What makes a difficult airway
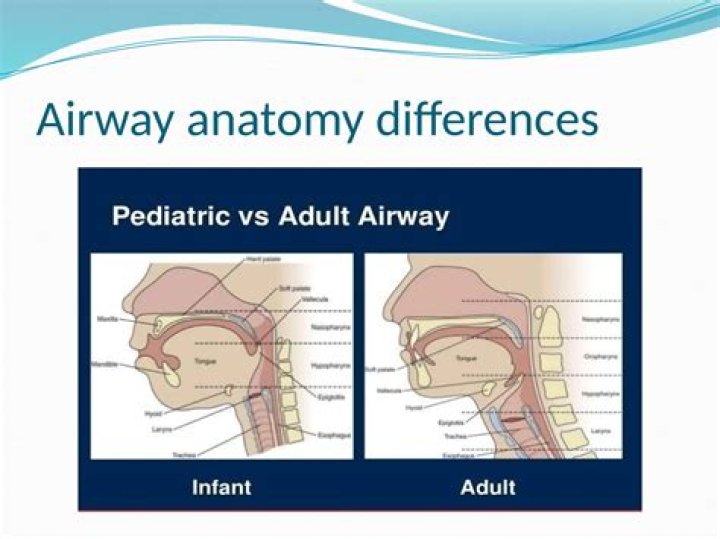
The American Society of Anesthesiologists defines a difficult airway as existing when “a conventionally trained anesthesiologist experiences difficulty with facemask ventilation of the upper airway, difficulty with tracheal intubation, or both.”[1] Canadian guidelines are broader, defining it as where “an experienced …
How common is a difficult airway?
The difficult airway is a challenge to emergency physicians. In the anaesthesia literature, is frequency ranges from 0.4 to 8.5% [1–3] of elective intubations. In the emergency medicine literature, is more common—from 2 to 14.8% [4–9]—but it includes prehospital intubation and may be performed by paramedics or doctors.
How do you prepare for a hard airway?
- Change equipment (eg. get a different blade)
- Change operator (get a more experienced person)
- Change patient position (eg. elevate the head/shoulders)
- Change modality (eg. try videolaryngoscopy)
How can you tell if you have a hard airway?
In the presence of pre-existing airway pathology, symptoms suggestive of impending airway obstruction should be identified. These include the presence of stridor, hoarseness, voice change, dysphagia and difficulty lying flat.What is difficult airway intubation?
A difficult airway is a clinical situation in which an anesthesiologist or other specially trained clinician has difficulty with mask ventilation or tracheal intubation. Difficult intubation can be defined as one requiring more than three attempts at laryngoscopy or more than 10 minutes of laryngoscopy.
How do you manage airway obstruction?
- The Heimlich maneuver. This is an emergency technique that may help a person who is choking on a foreign object: …
- Epinephrine. Epinephrine can be used to treat airway swelling due to an allergic reaction. …
- Cardiopulmonary resuscitation (CPR)
What is difficult laryngoscopy?
Difficult laryngoscopy is inability to view the glottis opening using a conventional curve blade laryngoscope, corresponding to a Cormack and Lehane III or IV grade view, in which only epiglottis or only pharynx and tongue, respectively, may be visualized, whereas difficult intubation is defined as usage of direct …
What are airway adjuvants?
Adjuvants to Upper Airway Obstruction They are measured and sized from the lip to the angle of the jaw and are useful for patients with spontaneous respirations who need help to keep their airway open (sleep apnea patients, for example).Can't oxygenate can't ventilate?
“Can’t Intubate Can’t Ventilate” is one of the frightening statements that causes massive surges of adrenaline in everyone. Unfortunately, most neural synapses don’t function well with that large surge of adrenaline, and it is, therefore, imperative to contemplate how to manage this scenario before it arises.
Which finding is most likely to predict a difficult airway?A likely indication of difficult intubation is present if the inter-incisor or hyoid-mental distance is less than three fingers or the hyoid-thyroid cartilage distance is less than two fingers. Depending on the patient population, reports of difficult intubation occur in 1.5% to 13% of patients.
Article first time published onWhat is the most common reason for unsuccessful intubation?
The most common reasons for an unsuccessful attempt were oesophageal intubation and failure to recognise the anatomy. In 36 (80%) of intubations, an intubatable view was achieved but was then either lost, not recognised or there was an apparent inability to correctly direct the endotracheal tube.
Are you awake when intubated?
Intubating a patient is a highly skilled procedure and involves inserting a tube through the patient’s mouth and into their airway: patients are usually sedated, allowing their mouth and airway to relax.
How do you intubate better?
- Practice. …
- Determine if intubation is indicated. …
- Prepare the patient. …
- Prepare your equipment. …
- Advance the laryngoscope blade. …
- BURP. …
- Bougie. …
- Abandon the attempt and reassess.
