high voltage electricity or high intensity microwaves, and a miscellaneous category (one patient had ventricular tachycardia when using his electric razor and another patient had …
What is atrial pacing?
In AOO mode, the atrium is paced at a set rate regardless of atrial activity; this is asynchronous atrial pacing. In AAI mode, the atrium is sensed and the pacemaker is inhibited if the native atrial rate rises above the pacemaker set rate; this is demand atrial pacing.
Do pacemakers prevent tachycardia?
In some cases, pacemakers have a program to lengthen the PVARP after PMT detection to potentially stop the tachycardia. Alternatively, prevention of one ventricular paced beat can also stop the tachycardia. Some pacemakers use this algorithm.
Can you do an EKG on someone with a pacemaker?
Monitoring a Pacemaker Patient The recommended lead placement for a pacemaker patient is as follows. A Pacemaker patient usually requires a different electrode patch placement configuration than a non-pacemaker patient. Do not place an ECG electrode directly over the pacemaker generator.
Does Idioventricular rhythm have a pulse?
An idioventricular rhythm — not accelerated — has a heart rate of < 60 beats per minute. AIVR is hemodynamically stable, and thus no specific treatment is needed.
When is a VVI pacemaker used?
VVI/VVIR pacing is indicated for patients with chronic atrial arrhythmias that are not expected to return to sinus rhythm. While VVI/VVIR protects patients from lethal bradyarrhythmias, it does not maintain AV synchrony, which sometimes leads to “Pacemaker syndrome.”
When is DDI mode used?
The ideal indication for this type of mode is a patient with AV block and atrial disease associating passage in fast AF (no risk of runaway) and permanent sinus dysfunction after reduction (AP-VP pacing).
Is Dddr pacemaker an ICD?
DDDR = dual chamber rate adaptive pacemaker; EPS = electrophysiology study; ICD = implantable cardiovertor defibrillator; LVEF = left ventricular ejection fraction; VF = ventricular fibrillation; VT = ventricular tachycardia; VVI = single chamber ventricular pacemaker.
What is 2nd and 3rd degree heart block?
A narrow QRS complex suggests nodal arrhythmia and likely type I block, while a wide complex indicates an infranodal location and type II block. Third degree AV block occurs when P waves are not conducted to the ventricles and an ectopic, slow escape rhythm is present.
What is the difference between Type 1 and Type 2 Second-degree heart block?
The hallmark of Mobitz type 1 block is the gradual prolongation of PR intervals before a block occurs. Mobitz type 2 block has constant PR intervals before blocks occur. Thus, if one can spot the gradual prolongation of PR intervals, Mobitz type 1 block should be diagnosed.
What is pacemaker lead?
A lead is a special wire that delivers energy from a pacemaker or implantable cardioverter defibrillator (ICD) to the heart muscle.
How are pacemaker leads attached to heart?
The lead (or leads) is an insulated wire that is connected to the pulse generator on one end, with the other end placed inside one of the heart’s chambers. The lead is almost always placed so that it runs through a large vein in the chest leading directly to the heart.
What causes pacemaker noise?
The appearance of noise on electrograms (EGMs) recorded from the lead of an implantable cardioverter-defibrillator (ICD) may be owing to oversensing of myopotentials, insulation breach, conductor coil fracture, loose set screw, or electromagnetic interference (EMI) from an external source.
How do you sleep with a pacemaker?
Sleep on your side. If you have an implanted defibrillator, sleep on the opposite side. Most defibrillators are implanted on the left side, so sleeping on the right side may feel more comfortable.
Is a pacemaker serious?
Safety. Having a pacemaker implanted is usually a very safe procedure with a low risk of complications. The biggest concern is the pacemaker losing its ability to control the heartbeat, either because it malfunctions or the wire moves out of the correct position.
What is the normal heart rate for a person with a pacemaker?
The pacemaker is individually programmed to maintain the patient’s natural, intrinsic ventricular rate which usually falls between 50 and 70 beats per minute.
Why am I short of breath with a pacemaker?
This can occur without any chest pain, presenting with sudden shortness of breath. His normally functioning pacemaker might be causing his heart to beat out of sync, which can result in what is called pacing-induced cardiomyopathy. The stress of his recent surgery caused the problem.
What happens when a pacemaker battery gets low?
“If the battery is completely drained, the device will no longer deliver pacing therapy. The patients who rely heavily on pacing or who are pacemaker dependent may be most at risk for having an adverse outcome.”
Can you have congestive heart failure with a pacemaker?
A large study found that 19 out of 100 people who were treated with a pacemaker for heart failure had to go into the hospital during the study because of heart failure. But 27 out of 100 people treated with medicine alone had to go into the hospital for heart failure.



