Who modified Mallampati score
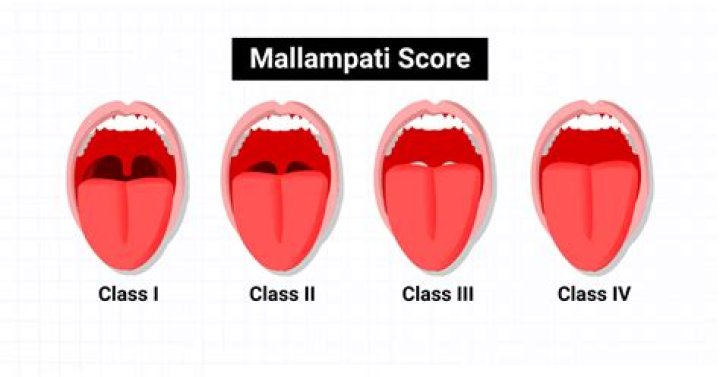
The original Mallampati Classification had three classes of visualization, but a fourth was later added by Samsoon and Young (1987) and shown to have greater predictive value, and is the version most commonly used today.
Is named after the Indian born American anaesthesiologist seshagiri Mallampati?
In anesthesia, the Mallampati score or Mallampati classification, named after the Indian anaesthesiologist Seshagiri Mallampati, is used to predict the ease of endotracheal intubation.
How do you score on Mallampati?
Mallampati Classification This test is performed while the patient is in the sitting position, awake and cooperative. Simply have the patient open their mouth and stick out their tongue and assess based upon the pharyngeal structures that are visible. This may not always be possible to accomplish in our patients.
What is the Mallampati score used for?
One of the clinical tests most widely used by the anaesthetists during preoperative physical examination is the Mallampati score (MS) 5. The goal is to assess whether the upper airways may be seen easily during tracheal intubation. The higher the score, the higher the risk of a difficult intubation.What is Mallampati class1?
According to the Mallampati scale, class I is present when the soft palate, uvula, and pillars are visible; class II when the soft palate and the uvula are visible; class III when only the soft palate and base of the uvula are visible; and class IV when only the hard palate is visible.
What does the B in burp stand for?
4–6. Applying backward, upward, rightward, and posterior pressure on the larynx (i.e., displacement of the larynx in the backward and upward directions with rightward pressure on the thyroid cartilage) is called the “BURP” maneuver and has been well described by Knill.
What is Friedman tongue position?
The Friedman Tongue Position (FTP) is a grading system used to assess the relationship of the palate to the tongue and is frequently utilized in the preoperative evaluation of patients with OSA. The tongue is evaluated in a neutral position within the oral cavity.
How do you intubate?
Applying firm, steady upward pressure at a 45-degree angle, the curved laryngoscope is used to lift the epiglottis and expose the vocal cords. Once the glottis is visualized, the operator will ask the respiratory assistant to place the endotracheal tube with the malleable stylet on the operator’s right hand.What is a Class 2 airway?
Keeping score with ‘class’ If you see a lot of room and can visualize the soft palate, uvula, the faucial pillars (the arches over the tonsils), and soft palate that is a Mallampati Class 1. If you see only see the soft palate, uvula, and faucial pillars, that’s a Class 2.
What causes Mallampati 4?A Mallampati score of III or IV is typically indicative of a higher rate of obstruction in airway as a result of enlarged tonsils or adenoids and poor Myofunctional activity (swallowing pattern and tongue position at rest) and tongue-tie.
Article first time published onWhat is UPPP surgery?
Uvulopalatopharyngoplasty (UPPP) is a procedure that removes excess tissue in the throat to make the airway wider. This sometimes can allow air to move through the throat more easily when you breathe, reducing the severity of obstructive sleep apnea (OSA).
What is measured in polysomnography?
Polysomnography, also called a sleep study, is a comprehensive test used to diagnose sleep disorders. Polysomnography records your brain waves, the oxygen level in your blood, heart rate and breathing, as well as eye and leg movements during the study.
How do you stage tonsils?