What is the tube they put down your throat called?
Sometimes, because of illness, injury, or surgery, you need help to breathe. Your doctor or anesthesiologist (a doctor who puts you to “sleep” for surgery) puts a tube (endotracheal tube, or ETT) down your throat and into your windpipe. This helps to get air into and out of your lungs. The process is called intubation.
For which of the following patients should a respiratory therapist anticipate having the most difficulty providing bag valve mask ventilation?
Patients over the age of 57 are more likely to have difficulties with bag mask ventilation. This may be because of decreased muscle tone in the upper respiratory tract, and subtle changes in the shape of the airway. Snoring may indicate structural abnormalities that make all forms of oxygenation more challenging.
What is the difficult airway assessment for laryngoscope?
Cervical radiographic assessment is a simple, economical, and non-invasive predictive method for difficult laryngoscopy. It should be used routinely along with other indices as pre-anesthetic airway assessment criteria to predict the difficult laryngoscopy.
Which risk factor is the most significant predictor of a difficult mask ventilation?
Six independent predictors for difficult mask ventilation were observed: body mass index of 30 kg/m2or greater, presence of a beard, Mallampati classification III or IV, age of 57 yr or older, severely limited mandibular protrusion, and a history of snoring.
Who does a laryngoscopy?
Laryngoscopy is when a doctor uses a special camera to look down the throat to see the voice box (larynx) and vocal cords. Ear, nose, and throat specialists (also called ENT doctors or otolaryngologists) do laryngoscopies.
What is the most common cause of airway obstruction in adults?
The tongue is the most common cause of upper airway obstruction, a situation seen most often in patients who are comatose or who have suffered cardiopulmonary arrest. Other common causes of upper airway obstruction include edema of the oropharynx and larynx, trauma, foreign body, and infection.
What illness causes an inflammation of the windpipe?
TracheitisOther namesInflammation of the tracheaAnatomy of the tracheaSpecialtyPulmonology
Which signs indicate that a person has severe airway obstruction?
A person who is choking (has complete airway obstruction): Can’t cry, talk, breathe, or cough. May grasp throat. May become severely anxious or agitated.
What happens if intubation fails?
When intubation has failed, face mask ventilation or LMA insertion may be difficult due to decreasing depth of anaesthesia and incomplete muscle relaxation. In this situation, the patient may not be sufficiently awake to spontaneously ventilate or deep/paralysed enough for ventilation to be effectively provided.
Can intubate Cannot ventilate?
The Difficult Airway Society has published guidelines for the management of such situations [1]. Situations arise, however, where although it is relatively straightforward to intubate, the patient’s lungs cannot be ventilated because of airway obstruction below the endo-tracheal tube.
Can intubate can't ventilate?
The ‘can intubate – can’t ventilate’ scenario is an acute anaesthetic emergency with the possibility of morbidity or even mortality [1]. We would like to describe another case of this, which occurred at Caesarean section for a 24-year-old primigravida.
How do I keep my airway open?
- Back slaps and abdominal thrusts are performed to relieve airway obstruction by foreign objects.
- Inward and upward force during abdominal thrusts.
- The head-tilt/chin-lift is the most reliable method of opening the airway.
Who can do intubation?
Who performs intubation? Doctors who perform intubation include anesthesiologists, critical care doctors, and emergency medicine doctors. An anesthesiologist specializes in relieving pain and providing total medical care for patients before, during and after surgery.
What 2 methods can be used to open the airway?
The two primary methods used by OEC Technicians to align and open a pa- tient’s airway are the head tilt-chin lift and the jaw-thrust maneuvers. Head Tilt-Chin Lift The head tilt-chin lift method is the primary technique OEC Technicians use to open a patient’s airway.
Which Mallampati score would predict a very difficult intubation?
A high Mallampati score (class 3 or 4) is associated with more difficult intubation as well as a higher incidence of sleep apnea.
How do you examine Airways?
Calder has suggested the following for routine preoperative airway assessment: a thorough history and review of previous notes, mouth opening followed by examination of the teeth and assessment of inter-dental (incisor) distance. A measurement of less than 37mm lies outside the normal range.
Can intubation go wrong?
When intubation error occurs, there can be several consequences for a patient. Brain, esophagus, nerve, vocal cord and lung damage may occur. After intubation, especially if the procedure is done improperly, a patient might suffer serious infections, bleeding, physical trauma or a collapsed lung.
What is an anterior larynx?
The larynx is located within the anterior aspect of the neck, anterior to the inferior portion of the pharynx and superior to the trachea. … The hyoid bone, while technically not part of the larynx, provides muscular attachments from above that aid in laryngeal motion.