When to use 59 or 51 modifier
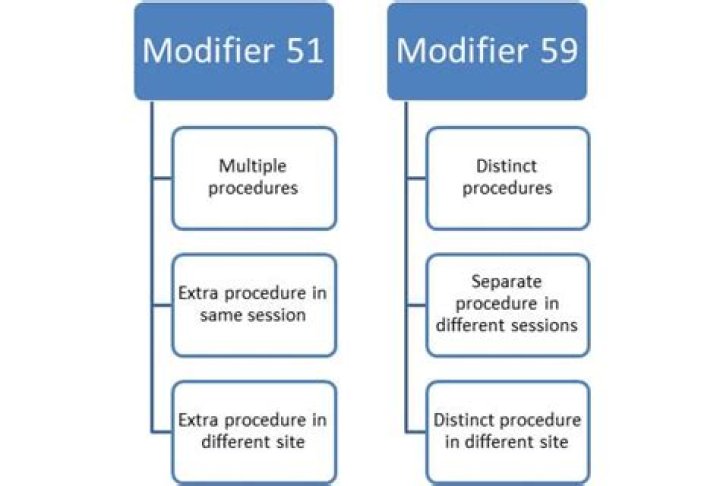
Modifier 51 impacts payment. … Modifier 51 impacts the payment amount, and modifier 59 affects whether the service will be paid at all. Modifier 59 is typically used to override National Correct Coding Initiative (NCCI) Edits.
Which code does the 51 modifier go on?
DEFINING MODIFIER 51 The additional procedure(s) or service(s) may be identified by appending modifier 51 to the additional procedure or service code(s).” In other words, modifier 51 reports that a physician performed two or more surgical services during one treatment session.
Is modifier 51 a facility modifier?
modifier 51 was designed for physicians, if you are coding for a physician then yes. if you are coding for the facility then the applicable outpatient hosp modifiers are on the inside front cover of the 2008 CPT Professional Edition, left column.
Why is modifier 51 exempt from the medicine section?
Carriers already assume during a hospital stay that multiple procedures will already be performed therefore designation of the exact nature and type of services rendered by the attending physician will still suffice for hospital medical billing claims. …Does Medicare accept modifier 51?
Medicare does not recommend reporting Modifier 51 on your claim; the processing system has hard-coded logic to append the modifier to the correct procedure code.
When verifying if a CPT code is modifier 51 exempt what appendix would you use?
You can find a full list of “add-on” and “modifier 51” exempt procedures in Appendices D and E of the CPT® codebook.
Can modifier 51 and 59 be billed together?
Never use both modifier 51 and 59 on a single procedure code. If there is a second location procedure (such as a HCPCS code for right or left), use the CPT® modifier first.
Does 51 modifier reduce RVU?
In another variation, some employers apply a 50% work RVU reduction to services with modifiers 50 and 51, but do not apply a work RVU reduction to procedures with modifier 59.Which CPT symbol conveys codes which are modifier 51 exempt?
The prohibition sign symbol is used to report codes that are exempt from modifier -51, but have not been designated as add-on procedures or services.
Which modifier should not be reported by anesthesiologists?Modifier 47 is considered invalid when appended to CPT codes describing anesthesia services (00100-01999).
Article first time published onWhat modifier identifies an anesthesia service that was performed personally by an anesthesiologist?
ModifierDescriptionAAAnesthesia services personally performed by the anesthesiologistADSupervision, more than four proceduresQKMedical direction of two, three, or four concurrent anesthesia proceduresQXQualified non-physician anesthetist with medical direction by a physician
How do you use CPT modifiers?
CPT modifiers are added to the end of a CPT code with a hyphen. In the case of more than one modifier, you code the “functional” modifier first, and the “informational” modifier second.
What does Hcpcs stand for?
The Healthcare Common procedure Coding System (HCPCS) is divided into two principal subsystems, referred to as level I and level II of the HCPCS.
What procedure is exempt from modifier 51?
Modifier 51 can be used with other modifiers, when appropriate, except modifier 50. Patient with bilateral simple mastectomies (19303, 19303-50) would not be billed with modifier 51.