Stage 1 corresponds to palate grade 1 or 2 with tonsil grade III or IV. In stage 2, the palate grade is 1 or 2 with a tonsil grade I or II or a palate grade 3 or 4 with a tonsil grade III or IV. Stage 3 corresponds to palate grade 3 or 4 with tonsil grade I or II.
How do you perform RSI?
- Plan.
- Preparation (drugs, equipment, people, place)
- Protect the cervical spine.
- Positioning (some do this after paralysis and induction)
- Preoxygenation.
- Pretreatment (optional; e.g. atropine, fentanyl and lignocaine)
- Paralysis and Induction.
- Placement with proof.
What is an awake intubation?
Awake intubation is placing an endotracheal tube in the trachea while the patient continues to breathe. The principle advantage over RSI is that you do not take away the patient’s respirations or airway reflexes, which makes the process safer in many circumstances.
What is a Combitube airway?
The Combitube is a twin lumen device designed for use in emergency situations and difficult airways. It can be inserted without the need for visualization into the oropharynx, and usually enters the esophagus.
What is a physical status?
The ASA physical status classification system is a system for assessing the fitness of patients before surgery. In 1963 the American Society of Anesthesiologists (ASA) adopted the five-category physical status classification system; a sixth category was later added. These are: Healthy person.
What is the difference between tracheostomy and intubation?
An endotracheal tube is an example of an artificial airway. A tracheostomy is another type of artificial airway. The word intubation means to “insert a tube”. Usually, the word intubation is used in reference to the insertion of an endotracheal tube (Image 1).
What is the difference between a ventilator and a respirator?
Your doctor might call it a “mechanical ventilator.” People also often refer to it as a “breathing machine” or “respirator.” Technically, a respirator is a mask that medical workers wear when they care for someone with a contagious illness. A ventilator is a bedside machine with tubes that connect to your airways.
Is intubation life support?
“Intubating a patient and putting them on a ventilator to help them breathe definitely means they are being put on life support, which is very scary to think about when it’s you or your loved one needing that treatment.”
Can tonsils grow back?
It is possible for tonsils to partially grow back. During a tonsillectomy, most of the tonsils are removed. However, some tissue often remains, so tonsils occasionally can regenerate (regrow) — although they probably won’t grow back completely or to their original size.
Can you talk after UPPP?
After the surgery, you will be taken to a room to wake up from the anesthesia. At first, your throat will feel very sore. It will be hard to talk and swallow. You may also feel sleepy and nauseated.
Can you talk without a uvula?
The authors hypothesized that because the uvula and the ability to speak set humans apart from other mammals, the uvula might have a role in the speech process. An acquired absent uvula may be secondary to surgery or cultural practices, or it may be a complication of infection.
What does Mslt stand for?
In the multiple sleep latency test (MSLT), a person is given 4-5 opportunities to sleep every two hours during normal wake times. The specialist uses the test to measure the extent of daytime sleepiness (how fast the patient falls asleep in each nap, also called sleep latency), and also how quickly REM sleep begins.
What is PSG data?
Polysomnography (PSG) is a study or test done while you’re fully asleep. A doctor will observe you as you sleep, record data about your sleep patterns, and may identify any sleep disorders. During a PSG, the doctor will measure the following to help chart your sleep cycles: brain waves.
What is the scientific term for sleep?
The word “somnolence” is derived from the Latin “somnus” meaning “sleep”.
What grade are kissing tonsils?
Tonsil volume was classified according to validated criteria2 as follows: grade 1, tonsils in the tonsillar fossa barely seen behind the anterior pillar; grade 2, tonsils visible behind the anterior pillar; grade 3, tonsils extended three-quarters of the way to medline; grade 4, tonsils completely obstructing the …
What does size 3 tonsils mean?
Tonsils are graded on a scale from 0 to 4. Zero means you’ve had them removed, 1 means they’re barely visible, 2 means they’re normal, 3 means they’re large and just about touching that thing that hangs down at the back of your throat called the uvula, and 4 means they’re ginormous.
Do tonsils fall out?
The good news is that most tonsil stones will fall out on their own without causing much fuss. You may not even notice them until one day, you feel as if you’ve swallowed something unexpected.