Can you bill modifier 50 and 51 together?
Yes, modifiers 50 and 51 can be used together. Most payers and clearinghouses remove modifier 51, because their systems automatically calculate the 50% reduction based on RVU ranking, whether the practice applies mod 51 or not.
When should KX modifier be used?
The KX modifier should only be used when the therapist (not the biller or the billing company) has made a determination that skilled therapy is medically necessary over the $1920 therapy caps.
Does modifier 59 affect reimbursement?
The 59 modifier allows for reduction because each procedure contains the reimbursement for the prep as well as the procedure. The 59 says this procedure is performed in the same session, there for the prep is then carved out of the reimbursement or as we say discounted.
Which modifier goes first 59 or GP?
Always add 26 before any other modifier. If you have two payment modifiers, a common one is 51 and 59, enter 59 in the first position.
How many main sections does the CPT codebook have?
The six sections of the CPT codebook are, in order: Evaluation and Management. Anesthesiology. Surgery.
What organization is responsible for updating CPT codes?
The CPT® Editorial Panel is responsible for maintaining the CPT code set. The panel is authorized by the AMA Board of Trustees to revise, update, or modify CPT codes, descriptors, rules and guidelines. The panel is composed of 17 members.
Which CPT modifier stands for reduced services?
Modifier 52 is outlined for use with surgical or diagnostic CPT codes in order to indicate reduced or eliminated services. This means modifier 52 should be applied to CPTs which represent diagnostic or surgical services that were reduced by the provider by choice.
What are the two ways codes are reported for outpatient services?
What are the two ways codes are reported for outpatient services? HCPCS codes (CPT® and HCPCS Level II) are assigned either by using the CDM (usually for nonsurgical services and supplies) or manually by the coding staff (usually for surgeries, ED visits, and other interventional procedures).
What services are included in the surgical global package?
The global surgical package concept includes the pre-operative, intra-operative and post-operative services, and are considered included in the specific CPT code.
What Association publishes the CPT?
The CPT codes are maintained and updated annually by the American Medical Association (AMA). CPT copyright 2019 American Medical Association. All rights reserved. CPT is a registered trademark of the American Medical Association.
What procedure has the highest RVU?
For example, Whipple procedure (52.8 RVUs) had the highest 30-day overall morbidity and frequency of SAEs (45% and 35%, respectively), while trans-hiatal esophagectomy (44.2 RVUs) had the second highest (32% and 21%, respectively), and partial hepatectomy (39 RVUs) had the third highest (25% and 22% respectively).
Does modifier reduce payment?
Yes, modifier 51 causes a 50% reduction in payment.
What is the correct code for a total ankle arthroplasty with an implant?
Total ankle arthroplasty includes cpt code 27700-27703. Ankle arthroplasty is an alternative to ankle arthrodesis (fusion) for the treatment of end-stage ankle osteoarthritis. The physician performs arthroplasty to correct joint problems caused by arthritis.
Is it true that a physician who personally administers the anesthesia?
Anesthesiologists may personally perform anesthesia services or may supervise anesthesia services performed by a CRNA or AA. CRNAs may perform anesthesia services independently or under the supervision of an anesthesiologist or operating practitioner.
What modifiers are used for anesthesia?
Modifiers are two-character indicators used to modify payment of a procedure code or otherwise identify the detail on a claim. Every anesthesia procedure billed to OWCP must include one of the following anesthesia modifiers: AA, QY, QK, AD, QX or QZ.
Where are anesthesia modifiers located?
Anesthesia modifiers are used to receive the correct payment of anesthesia services. Pricing modifiers must be placed in the first modifier field to ensure proper payment ( , AD, QK, QX, QY, and QZ).
How much reimbursement will the claim receive when modifier QZ is reported?
Claims submitted with modifier QZ are reimbursed at 100 percent. When providing anesthesia services, anesthesiologist assistants (AAs) must work with anesthesiologist oversight – as specified under the laws of the state where the anesthesiologist and AA practice.